Lumps and Bumps in Children: Cysts

External Angular Dermoid Cyst
A 3-month-old girl was noted to have a cystic mass at the lateral angle of the orbit in the weeks after birth. She had been born via normal vaginal delivery after an uncomplicated pregnancy. There was no history of trauma.
A dermoid cyst is located at the outer end of the eyebrow or at the lateral angle of the orbit. External angular dermoid cysts are the most frequently encountered periorbital tumors in childhood.1,2 Dermoid cysts that involve the lateral eyebrow or eyelid account for more than 50% of these lesions in the head and neck.1 The cyst may cause a bony depression from pressure or may have a dumb-bell extension into the orbit. Histologically, the cyst is lined by epidermis with skin appendages. The central cavity contains keratin debris, hair, and sebum.
Rupture of the dermoid cyst into the subcutaneous tissue can create severe granulomatous inflammation. To prevent this possibility, and for cosmetic reasons, external angular dermoid cysts are usually excised. Traditional approaches involve an incision directly over the lesion, above, below, or through the eyebrow. To avoid the visible scar associated with eyebrow incision, an alternative approach is to enter through an upper eyelid crease.1
REFERENCES:
1. Cozzi DA, Mele E, d’Ambrosio G, et al. The eyelid crease approach to angular dermoid cysts in pediatric general surgery. J Pediatr Surg.2008;43(8):1502-1506.
2. Sreetharan V, Kangesu L, Sommerlad BC. Atypical congenital dermoids of the face: a 25-year experience. J Plast Reconst Aesthet Surg. 2007;60(9):1025-1029.
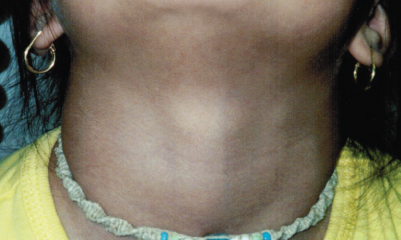
Thyroglossal Duct Cyst
This 13-year-old girl first noticed a painless lump in her neck about a year earlier. Physical examination showed a smooth, nontender mass in the midline of the anterior neck, at the level of the hyoid bone. The mass moved with swallowing and on protrusion of the tongue. The thyroid gland was in the normal position.
These findings are consistent with a thyroglossal duct cyst. Embryologically, the thyroid anlage arises from the foregut diverticulum at the site of the future foramen cecum at about the third week of gestation.1 The thyroid gland descends along the midline of the neck, between the first and second branchial arteries, and ventral to the hyoid bone and the developing laryngeal cartilage. The thyroid gland remains connected to the foramen cecum by the thyroglossal duct during the descent. The thyroglossal duct usually involutes during weeks 5 to 10 of gestation.2 A thyroglossal duct cyst results when the thyroglossal duct fails to involute.
Typically, a thyroglossal duct cyst presents as a painless midline neck mass that may move with swallowing and move upward with protrusion of the tongue.3 The mass is slightly mobile on palpation. However, its movement may be limited with protrusion of the tongue because of its persistent attachment to the foramen cecum.3 About 1% of the cysts are located laterally, often on the left side.4
A thyroglossal duct cyst can occur at any site along the normal pathway of descent from the foramen cecum to the lower neck region.3 The most common site is between the thyroid gland and the hyoid bone (61% of cases).5 Other potential locations include suprahyoidal (24%), suprasternal (13%), and intralingual (2%).4 Although thyroglossal duct cysts are congenital, these lesions rarely present in the neonatal period. More commonly, the cysts are noted in preschool children, sometimes after an upper respiratory tract infection.3 Up to 50% of the lesions are not diagnosed until the second decade of life.5 Some do not present until adulthood.1
Infection is the most common complication.1 Extrinsic airway compression and intralaryngeal extension, with resultant dyspnea or hoarseness, rarely occur.4 A lingual thyroglossal duct cyst might result in dysphagia, speech impairment, and ball-valve obstruction of the larynx.4 Malignant transformation during childhood is possible but rare.1 About 75% to 85% of thyroglossal duct malignancies are papillary adenocarcinomas.1,3
Ultrasonography can confirm the lesion’s cystic nature and the presence of a normal-appearing and normally situated thyroid gland.2 The ultrasonographic appearance of the lesion may be anechoic, homogeneously hypoechoic, or heterogeneous. If ultrasonography shows the absence of a normal thyroid gland and the midline swelling is solid, a radioisotope scan is appropriate to rule out ectopic thyroid gland.6 Three-dimensional CT is important for the diagnosis of a lingual thyroglossal duct cyst.7
The Sistrunk procedure is the surgical treatment of choice.2 It involves excision of the cyst, thyroglossal tract, and central portion of the hyoid bone to prevent recurrence.
