Milroy Disease
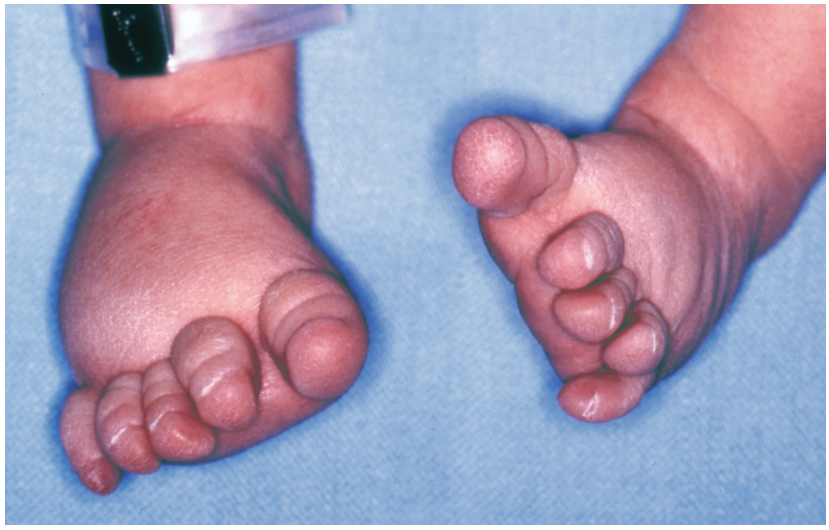
A male infant was delivered at term to a 24-year-old woman (gravida 3, para 1). The pregnancy had been uncomplicated; the vaginal delivery was normal. Apgar scores were 7 at 1 minute and 9 at 5 minutes. Birth weight was 3020 g (6 lb 11 oz); length, 51 cm (20 in); and head circumference, 36 cm (14 in).
Nonpitting edema of both feet was noted at birth; all other physical examination findings were normal. A review of the family history revealed that the child’s father and paternal grandfather had lymphedema of both feet at birth.
Milroy disease was diagnosed. This is an autosomal dominant inherited form of lymphedema, with onset at or near birth.
Inadequate lymphatic drainage that causes lymphedema may be attributed to congenital lymphatic hypoplasia or to structural damage to lymphatic vessels. Congenital lymphatic hypoplasia is associated with Milroy disease, Turner syndrome, Noonan syndrome, yellow nail syndrome, lymphedema praecox, and distichiasis. Damage to the lymphatic vessels can occur from surgery, trauma, neoplasms, radiation therapy, and chronic lymphangitis caused by filariasis or lymphogranuloma venereum.
There is no specific therapy for Milroy disease. Affected limbs should be elevated whenever possible. If skin sepsis occurs, prompt treatment is necessary to prevent further lymphatic insufficiency. Over time, fibrosis develops in the interstitial tissues and the skin may become thickened and pigmented. Skin ulcers can occur at sites of pressure.
FOR MORE INFORMATION:
•Leung AK, Robson WL. Oedema in childhood. J R Soc Health. 2000;120:212-219.


