Photoclinic
Foresee Your Next Patient
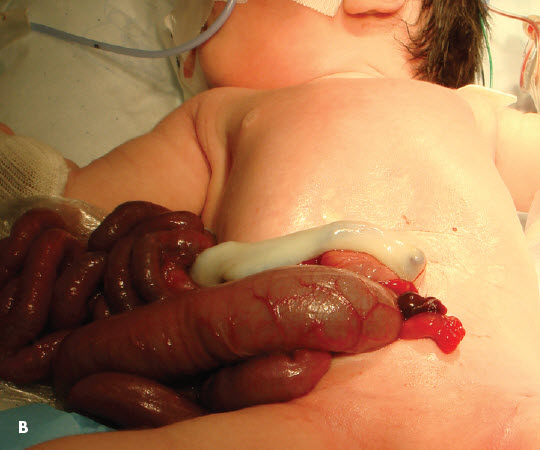
 This baby girl was born at 37 weeks' gestation via cesarean section, with the stomach, small bowel, proximal colon, and ovary outside the body (A). The mother, a 22-year-old gravid 1, para 0, had adequate prenatal care. The anomaly had been detected at 17 weeks' gestation. All maternal serological results were negative, as were cultures for Neisseria gonorrhoeae and Chlamydia. The baby weighed 2950 g. Apgar scores were 8 and 9 at 1 and 5 minutes, respectively.
This baby girl was born at 37 weeks' gestation via cesarean section, with the stomach, small bowel, proximal colon, and ovary outside the body (A). The mother, a 22-year-old gravid 1, para 0, had adequate prenatal care. The anomaly had been detected at 17 weeks' gestation. All maternal serological results were negative, as were cultures for Neisseria gonorrhoeae and Chlamydia. The baby weighed 2950 g. Apgar scores were 8 and 9 at 1 and 5 minutes, respectively.
Gastroschisis is a rare congenital defect in the abdominal wall that results in herniation of abdominal contents; the estimated incidence is 1 in 10,000 live births.1 Unlike omphaloceles, gastroschisis typically occurs in the right paraumbilical area, as in this infant (B), and does not contain a peritoneal sac covering.
The cause is thought to be a vascular accident involving the right umbilical vein or right omphalomesenteric artery (OMA).2 The right umbilical vein normally involutes between 28 and 32 days postconception, whereas the right OMA develops into the superior mesenteric artery. Premature involution of the right umbilical vein or disruption of the distal right OMA can lead to ischemia, infarction, and necrosis of the abdominal wall in the paraumbilical region on the right side. This necrotic section allows bowel to enter the amniotic cavity.3
 Gastroschisis is associated with young maternal age (younger than 20 years). An association with vasoactive substances, such as nicotine, cocaine, and pseudoephedrine, has been suggested but has not been consistently demonstrated.4 (The mother of this baby reported a 1-pack-year smoking history but claimed to have ceased tobacco use throughout her pregnancy.) Associated complications include malrotation, stenosis, and atresia of the GI tract.5 The incidence of cryptorchidism is reportedly higher in infants with gastroschisis.
Gastroschisis is associated with young maternal age (younger than 20 years). An association with vasoactive substances, such as nicotine, cocaine, and pseudoephedrine, has been suggested but has not been consistently demonstrated.4 (The mother of this baby reported a 1-pack-year smoking history but claimed to have ceased tobacco use throughout her pregnancy.) Associated complications include malrotation, stenosis, and atresia of the GI tract.5 The incidence of cryptorchidism is reportedly higher in infants with gastroschisis.
Diagnosis is primarily made prenatally, usually in the second trimester, via ultrasonographic findings showing an intestinal mass to the right of midline that lacks a peritoneal sac. The eviscerated bowel is cauliflower-like in appearance, with amniotic fluid found between each free-floating loop of bowel.6 An elevated maternal serum a-fetoprotein level may also suggest the diagnosis.7
 It is important to wrap the herniated abdominal contents with sterile saline dressings and plastic wrap to help prevent fluid loss and preserve heat and to initiate broad-spectrum antibiotic therapy. The large bowel is evacuated via saline enema, and the upper bowel is decompressed by aspirating stomach contents. The original defect is expanded 1 to 2 cm and the abdominal wall is manually stretched to minimize trauma to the bowel during reduction. In the event that primary closure is unsuccessful, staged closure using a silo may be attempted.8 Total parenteral nutrition is often necessary postoperatively because of prolonged dysmotility of the GI tract.
It is important to wrap the herniated abdominal contents with sterile saline dressings and plastic wrap to help prevent fluid loss and preserve heat and to initiate broad-spectrum antibiotic therapy. The large bowel is evacuated via saline enema, and the upper bowel is decompressed by aspirating stomach contents. The original defect is expanded 1 to 2 cm and the abdominal wall is manually stretched to minimize trauma to the bowel during reduction. In the event that primary closure is unsuccessful, staged closure using a silo may be attempted.8 Total parenteral nutrition is often necessary postoperatively because of prolonged dysmotility of the GI tract.
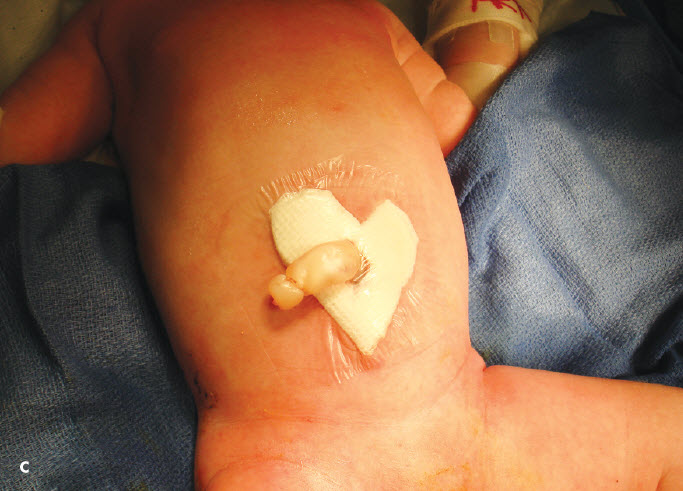
This infant was rushed to the neonatal ICU, where antibiotic therapy with intravenous ampicillin and gentamicin was started. The abdominal contents were successfully reduced during primary closure 5 hours after delivery. Total parenteral nutrition was advanced via a central saphenous line. Photo C shows the abdomen on day 3 of life. On this day, she was extubated and was doing well.■


