Fatal Septicemia due to Vibrio vulnificus following Hurricane Fay
History
A 64-year-old white male was admitted to the hospital with right leg swelling, severe pain, fevers, and chills. One week prior to admission, the patient scraped his right leg against a metal object while working as a bartender at an intracoastal restaurant where he had to frequently wade through water—at higher levels due to tropical storm Fay. His other pertinent medical history included chronic alcohol abuse, hepatitis C, diabetes mellitus, and hypertension.

Figure 1. Extensive cellulitis of the right lower limb.
Physical Examination
Vital signs at admission included blood pressure at 84/51 mm Hg, a heart rate of 120 beats per minute, a respiration rate of 30 breaths per minute, and a temperature of 102.5º F. Examination revealed an encephalopathic male with extensive cellulitis of his right lower extremity and early blistering of the skin (Figure 1). There was tenderness to palpation but no crepitus. Two superficial scratches were present on the lateral side of the leg. Pulses were palpable in the lower extremities, bilaterally. There were multiple circular skin lesions on his trunk, some with early central blistering (Figures 2 and 3).

Figure 2. Circular lesions present over the trunk with early blistering.
Initial laboratory data is shown in the Table. A CT scan of the leg showed edema in the superficial soft tissue without focal fluid collections.
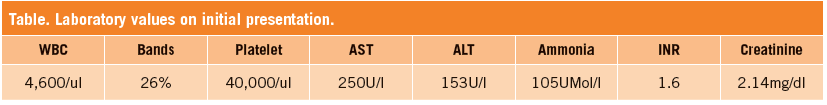
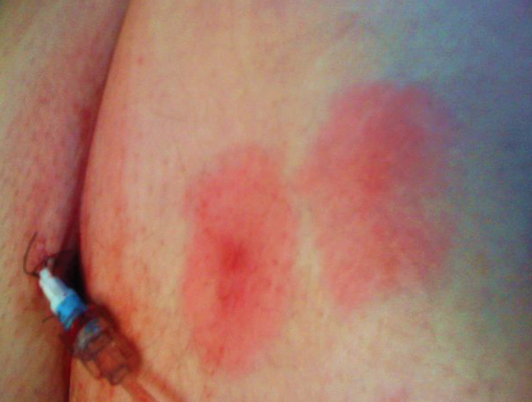
Figure 3. Circular lesions present on the trunk at initial presentation to the hospital.

