Girl With Abdominal Pain, Headache, and Purple-Blue Nodules
What’s Your Diagnosis?
Sharpen Your Physical Diagnostic Skills
 HISTORY
HISTORY
A 7-year-old girl presented to the emergency department with a subjective fever, nonradiating right upper quadrant abdominal pain, dizziness, generalized headache, blurry vision, and photophobia of 6 days’ duration. Her mother reported that the child had been uncharacteristically pale for the past 2 weeks and had decreased appetite, fatigue, and rapid breathing but no hematemesis, hematochezia, melena, epistaxis, or bruising.
Birth history unremarkable, no neonatal complications. Early development normal. Child underwent surgical removal of several skin lesions from her right hip, right thigh, and right forearm at a different institution 3 years earlier. Family history notable for iron deficiency anemia in the mother. Child’s diet, while varied, significant for excessive cow’s milk intake.
PHYSICAL EXAMINATION
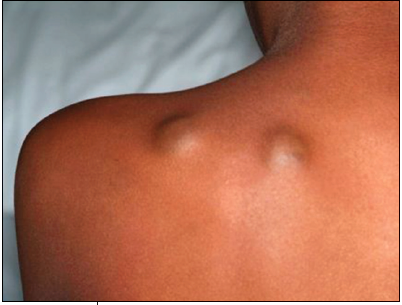
Temperature, 37.6ºC (99.6ºF); heart rate, 88 beats per minute; blood pressure, 112/50 mm Hg; respiration rate, 18 breaths per minute; and pulse oximetry, 99% while on room air. Child had rhinorrhea, mild right upper quadrant abdominal tenderness on palpation, generalized pallor, and grade 2/6 functional systolic murmur. Purple-blue, rubbery subcutaneous nodule noted on the right anterior chest and 2 similar nodules on the back over the left scapula, shown here. Lesions were mobile, tender, compressible, and nonpulsatile. According to the mother, these nodules were similar to the ones that were surgically removed.
IMAGING FINDINGS
CT scan of the head showed no intracranial hemorrhage, hydrocephalus, or shifting of the ventricles.
LABORATORY RESULTS
Hemoglobin level, 2.4 g/dL; hematocrit, 7.6%; red blood cell count, 1.39 3 106/μL; mean corpuscular volume, 54.7 fL, mean corpuscular hemoglobin, 17.2 pg/cell; red cell distribution width, 21.6%; platelet count, 189,000/μL. In view of the severe symptomatic anemia, emergent transfusion was performed.
Iron studies obtained after transfusion showed ferritin, 28 ng/mL (normal, 7 to 140 ng/mL); iron, 112 μg/dL (normal, 50 to 120 μg/dL); total iron-binding capacity, 341 μg/dL (normal, 250 to 425 μg/dL); and iron saturation, 32.8%.
Results of fecal occult blood testing initially negative.
WHAT’S YOUR DIAGNOSIS?
Answer on next page
 What’s Your Diagnosis?
What’s Your Diagnosis?
ANSWER: BLUE RUBBER BLEB NEVUS SYNDROME
The child was admitted to the pediatric ICU and received blood transfusions and oral iron supplementation. Several days after admission, results of fecal occult blood testing were positive. The severe hypochromic, microcytic anemia and rubbery, mobile nodules led to a preliminary diagnosis of blue rubber bleb nevus syndrome (BRBNS).
Upper endoscopy identified 2 lesions in the body of the stomach at the greater curvature and 1 lesion at the cardiac of the stomach (Figure). The first and second portions of the duodenum appeared normal. Lower endoscopy of the large bowel and distal terminal ileum revealed a normal vascular pattern, with no vascular or polypoid lesions.
 Chest ultrasonography revealed 2 ovoid lesions, of 2.3 X 2.1 cm and 1.8 X 1.2 cm, in the superficial soft tissue overlying the left scapula. Ultrasonography of the pelvis showed a similar heterogeneous lesion of 2.1 X 1.6 cm in the right buttock. The lesions were thought to be consistent with hemangiomas. Ultrasonography of the abdomen detected a small calcification in the lateral aspect of the hepatic lobe, representative a small vascular malformation.
Chest ultrasonography revealed 2 ovoid lesions, of 2.3 X 2.1 cm and 1.8 X 1.2 cm, in the superficial soft tissue overlying the left scapula. Ultrasonography of the pelvis showed a similar heterogeneous lesion of 2.1 X 1.6 cm in the right buttock. The lesions were thought to be consistent with hemangiomas. Ultrasonography of the abdomen detected a small calcification in the lateral aspect of the hepatic lobe, representative a small vascular malformation.
MRI of the brain using postgadolinium contrast showed a focus of low-signal T1 and increased T2 within the white matter at the right centrum semiovale region anteriorly, which was compatible with a small hemangioma.
