Is Leg Bowing in This 3-Year-Old Girl Related to Obesity?
How Do You Read These Images?
 During a well-child check-up, the mother of a 3-year-old girl expresses concern about the way her daughter walks. She has noticed progressive bowing of the child’s legs over the past year. The child has had no leg trauma. There is no significant personal or family history.
During a well-child check-up, the mother of a 3-year-old girl expresses concern about the way her daughter walks. She has noticed progressive bowing of the child’s legs over the past year. The child has had no leg trauma. There is no significant personal or family history.
The girl is at the 30th percentile for height and the 95th percentile for weight. Mild genu varum is noted bilaterally and is more pronounced on weight bearing. Both wrists and other joints appear normal and have full range of motion. Remaining physical findings are unremarkable.
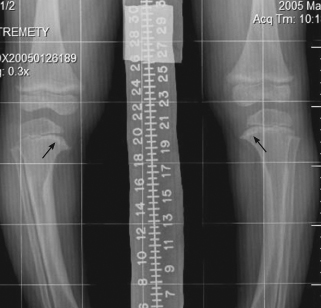
An anteroposterior view of both knees with weight bearing is shown.
What do you suspect?
A. Rickets.
B. Scurvy.
C. Physiologic bowing.
D. Blount disease.
E. Post-traumatic growth plate deformity.
(Answer and discussion on next page.)
 Answer: D, Blount disease
Answer: D, Blount disease
The radiograph shows bilateral genu varum deformity, with bowing and beaking of the medial metaphysis of the tibia. Reactive cortical thickening in the medial aspect of the tibial shaft is present bilaterally. These findings are suggestive of Blount disease.
Blount disease, or tibia vara, is a developmental abnormality that results from an anomalous endochondral ossification of the medial aspect of the tibial physis. Consequent undergrowth of the medial tibia leads to bowing. The cause of abnormal ossification is unknown; however, the strong association with childhood obesity implicates a mechanical mechanism. Bowing may also be physiologic (in children younger than 2 years) or be a result of rickets, renal osteodystrophy, skeletal dysplasia, and conditions that cause asymmetric physeal growth (eg, infection, fractures, and tumors).
Blount disease is classified into 2 broad categories based on age of onset: infantile and juvenile or adolescent. Early-onset disease occurs between 1 and 3 years of age and is more common. Late-onset disease is thought to be a consequence of premature fusion of the medial portion of the tibial growth plate. Blount disease in adolescents is often less aggressive and unilateral; in infants, it tends to be progressive and bilateral.
It is important to distinguish physiologic bowing from infantile Blount disease, which may lead to progressive deformity with gait deviation, limb length discrepancy, and premature arthritis of the knee. Physiologic bowing is usually symmetrical and improves with age. Persistent bowing after age 2 years or progression warrants further evaluation. Likewise, unilateral findings and/or lateral thrust of the knee with ambulation indicate a nonphysiologic cause. Physiologic bowing often presents with short stature and delayed ambulation, whereas Blount disease is typically associated with obesity and early walking and occurs in ambulatory patients. African American ethnicity and female gender are other well-established risk factors for this condition.
Radiographs are helpful in making the diagnosis. An anteroposterior standing radiograph of both extremities and lateral radiograph of the affected extremity are typically obtained. The findings include sloping and fragmentation of the medial epiphyseal ossification center, widening of the growth plate, and “beaking” of the medial metaphysis, as seen in this case. MRI is often helpful in evaluating the growth plate in adolescent Blount disease.
Management depends on the child’s age. Observation and serial clinical and radiographic examinations are recommended for children younger than 2 years when the diagnosis is uncertain. Children 3 years and younger are often treated with a knee-ankle-foot orthosis. Children 4 years and older and those for whom a 1-year trial of bracing is unsuccessful are surgically treated to realign the mechanical axis of the knee. Bracing is ineffective in adolescents with Blount disease. Surgical correction is also recommended before age 4 years for patients with progressive clinical and radiological findings, and impending closure of the medial tibial physis.
Rate of recurrence of the deformity is higher among adolescents and those treated after 4 years of age. Close follow-up is recommended until skeletal maturity is reached.
The patient described was treated with long-leg braces. After a year of use, the deformity significantly improved and the brace was discontinued.


