Lumps and Bumps in Children: Musculoskeletal Lesions
Popliteal Cyst
 A 17-year-old boy presented with a fluctuant, cystic mass on the posterior aspect of the left knee. He had recurrent pain in this knee for the past 4 months. There was no history of trauma.
A 17-year-old boy presented with a fluctuant, cystic mass on the posterior aspect of the left knee. He had recurrent pain in this knee for the past 4 months. There was no history of trauma.
A diagnosis of popliteal cyst (also known as Baker cyst) was made after clinical examination of the lesion. A popliteal cyst forms when the synovial fluid from the knee joint fills and distends the gastrocnemio-semimembranous bursa in the popliteal area.1 The cyst is called “primary” when there is a valvular connection with the joint cavity, impeding reflux of synovial fluid from the cyst into the joint, and no knee derangement. The vast majority of primary cysts are found in children and young adults and are usually asymptomatic. In contrast, the cyst is called “secondary” when it communicates freely with the joint cavity and is associated with an intra-articular lesion. Secondary cysts occur mainly in adults.2 Meniscal tears account for at least 75% of these lesions.2 Other causes include osteoarthritis, rheumatoid arthritis, and infectious arthritis.1,2 In children, popliteal cysts may occur in patients with juvenile rheumatoid arthritis and benign joint hypermobility syndrome.1 Standard radiographs, ultrasonography, CT, and MRI can be useful in the evaluation of popliteal cysts.
The underlying cause should be treated if possible. Most popliteal cysts in children regress spontaneously or after successful treatment of the underlying lesion.1 For cysts that persist after treatment and that are symptomatic, options include aspiration, corticosteroid injection, simple open resection, and arthro-scopic treatment. The latter has the merit of simultaneously correcting both the valvular opening (by re-establishing a normal bidirectional communication) and the associated intra-articular pathology (eg, removal of loose body, partial meniscectomy, or chondroplasty) responsible for the persistence of the cyst.2-4 In addition, arthroscopic treatment has the lowest recurrence rate and is the treatment of choice.2-4
REFERENCES:
1. Neubauer H, Morbach H, Schwarz T, et al. Popliteal cysts in paediatric patients: clinical characteristics and imaging features on ultrasound and MRI. Arthritis. 2011;2011:751593.
2. Lie CW, Ng TP. Arthroscopic treatment of popliteal cyst. Hong Kong Med J. 2011;17:180-183.
3. Ahn JH, Lee SH, Yoo JC, et al. Arthroscopic treatment of popliteal cyst: clinical and magnetic resonance imaging results. Arthroscopy. 2010;26:1340-1347.
4. Froelich JM, Hillard-Sembell D. Symptomatic loose bodies of the knee located in a popliteal cyst.Orthopedics. 2009;32:918.
Ganglion
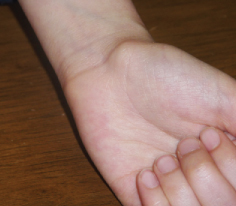 A 16-year-old girl was noted to have a mass at the ventral aspect of the left wrist. She could not recall when the mass first appeared. It was painless and tensely cystic. There was no history of trauma, decreased wrist motility, or weakness of the hand.
A 16-year-old girl was noted to have a mass at the ventral aspect of the left wrist. She could not recall when the mass first appeared. It was painless and tensely cystic. There was no history of trauma, decreased wrist motility, or weakness of the hand.
A ganglion is a cystic swelling that typically arises from the synovium of either a joint capsule or tendon sheath. The cyst contains a clear, gelatinous, colloid material, or a thick mucinous fluid. The latter contains hyaluronic acid and other mucopolysaccharides.1 The fluid is surrounded by a dense network of collagen fibres and fibrocytes.1 The most common sites include the dorsum of the wrist and the dorsum of the foot, although ganglion cysts may occur throughout the body. Ganglion cysts seldom emanate from within the joint itself; the incidence of intra-articular lesions has been reported to be 0.2% to 1.6% on MRI.2
Ganglia are often asymptomatic. Occasionally, there might be localized pain, paresthesia, limitation of motion, or weakness of the involved area.1 The condition can be complicated by carpal tunnel syndrome.3
Most ganglia resolve spontaneously. Treatment with needle aspiration or surgical excision is indicated only when the ganglion is large, causes pain, or interferes with normal tendon function.
REFERENCES:
1. Sloane J, Gulati V, Penna S, et al. Large intra-articular anterior cruciate ligament ganglion cyst, presenting with inability to flex the knee. Case Report Med. 2010;2010:705919.
2. Derman P, Kamath AF, Kelly Iv JD. Ganglion cysts of the posterior cruciate ligament. Am J Orthop (Belle Mead NJ). 2011;40:257-258.
3. Shimizu A, Ikeda M, Kobayashi Y, et al. Carpal tunnel syndrome caused by a ganglion in the carpal tunnel with an atypical type of palsy: a case report. Hand Surg. 2011;16:339-341.
Infrapatellar Bursitis
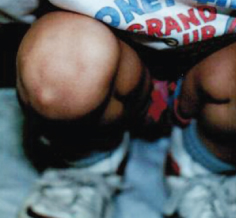 For 6 months, an 8-year-old boy had a cystic mass below the right patella. The mass was usually asymptomatic but occasionally became painful. It did not fluctuate in size. The child was very active in sport activities but had no history of associated injury or trauma. He was otherwise in good health. In particular, there was no history of recurrent fever, weight loss, or multiple joint swelling/pain.
For 6 months, an 8-year-old boy had a cystic mass below the right patella. The mass was usually asymptomatic but occasionally became painful. It did not fluctuate in size. The child was very active in sport activities but had no history of associated injury or trauma. He was otherwise in good health. In particular, there was no history of recurrent fever, weight loss, or multiple joint swelling/pain.
The infrapatellar bursa is located proximal to the insertion of the patellar tendon on the tibial tubercle. Inflammation may cause thickening of the synovial lining and fluid accumulation.1 Infrapatellar bursitis, also known as clergyman knee, usually affects persons who have continual mechanical strain and monotone movements of the patella.2 In children, infrapatellar bursitis may result from overuse of the knee extensor mechanism, particularly in runners or jumpers.1 It may also occur in association with juvenile idiopathic arthritis.1
Prevention and treatment consist of avoiding unnecessary kneeling and participating in strenuous exercise.2 If prolonged kneeling cannot be avoided, padding to cushion the knees should be considered. For those patients with severe pain, injection of the bursa with
lidocaine or a combination of lidocaine and corticosteroids may be beneficial.
For the child in this case, he and/or his parents may consider different, less strenuous activities to avoid aggravating the bursitis.
REFERENCES:
1. Alqanatish JT, Petty RE, Houghton KM, et al. Infrapatellar bursitis in children with juvenile idiopathic arthritis: a case series. Clin Rheumatol. 2011;30:263-267.
2. Kamper L, Haage P. Infrapatellar bursitis. N Engl J Med. 2008;359:2366.


