Infantile Hemangioma Significant Improvement With β-Blockers
A mother brought her healthy 8-week-old daughter to a pediatric office for the infant’s 2-month well-baby checkup. The girl had been delivered vaginally at term with no associated complications. She weighed 4.2 kg at presentation, and she had no family history of congenital disease or vascular disease. Physical examination findings were normal.
At the visit, the mother mentioned that she had noticed a prominent, clear discharge from the girl’s right eye for the preceding 2 weeks. A diagnosis of nasolacrimal duct obstruction was considered at the visit, but because of the girl’s constant discharge and parental anxiety, the patient was referred to a pediatric ophthalmologist for further evaluation.
When seen by theophthalmologist 3 weeks later, the infant had developed mild right exophthalmos. Magnetic resonance imaging (MRI) of the brain showed a capillary hemangioma, predominating at the inferolateral aspect of the right orbit, extending superiorly and medially, but not reaching the medial rectus or superior rectus muscles (Figure 1). It abutted the posterior and inferior aspect of the right globe but did not deform it (Figure 2). She was started on propranolol, 3 mg/kg/day initially then tapered to 2 mg/kg/day, with close follow-up.


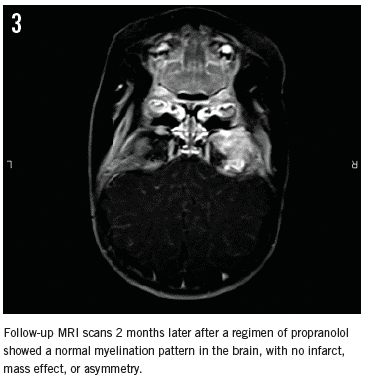
MRI results 2 months later showed a slight reduction in the bulk of the hemangioma (Figure 3). The exophthalmos mass effect related to the lesion on the right globe appeared to have improved after propranolol treatment. Nevertheless, since the MRI results did not show complete remission of the hemangioma, the regimen of propranolol 2 mg/kg/day was resumed. A follow-up MRI scan was to be done in 8 to 12 months.
Discussion
Infantile hemangiomas are benign vascular tumors characterized by very rapid growth. Capillary hemangiomas are among the most common orbital tumors in children, affecting 1% to 3% of newborns.1-3 Although they are usually self-limited, periocular hemangiomas can cause serious vision loss through the induction of strabismic, deprivational, or anisometropic amblyopia.
The lesions present predominantly in girls and typically appear at birth or within the first 2 months of life. The sites of predilection are the orbit, the eyelids, or both. Pure exophthalmos caused by a deep orbital tumor without an anterior component, as in our patient’s case, is relatively rare, occurring in as few as 9% of all periorbital hemangioma cases.4

A 2004 survey of members of American Association of Pediatric Ophthalmology and Strabismus showed that intralesional corticosteroid injection was the most commonly used treatment for periorbital capillary hemangiomas.5 Oral corticosteroids and excision also are common treatments for these periocular lesions.5-10
Surgical resection is reserved for severe cases,4,11-13 especially when the lesion is growing rapidly or is causing astigmatism, anisometropic amblyopia, or obscuration of the visual axis.2,14 The surgery should be performed at 13 months of age or earlier to reduce the amount of astigmatism. Surgical resection has been found to be very useful in relieving pupillary occlusion.15
The use of alternative therapies such as the interferons has been reported in select cases of periocular capillary hemangioma, especially in cases of life- or sight-threatening complications.3 A combination of low-dose cyclophosphamide with interferon alfa-2a for a short time induced early and lasting regression of orbital juvenile capillary hemangiomas with minimal side effects in one case series study.16 All of these treatments could have severe adverse effects or complications.
