Eye Infection: Cures for a Common Ailment, Part 1
ABSTRACT: For uncomplicated infections of the eyelid, treatment typically consists of warm compresses. Topical 1% azithromycin ophthalmic drops for 4 weeks have been shown to improve meibomian gland secretion and reduce conjunctival redness and other symptoms in patients with blepharitis. In patients with hordeola, topical antibiotics may help prevent the spread of infection. Dacryoadenitis is generally treated with an oral antibiotic, such as dicloxacillin or clindamycin, whereas dacryocystitis often requires parenteral antibiotics with nafcillin or clindamycin. Primary treatment of viral conjunctivitis is patient education; medical management includes artificial tears, cold compresses, and topical vasoconstrictors (eg, naphzoline). Topical 1% trifluorothymidine or trifluridine solution, 1 drop every 2 hours, or vidarabine ointment may be used in primary cases of ocular herpes simplex virus infection. Therapy for bacterial conjunctivitis should be aggressive and antibiotics should be instilled in the eyes at least every 6 hours over the first few days. Initial broad-spectrum antibiotics include combination polymixin B sulfate and trimethoprim sulfate, 0.3% gentamicin, 0.5% erythromycin, and 0.3% tobramycin drops or ointments. Alternatives include fluoroquinolones, such as ciprofloxacin, ofloxacin, and moxifloxacin.
_____________________________________________________________________________________________________________________________________________________________________
Children frequently present to their primary care providers with eye complaints, such as redness, itchiness, drainage, and crusting. Examination of the eye in a child can be challenging and requires knowledge and expertise. The clinician must be able to perform an eye examination efficiently and thoroughly and consider the various pathological processes, which may involve the eyelid, conjunctiva, cornea, lens, or structures behind the eye.
This article is the first in a 2-part series on eye infections that are commonly managed by the pediatric primary care practitioner. Here, we discuss infections of the eyelid, lacrimal system, and conjunctiva. In an upcoming article, we will review infections of the cornea, sclera, uveal tract, and orbit.
INFECTIONS OF THE EYELID
Blepharitis is an inflammation of the eyelid that may be associated with conjunctivitis and keratitis. There are 2 types of blepharitis: anterior and posterior. Anterior blepharitis affects the region at the base of the eyelashes, is usually caused by infection (Staphylococcus) and dandruff, and is characterized by scaling and crusting along the eyelashes. Chronic inflammation may be interspersed with acute exacerbations leading to ulcerative blepharitis with loss of eyelashes and involvement of the cornea. A combination of direct infection with staphylococci, reaction to the exotoxin and allergic reaction to the staphylococcal antigen is probably responsible for the clinical manifestations.
Posterior blepharitis involves the inner (moist) surface of the lid and is caused by dysfunction of the meibomian gland that is often associated with skin conditions, such as acne rosacea. Redness and crusting of eyelid margins (particularly in the mornings), tearing, photophobia, itching, swollen eyelids, and redness of the conjunctiva may occur. Complications include hordeolum, chalazion, and dry eyes.
Treatment. Both forms of blepharitis are treated by keeping the lids clean and free of crusts. Warm compresses followed by light scrubbing of the eyelid with a cotton swab dipped in a mixture of baby shampoo and water may be effective. However, this regimen may need to be followed for a prolonged period because blepharitis rarely resolves completely.
Use of topical antibiotics can play a role in the treatment of blepharitis because of the propensity for bacterial overgrowth and increased lipase activity of the bacteria. Topical 1% azithromycin ophthalmic drops for 4 weeks have been shown to improve meibomian gland secretion and reduce conjunctival redness and other symptoms.1,2
For patients with staphylococcal blepharitis, a topical antibiotic, such as bacitracin or erythromycin, can be applied to the eyelids 1 to 3 times daily for 1 or more weeks, with the frequency and duration of therapy being guided by severity of disease.
For patients with meibomian gland dysfunction, oral erythromycin (for young children) or doxycycline (for older children) may be used. In severe cases of inflammation, a brief course of topical corticosteroids may be effective.3 Use of cyclosporine 0.05% eye drops has led to reduced symptoms in some cases of posterior blepharitis but is very expensive and should be reserved for cases that have failed traditional treatment. Other medications that are being evaluated include topical metronidazole in cases associated with rosacea and topical tacrolimus in severe cases.
Many patients with blepharitis have aqueous tear deficiency. Application of artificial tears 2 to 4 times daily, when used as an adjunct to medications and lid hygiene, may ameliorate symptoms. Any underlying skin conditions should be treated. Severe blepharitis may need referral to an ophthalmologist.

Hordeolum is an acute infection of the Zeis or Moll sebaceous glands (external hordeolum or stye, Figure 1) or meibomian gland (internal hordeolum). Staphylococcus aureus or Staphylococcus epidermidis are the usual offending organisms. Spread to the neighboring tissues may lead to preseptal cellulitis, and a persistent hordeolum may lead to chronic inflammation resulting in a chalazion.
Treatment. Application of warm compresses 4 times daily is advised. In hordeolum externum, the infection often centers on the base of the eyelash follicle and plucking of the eyelashes often promotes healing. Although topical antibiotics do not help with resolution of hordeola, they may help prevent the spread of infection to other structures. In severe nonresolving cases, surgical drainage may be needed.
Chalazion is a focal inflammatory lesion of the eyelids caused by obstruction of the meibomian gland (usually a result of an internal hordeolum). The meibomian glands are oil-producing glands located in the tarsal plates of both upper and lower eyelids. Due to blockage of the orifice of the gland on the eyelid margin, the sebum of the gland is released into the tarsus and surrounding soft tissues. This results in an inflammatory response with erythema of the skin (Figure 2). Histologically, these lesions are characterized by chronic lipogranulomatous inflammation. Unlike hordeola, chalazia are the result of gland obstruction and sterile inflammation as opposed to bacterial infection. Pain is either mild or often absent.

