Jaw Pain, Tender Facial Rash, and Fever in a 7-Year-Old Girl
 HISTORY
HISTORY
A 7-year-old girl with a history of secondary adrenal insufficiency of unclear cause treated with replacement corticosteroid therapy had pain and swelling of the jaw for the past 4 days. She also had fever and a painful itchy rash with blisters on the right side of the face involving the upper lip, cheek, and forehead for the past 3 days. There were no sick contacts. Immunizations, including varicella vaccine, were up-to-date. She had not had chickenpox infection. Father had hypogammaglobulinemia and alopecia.
PHYSICAL EXAMINATION
Alert, well-nourished child with fever. Other vital signs normal. Tender erythematous rash on the right side of the face with vesicular lesions on upper lip, cheek, periorbital region, and forehead. Right eye swollen shut, with injected conjunctiva. Jaw swollen and tender on the right side. Oropharyngeal examination limited secondary to difficulty in opening mouth due to pain. No right ear tenderness. Hearing grossly intact.
Cardiac, respiratory, abdominal, and musculoskeletal findings within normal limits. No rash elsewhere. Higher neurological functions normal, no focal neurological deficits.
WHAT’S YOUR DIAGNOSIS?
(Answer on Next Page)
ANSWER: HERPES ZOSTER
The child was evaluated by specialists in neurology, infectious diseases, ophthalmology, endocrinology, and immunology. Direct fluorescent antibody testing of a skin lesion was positive for varicella zoster virus (VZV). Cerebrospinal fluid (CSF) obtained by lumbar puncture, obtained to determine treatment course, was suggestive of viral meningitis. Polymerase chain reaction analysis of CSF was positive for VZV.
ETIOLOGY
VZV causes primary, latent, and recurrent infections. The primary infection is manifested as chickenpox and results in establishment of a lifelong latent infection of sensory ganglion neurons.1 Reactivation of the latent VZV causes herpes zoster. Initial infection can be prevented by immunization with live-attenuated VZV vaccine.2 On the other hand, because varicella vaccine is a live-attenuated virus, herpes zoster may develop in a vaccine recipient, especially if the individual is immunocompromised.3
Herpes zoster is uncommon in childhood and is very rare in children younger than 10 years, with the exception of infants who were infected in utero or in the first year of life.4 However, children receiving immunosuppressive therapy and those who have HIV infection5 or other immunodeficiency disorder are at greater risk for herpes zoster.
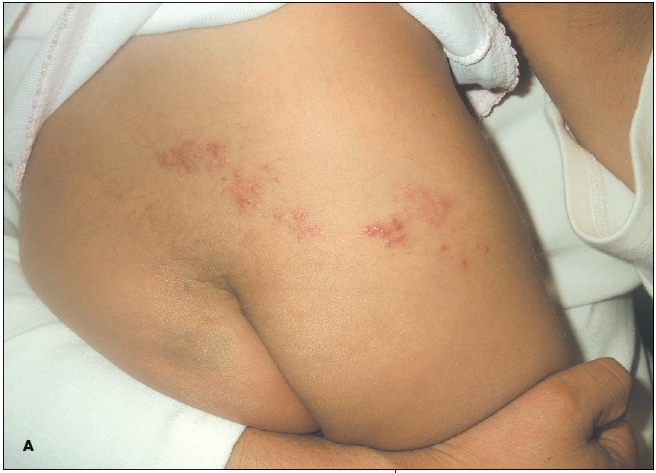
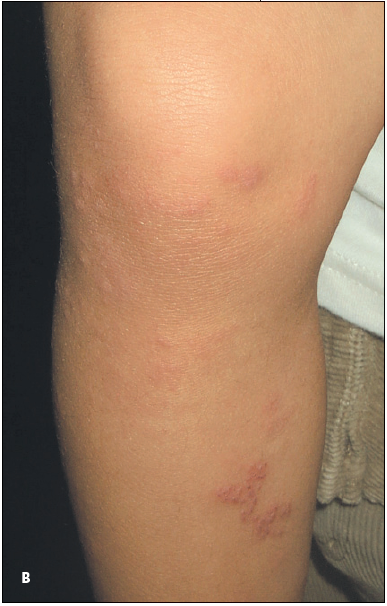
Figure – Herpes zoster in the sacral (A) and lower lum- bar (B) dermatomes in an otherwise healthy 22-month- old girl is shown. The child was up-to-date on all immunizations, including varicella vaccine, which she received at 12 months. She had not been exposed to chickenpox.
(Courtesy of Julie L. Cantatore-Francis, MD and Yelva Lynfield, MD.)
CLINICAL MANIFESTATIONS
Herpes zoster typically begins with burning pain and vesicular skin lesions clustered within 1 or, less commonly, 2 adjacent dermatomes.3 In young children, herpes zoster has a predilection for areas supplied by the cervical and sacral dermatomes (Figure), whereas in adults the lesions are more common in the lower thoracic and upper lumbar dermatomes.6 The illness in childhood is generally less severe than in adulthood. In children, the rash is mild with new lesions appearing over a few days; symptoms of acute neuritis are minimal and complete resolution usually occurs within 1 or 2 weeks.7
Immunocompromised children with herpes zoster may have more severe symptoms, including postherpetic neuralgia. They may also experience disseminated cutaneous disease as well as life-threatening visceral dissemination with pneumonia, hepatitis, encephalitis, and intravascular coagulopathy. Transverse myelitis with transient paralysis is a rare complication of herpes zoster.8
 EVALUATION
EVALUATION
VZV can be identified quickly by direct fluorescent antibody testing of cells from cutaneous lesions and by polymerase chain reaction testing. VZV IgG antibodies can be detected by several methods; a 4-fold rise in IgG antibodies is confirmatory of acute infection. VZV IgG antibody tests can also help determine the immune status of individuals whose clinical history of varicella is unknown or equivocal.9
Patients with either neurological complications of varicella or uncomplicated herpes zoster may have mild lymphocytic pleocytosis, a slight to moderate increase in protein levels, and normal to low glucose levels in the CSF.10
TREATMENT AND OUTCOME
In otherwise healthy children, treatment of uncomplicated herpes zoster may not always be necessary, although some experts treat with oral acyclovir. Patients at risk for disseminated disease should receive intravenous acyclovir.11 For children of any age who are immunocompromised or immunocompetent and require hospitalization, IV acyclovir, 30 mg/kg/d in 3 divided doses, is given for 7 to 10 days. For immunocompetent children older than 12 years who do not require hospitalization, PO acyclovir, 4000 mg/d in 5 divided doses, is given for 5 to 7 days.12
This child was treated with intravenous acyclovir for 14 days and 1 dose of intravenous immunoglobulin, because serum immunoglobulin levels were found to be low. She responded well to treatment. She is currently undergoing a work-up for immunodeficiency disorders, including common variable immunodeficiency.