In 2008, Léauté-Labrèze and Taïeb reported that some patients being treated with β-blockers for cardiac indications had an incidental finding of rapid regression of their hemangiomas.17 Since then, increasing use of β-blockers in the treatment of capillary hemangiomas has been reported.18-24 One retrospective observational case series25 showed an average of 7.1 months of oral propranolol treatment of 5 patients with infantile hemangioma significantly reduced the size of the hemangioma in 4 of the patients without significant adverse events. Other authors have reported similar results.26,27
Some authors have proposed the use propranolol as first-line therapy for severe periocular hemangiomas instead of traditional corticosteroid treatment.28 A 2011 comprehensive review29 showed that propranolol had been used as first-line treatment in 50 of 85 cases, with the most common dosage being 2 mg/kg/day. Minor adverse reactions such as bradycardia occurred in one-third of cases. Recurrence was observed in one-fifth of cases. Topical application of a β-blocker such as timolol, 0.5%, also has been shown to be effective.30,31
Ultrasonography and color Doppler imaging are useful modalities in the diagnosis of intraorbital and periorbital hemangiomas.32 However, MRI is a more important and complementary study for the delineation and diagnosis of malformations.33 In addition, MRI is very helpful for choosing the appropriate clinical approach (oral medication, local injection, or surgery) and follow-up.34
Wang Li, MD, PhD, is chief resident in the Department of Family and Community Medicine at the School of Medicine at Texas Tech University Health Sciences Center at the Permian Basin in Odessa, Texas.
Bhargavi B. Kola, MD, is the assistant medical director and an assistant professor in the Department of at the School of Medicine at Texas Tech University Health Sciences Center at the Permian Basin in Odessa, Texas.
Bhavana Y. Mocherla, MD, is a resident in the Department of Family and Community Medicine at the School of Medicine at Texas Tech University Health Sciences Center at the Permian Basin in Odessa, Texas.
George Rodenko, MD, is a radiologist in the Department of Radiology at Medical Center Hospital in Odessa, Texas.
References
- Haik BG, Karcioglu ZA, Gordon RA, Pechous BP. Capillary hemangioma (infantile periocular hemangioma). Surv Ophthalmol. 1994;38(5):399-426.
- Slaughter K, Sullivan T, Boulton J, O’Reagan P, Gole G. Early surgical intervention as definitive treatment for ocular adnexal capillary haemangioma. Clin Experiment Ophthalmol. 2003;31(5):418-423.
- Teske S, Ohlrich SJ, Gole G, Spiro P, Miller M, Sullivan TJ. Treatment of orbital capillary haemangioma with interferon. Aust N Z J Ophthalmol. 1994;22(1):13-17.
- Haik BG, Jakobiec FA, Ellsworth RM, Jones IS. Capillary hemangioma of the lids and orbit: an analysis of the clinical features and therapeutic results in 101 cases. Ophthalmology. 1979;86(5):760-792.
- Wasserman BN, Medow NB, Homa-Palladino M, Hoehn ME. Treatment of periocular capillary hemangiomas. J AAPOS. 2004;8(2):175-181.
- Egbert JE, Paul S, Engel WK, Summers CG. High injection pressure during intralesional injection of corticosteroids into capillary hemangiomas. Arch Ophthalmol. 2001;119(5):677-683.
- Friling R, Axer-Siegel R, Ben-Amitai D, Goldenberg-Cohen N, Weinberger D, Snir M. Intralesional and sub-Tenon’s infusion of corticosteroids for treatment of refractory periorbital and orbital capillary haemangioma. Eye (Lond). 2009;23(6):1302-1307.
- Neumann D, Isenberg SJ, Rosenbaum AL, Goldberg RA, Jotterand VH. Ultrasonographically guided injection of corticosteroids for the treatment of retroseptal capillary hemangiomas in infants. J AAPOS. 1997;1(1):34-40.
- Verity DH, Rose GE, Restori M. The effect of intralesional steroid injections on the volume and blood flow in periocular capillary haemangiomas. Orbit. 2008;27(1):41-47.
- Weiss AH, Kelly JP. Reappraisal of astigmatism induced by periocular capillary hemangioma and treatment with intralesional corticosteroid injection. Ophthalmology. 2008;115(2):390-397.e1.
- Aldave AJ, Shields CL, Shields JA. Surgical excision of selected amblyogenic periorbital capillary hemangiomas. Ophthalmic Surg Lasers. 1999;30(9):754-757.
- Günalp I, Gündüz K. Vascular tumors of the orbit. Doc Ophthalmol. 1995; 89(4):337-345.
- Walker RS, Custer PL, Nerad JA. Surgical excision of periorbital capillary hemangiomas. Ophthalmology. 1994;101(8):1333-1340.