Chest radiographs to rule out upper respiratory tract infection secondary to unremitting fevers were normal. Radiographs of the paranasal sinuses indicated some opacification of the ethmoidal sinuses. Sinusitis was diagnosed, and the child was treated with intravenous ceftriaxone. Sinusitis, if treated, is usually managed in the outpatient setting by oral antibiotics (commonly high-dose amoxicillin, amoxicillin/clavulanate, or third-generation cephalosporins). Because this patient was hospitalized at the time of her fever and the fever started several days after she was admitted, blood and urine samples were obtained for cultures. Empiric intravenous cephalosporin was given until these cultures were shown to be negative and the working diagnosis of sinusitis was confirmed. Over the next several days, her fever resolved. Evidence of mild sinusitis was also apparent on MRI of the brain.
BRBNS is associated with venous malformations of the skin and internal organs, particularly the GI tract; GI bleeding; and chronic anemia. This congenital disorder, first described by Gascoyen1 in 1860 and later named by Bean2 in 1958, is categorized into 3 types of angiomatous lesions. The first is a large, disfiguring cavernous angioma capable of displacing vital structures or causing obstruction. The second most common lesion is described as a blood sac similar to a “blue rubber nipple” covered in thin skin—consistent with the clinical features in this patient. The third is a blue to black irregular skin marking that unites with the surrounding normal skin in a series of color gradations.2
CLINICAL MANIFESTATIONS
BRBNS usually presents during infancy or childhood with the characteristic, 1- to 3-cm, cutaneous nevi on the trunk, limbs, or perineum; however, they may occur anywhere on the body.3 A few cases of adult-onset BRBNS have been reported.4 BRBNS affects all races, with males and females affected equally.5 An autosomal dominant pattern of inheritance has been reported in about 15% of cases, although most cases are sporadic, as in this patient.6,7 Malignant transformation has not been reported.8
In addition to the skin and GI tract, lesions may be found in the liver, spleen, eye, heart, lung, pleura, thyroid, parotid, skeletal muscle, joints/bones, genitalia,bladder, kidney, and CNS.3,4,9 CNS lesions are rarely reported in children.10 A review of the literature revealed that of 20 cases of BRBNS with lesions in the CNS, 30% involved children. In all of these cases, patients presented with seizures, psychomotor dysfunction, or developmental delay. This patient’s presentation was unique in that she had no history of neurological dysfunction. The cephalgia was probably secondary to her concurrent sinusitis, because it resolved along with the sinus infection after antibiotic treatment.
The anemia and GI bleeding associated with BRBNS often present in late childhood or adolescence. Venous malformations may be detected anywhere along the GI tract but are most frequently found in the small bowel.11,12 Thrombosis and secondary calcification may occur within the lesions and may explain the hepatic calcifications identified in this patient.13
Anemia in BRBNS is usually occult and chronic, although acute bleeding can present as melena or hematemesis.5 The cause of this patient’s anemia was most likely bleeding from the stomach lesions. No acute bleeding was noted during endoscopy, and capsular endoscopy performed after discharge showed no other lesions in the small bowel. Other cases of patients with BRBNS who presented with anemia and no evidence of active bleeding on endoscopy, similar to this patient, have been reported.14
MANAGEMENT
In patients with mild bleeding or diffuse lesions, treatment usually consists of iron supplementation and blood transfusions, if needed. Refractory GI lesions may be treated with sclerosing therapy or band ligation, although perforation is a risk.12 For lesions in the small bowel, surgical resection of the involved segment is typically considered.12,15 Treatment with oral corticosteroids and subcutaneous interferon-a has been used; however, any effectiveness is lost once the agents are discontinued.5,16
Close follow-up of patients with BRBNS is essential because blood transfusions may need to be repeated. This may consist of periodic fecal occult blood testing and screening for iron deficiency anemia. GI angiomas frequently recur and may warrant further endoscopic monitoring.3 Although radiographic studies with contrast may potentially identify GI lesions, upper endoscopy is more sensitive; colonoscopy is more helpful than barium enema.11 Wireless capsule endoscopy, similar to what was performed in this patient, may be particularly beneficial in identifying lesions in areas of the small bowel inaccessible by peroral push enteroscopy. Children with BRBNS who have abdominal pain should be evaluated for polypoid lesions, which may act as lead points for intussusception.12,14
OUTCOME OF THIS CASE
Surgical and pathology reports from the previous resections of the masses in the child’s hip, thigh, and forearm were all consistent with hemangiomas. At discharge, her hemoglobin level was 10.5 g/dL. The mother was counseled on the importance of continued follow-up to head-off future anemic episodes and the need to discontinue the child’s excessive milk intake. She was also advised of the potential for the child to have neurological sequelae related to the CNS lesions.■