REFERENCES:
1. Leung A. Thyroglossal duct cyst. In: Lang F, ed. The Encyclopedia of Molecular Mechanisms of Disease. Berlin: Springer-Verlag; 2009:2069-2070.
2. Hirshoren N, Neuman T, Udassin R, et al. The imperative of the Sistrunk operation: review of 160 thyroglossal tract remnant operations. Otolaryngol Head Neck Surg. 2009;140(3):338-342.
3. Leung A, Robson WL. Eight-year-old girl with mass in midline of neck. Consultant For Pediatricians. 2007;6(1):29-32.
4. Soliman AM, Lee JM. Imaging case study of the month. Thyroglossal duct cyst with intralaryngeal extension. Ann Otol Rhinol Laryngol. 2006;115(7):
559-562.
5. Türkyilmaz Z, Sönmez K, Karabulut R, et al. Management of thyroglossal duct cyst in children. Pediatr Int. 2004;46(1):77-80.
6. Khan RA, Mahajan JK, Rao KL. Thyroglossal duct cyst in children. Nuklearmedizin. 2009;48(4):N24-N25.
7. Bai W, Ji W, Wang L, Song Y. Diagnosis and treatment of lingual thyroglossal duct cyst in newborns. Pediatr Int. 2009;51(4):552-554.

Meibomian Cyst
The 2 masses one on each upper eyelid of a 9-year-old girl had been present for a year. They were asymptomatic. The child’s vision was normal.
The lesions are meibomian cysts or chalazia. A meibomian cyst is a localized lipogranulomatous inflammation that results from blockage of the meibomian gland by desquamated epithelial cells and/or lipid inspissation.1,2 It is the most common inflammatory lesion of the eyelid.1
Clinically, a meibomian cyst manifests as a firm, nontender nodule in the upper or lower eyelid. The condition is more common in the upper eyelid, where an increased number and length of meibomian glands are present.2 The cyst may occur externally as a lump on the skin, as in this patient, or internally as a lump beneath the conjunctiva. It is usually painless and nonerythematous but may be cosmetically unsightly and can become secondarily infected.
Meibomian cysts may be associated with meibomian gland dysfunction or chronic blepharitis.3 Rarely, an infected lesion may lead to preseptal cellulitis.4 If the lesion is large enough, it may cause visual problems, such as astigmatism by exerting pressure on the eyeball.5
About 80% of meibomian cysts resolve with conservative treatment, which consists of eyelid hygiene, twice daily warm compresses, and gentle lid massage.3,6 The massage is performed over the lesion, in the direction of the eyelashes.6 A topical antibiotic is used when the lesion is infected.
If the cyst fails to resolve with conservative treatment and is cosmetically unappealing, a surgical approach can considered. Intralesional corticosteroid injection has a success rate of 93% to 95%,2 but can be painful. In contrast, subcutaneous corticosteroid injection into the looser extralesional tissue results in less pain. Because skin depigmentation may occur at the injection site, subconjunctival rather than subcutaneous injection is preferred, especially in patients with darker skin complexion.5 Large lesions or lesions that fail to respond to 2 or 3 corticosteroid injections may require subconjunctival incision and curettage.7
REFERENCES:
1. Ozdal PC, Codère F, Callejo S, et al. Accuracy of the clinical diagnosis of chalazion. Eye (Lond). 2004;18(2):135-138.
2. Pavicic´-Astalos J, Ivekovic´ R, Knezevic´ T, et al. Intralesional triamcinolone acetonide injection for chalazion. Acta Clin Croat. 2010;49(1):43-48.
3. Mansour AM, Chan CC, Crawford MA, et al. Virus-induced chalazion. Eye (Lond). 2006;20(2):242-246.
4. Dubey R, Wang LW, Figueira EC, et al. Management of marginal chalazia: a surgical approach. Br J Ophthalmol. 2011;95(4):590,596-597.
5. Ben Simon GJ, Huang L, Nakra T, et al. Intralesional triamcinolone acetonide injection for primary and recurrent chalazia: is it really effective? Ophthalmology. 2005;112(5):913-917.
6. Gilchrist H, Lee G. Management of chalazia in general practice. Aust Fam Physician. 2009;38(5):311-314.
7. Duarte AF, Moreira E, Nogueira A, et al. Chalazion surgery: advantages of a subconjunctival approach. J Cosmet Laser Ther. 2009;11(3):154-156.