- Tronina SA, Bobrova NF, Khrinenko VP. Combined surgical method of orbital and periorbital hemangioma treatment in infants. Orbit. 2008;27(4):249-257.
- Levi M, Schwartz S, Blei F, et al. Surgical treatment of capillary hemangiomas causing amblyopia. J AAPOS. 2007;11(3):230-234.
- Wilson MW, Hoehn ME, Haik BG, Rieman M, Reiss U. Low-dose cyclophosphamide and interferon alfa 2a for the treatment of capillary hemangioma of the orbit. Ophthalmology. 2007;114(5):1007-1011.
- Léauté-Labrèze C, Taïeb A. Efficacy of beta-blockers in infantile capillary hemangiomas: the physiopathological significance and therapeutic consequences [in French]. Ann Dermatol Venereol. 2008;135(12):860-862.
- Cloke A, Lim LT, Blaikie A. Capillary haemangioma successfully treated with oral beta-blocker in Dar es Salaam, Tanzania: a case report. Semin Ophthalmol. 2013;28(1):32-33.
- Cruz OA, Siegfried EC. Propranolol treatment for periocular capillary hemangiomas. J AAPOS. 2010;14(3):199-200.
- Claerhout I, Buijsrogge M, Delbeke P, et al. The use of propranolol in the treatment of periocular infantile haemangiomas: a review. Br J Ophthalmol. 2011;95(9):1199-1202.
- Mai C, Vega-Pérez A, Koch M, Bertelmann E. Successful treatment of orbital capillary hemangioma with propranolol [in German]. Ophthalmologe. 2011;108(4):364-367.
- Salazar-Murillo R, García-Pacheco S, González-Blanco MJ, Bolívar-Montesa P, Campos-García S. Propranolol: treatment of capillary hemangioma with orbital involvement [in Spanish]. Arch Soc Esp Oftalmol. 2012;87(12):411-414.
- Haider KM, Plager DA, Neely DE, Eikenberry J, Haggstrom A. Outpatient treatment of periocular infantile hemangiomas with oral propranolol. J AAPOS. 2010;14(3):251-256.
- Taban M, Goldberg RA. Propranolol for orbital hemangioma. Ophthalmology. 2010;117(1):195-195.e4.
- Fridman G, Grieser E, Hill R, Khuddus N, Bersani T, Slonim C. Propranolol for the treatment of orbital infantile hemangiomas. Ophthal Plast Reconstr Surg. 2011;27(3):190-194.
- Missoi TG, Lueder GT, Gilbertson K, Bayliss SJ. Oral propranolol for treatment of periocular infantile hemangiomas. Arch Ophthalmol. 2011;129(7):899-903.
- Snir M, Reich U, Siegel R, et al. Refractive and structural changes in infantile periocular capillary haemangioma treated with propranolol. Eye (Lond). 2011;25(12):1627-1634.
- Thoumazet F, Léauté-Labrèze C, Colin J, Mortemousque B. Efficacy of systemic propranolol for severe infantile haemangioma of the orbit and eyelid: a case study of eight patients. Br J Ophthalmol. 2012;96(3):370-374.
- Spiteri Cornish K, Reddy AR. The use of propranolol in the management of periocular capillary haemangioma—a systematic review. Eye (Lond). 2011;25(10):1277-1283.
- Xue K, Hildebrand GD. Deep periocular infantile capillary hemangiomas responding to topical application of timolol maleate, 0.5%, drops. JAMA Ophthalmol. 2013;131(9):1246-1248.
- Sloan B, Mora J, Dai S. Everything old is new again. Clin Experiment Ophthalmol. 2010;38(6):545-546.
- Neudorfer M, Leibovitch I, Stolovitch C, et al. Intraorbital and periorbital tumors in children—value of ultrasound and color Doppler imaging in the differential diagnosis. Am J Ophthalmol. 2004;137(6):1065-1072.
- Gelbert F, Riche MC, Reizine D, et al. MR imaging of head and neck vascular malformations. J Magn Reson Imaging. 1991;1(5):579-584.
- Orhan S, Durak AC, Mavili E, Akdemir H. MRI findings of orbital hemangiomas [in Turkish]. Tani Girisim Radyol. 2004;10(1):26-30.