Figure 4. Increase in the size and number of lesions on the trunk over subsequent 36 hours.
Blood and wound cultures were obtained. Empiric vancomycin, clindamycin, and cefipime were administered. He clinically deteriorated, was intubated, and started on vasopressors. Wound and blood cultures grew gram negative bacilli. Ciprofloxacin was added to the regimen.
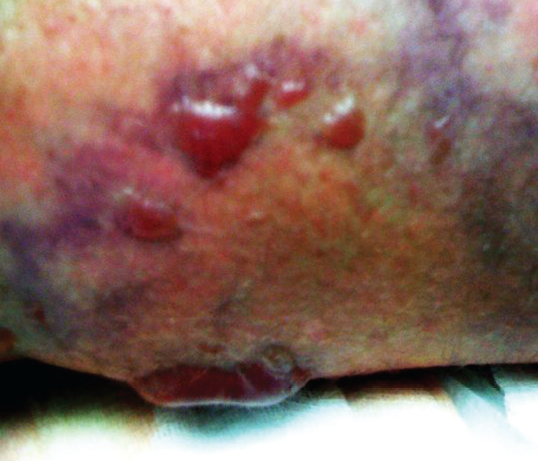
Figure 5. Progression of the lesions to hemorrhagic bullae.
Over the subsequent 12 hours, he developed expanding lesions over his body with bulla and central necrosis (Figures 4 and 5).
What's Your Diagnosis?
(Answer and discussion on next page)
Answer: Vibrio vulnificus
Surgical debridement of the leg was deferred due to hemodynamic instability. The APACHE II score was 39 and Xigris was added. Blood and wound cultures ultimately grew Vibrio vulnificus, sensitive to all antibiotics tested. Doxycycline was added to the regimen and cefipime was changed to ceftriaxone.
Despite antibiotics and aggressive care, the patient developed overwhelming disseminated intravascular coagulopathy and died within 36 hours of admission to the hospital.
Discussion
Vibrio vulnificus is a halophilic, gram negative marine bacteria commonly isolated from shellfish that causes gastroenteritis, wound infections, and septicemia.1 In healthy individuals, nausea, vomiting, and diarrhea occur 15-20 hours after ingesting undercooked shellfish, often resolving without long-term consequences.2 However, patients with chronic liver disease, alcoholism, and diabetes are at risk to develop primary septicemia—usually acquired through ingestion of raw oysters or exposure of wounds to sea water.3
Vibrio vulnificus inhabits marine waters worldwide, thrives at warmer temperatures, and prefers salinities of 15-25 parts per thousand salt.4 The organism is not associated with pollution or fecal waste, and is readily killed by cooking.5 Vibrio vulnificus is sensitive to most antibiotics, including third generation cephalosporins, quinolones, tetracyclines, and aminoglycosides; some evidence suggests there is synergy between third generation cephalosporins and tetracyclines.6
The organism’s major virulence factor appears to be utilization of iron to accelerate bacterial growth; inoculating Vibrio vulnificus in iron-overloaded mice resulted in increased proliferation and enhanced cytotoxicity.7 Liver diseases associated with deranged iron metabolism, such as hemochromotosis and cirrhosis, are highly associated with fatal outcome.8
Vibrio vulnificus infections are more common in males. Females appear to have protection from the bacterial endotoxin by the hormone estrogen.9 Patients presenting in shock and with hemorrhagic bullous lesions have a mortality of up to 50 %.10
We speculate that exposure to tropical storm waters may have increased this patient’s risk for infection, which will correlate with data from the Centers for Disease Control and Prevention reported an increase in the incidence of Vibrio vulnificus infections after Hurricane Katrina.11 The increased incidence of Vibrio vulnificus infections after tropical storms should alert physicians in coastal areas to have a high index of suspicion among patients with risk factors for developing primary septicemia, including liver disease, diabetes, and immune suppression. Early antibiotic treatment and surgical debridement may improve the outcome in these patients.12 ■
References
1. Hlady WG, Klontz KC. The epidemiology of Vibrio infections in Florida, 1981-1993. J Infect Dis. 1996;173(5):1176-1183
2. Schwartz RA, Jagar C. Prognostic factors for primary septicemia and wound infection caused by Vibrio vulnificus. Am J Emerg Med. 2010; 28(4):424-431.
3. Morris JG. Cholera and other types of vibriosis: a story of human pandemics and oysters on the half shell. Clin Infect Dis. 2003;37(2):272-280.
4. Strom MS, Paranjpye RN. Epidemiology and pathogenesis of Vibrio vulnificus. Microbes and Infection. 2000;2(2):177-188.
5. Bross HM, Soch K, Morales R, et al. Vibrio Vulnificus infection: diagnosis and treatment. American Family Physician. 2007;76(4):539-544.
6. Chiang SR, Chuang YC. Vibrio vulnificus infection: clinical manifestations, pathogenesis, and antimicrobial therapy. J Microbial Immunol Infect. 2003;36:81-88
7. Hor LI, Chang YK, Chang CC, et al. Mechanism of high susceptibility of iron-overloaded mouse to Vibrio vulnificus. Microbiol Immunol. 2000; 44(11):871-878.
8. Shapiro RL, Altekruse S, Hutwagner L, et al. The role of Gulf Coast oysters harvested in warmer months in Vibrio vulnificus infections in the United States, 1988-1996. J Infect Dis. 1998;178:752-759.
9. Oliver JD. Wound infections caused by Vibrio Vulnificus and other marine bacteria. Epidemiol Infect. 2005;133:383-391.
10. Liu JW, Lee IK, Tang HJ, et al. Prognostic factors and antibiotics in Vibrio Vulnificus septicemia. Arch Intern Med. 2006;166(19):2117-2123.
11. Bopp C, Mintz E, Sobel J et al. Vibrio illnesses after Hurricane Katrina—Multiple States, August-September 2005. MMWR. 2005;54(37):928-931.
12. Halow KD, Harner RC, Fontenelle LJ. Primary skin infections secondary to Vibrio vulnificus: the role of operative intervention. J Am Coll Surg. 1996;183:329-334.
Anju Bhagavan, MD, is a hospitalist at Baystate Medical Center/TUFTS University School of Medicine in Springfield, MA.
Latha Srinath, MD, is an infectious disease consultant at Bethesda Memorial Hospital in Boynton Beach, FL.
Sarah Haessler, MD, is an infectious disease specialist and assistant professor of medicine at Baystate Medical Center/TUFTS University School of Medicine in Springfield, MA.