Although S aureus has been implicated in these lesions, the exact role of bacterial agents is unclear. Seborrhea, acne, and blepharitis are predisposing factors to the formation of a chalazion. Continued inflammation may lead to disfiguration of the eyelids, pyogenic granuloma, and preseptal cellulitis. Large, centrally located chalazia may result in astigmatism and visual disturbances. Diagnosis is clinical and more than half of the cases require only conservative management.
Treatment. Warm compresses 4 times daily and topical antibiotic-steroid ointment may be advised. Intralesional injection of corticosteroids may help in accelerating healing but carries the risk of hypopigmentation of the overlying skin. Large persistent chalazia require surgical drainage and curettage.
In a study that evaluated the efficacy of intralesional triamcinolone acetonide injection, incision and curettage, and a combination of the 2 treatments in children, Mustafa and colleagues4 concluded that all 3 modalities are safe and effective. Intralesional triamcinolone injection is a good procedure for children with chalazia, for those with allergy to local anesthetics, and for children with a chalazion in proximity to the lacrimal drainage system. The authors recommend incision and curettage for infected lesions and the combined treatment for large, recurrent, and multiple chalazia.4
INFECTIONS OF LACRIMAL SYSTEM
Dacryoadenitis is an infection of the lacrimal gland that presents with sudden redness and swelling of the outer end of the upper eyelid. It may be caused by viruses (mumps virus, Epstein-Barr virus, cytomegalovirus, echovirus, varicella zoster virus) or bacteria (S aureus, Streptococcus pyogenes, Chlamydia trachomatis, and Neisseria gonorrhea). Dacryoadenitis is generally treated with an oral antibiotic, such as dicloxacillin or clindamycin, and occasionally intravenous therapy with nafcillin may be required.
Dacryocystitis is a bacterial infection of the lacrimal sac that usually results from the stasis following obstruction of the nasolacrimal duct (the duct that connects the lacrimal sac to the nasal cavity). This is generally preceded by a viral upper respiratory tract infection followed by fever, erythema, swelling, and tenderness in the area below and lateral to the medial canthus (Figure 3). Pus can be exuded from the sac when pressure is applied to the region. Streptococcus pnemoniae is common in neonates, whereas S aureus and S epidermidis are more common in older children. Most patients are toxic-appearing and require parenteral antibiotics with nafcillin or clindamycin.

INFECTIONS OF THE CONJUCTIVA
Inflammation of the conjunctivae lining the eyelids (palpebral) and covering the exposed surface of the sclera (bulbar) is common and may result from infections, irritants, chemicals, and allergens. Only the infectious pathology will be discussed in the underlying sections.
VIRAL CONJUNCTIVITIS
Viral infection is the most common cause of conjunctivitis. Most viral infections produce a mild, self-limited conjunctivitis but some have the potential to cause severe disability. The 2 most common self-limited forms of viral conjunctivitis are epidemic keratoconjunctivitis and pharyngoconjunctival fever.
Epidemic keratoconjunctivitis (EKC) is usually bilateral and pre-sents as inferior, palpebral follicular conjunctivitis. In one-third of patients, corneal inflammation (keratitis) with subepithelial stromal infiltrates develops 7 to 10 days after onset of conjunctivitis. The keratitis is a hypersensitivity reaction to the virus and not a true viral infection. EKC is usually caused by adenovirus 8, 19, or 37.
Pharyngoconjuctival fever (PCF) is characterized by fever, sore throat, and follicular conjunctivitis. Although usually caused by adenovirus 3, it may occasionally be caused by adenovirus 4 or 7. It may be unilateral or bilateral and corneal infiltrates are rare. A few days after the onset, the cornea may show punctuate keratitis that begins as small epithelial dots, which stain with fluorescein. The severity varies and the infection may persist from few days to 2 weeks.
Both EKC and PCF present with redness, tearing, serous discharge, edema of eyelids, pin point subconjunctival hemorrhages, severe photophobia due to corneal infiltrates, pseudomembrane formation and palpable preauricular lymph nodes. In severe cases, scarring and symblepharon may develop. Both conditions are extremely contagious and usually start in one eye and then spread to the other eye within a few days.
Treatment. Primary treatment of viral-associated conjunctivitis is patient education. Children and adolescents should be kept from school or work until there is no discharge and should be advised to avoid sharing of items such as utensils and clothes. Medical management includes artificial tears, cold compresses, topical vasoconstrictors (eg, naphzoline), and corticosteroid drops (only in severe cases with corneal involvement). Caution must be exercised when using corticosteroid drops because they may worsen any bacterial corneal ulcers or herpetic disease.
When a membrane is present, it can be removed using wet cotton-tipped forceps. After removal, a topical antibiotic ointment may be placed in the eye. Antiviral drops are generally ineffective, although cidofovir, an antiviral drug generally used for cytomegalovirus retinitis, has been shown to be efficacious in adenoviral keratoconjunctivitis. Twice daily application is recommended.
Herpes infection. Usually caused by herpes simplex virus 1 (HSV-1), herpetic keratoconjunctivitis (Figure 4) may be associated with encephalitis and other systemic diseases, although it may occur as an isolated lesion. In neonates, it is usually caused by HSV-2, with onset 1 to 2 weeks after birth and serous discharge with moderate conjunctival injection occurring mostly only in one eye.
Ocular infection with HSV carries a significant risk of vision loss, and lesions may include blepharitis, conjunctivitis, keratitis, retinitis, and rarely scleritis. Primary HSV infection presents with conjunctivitis and enlarged preauricular nodes.
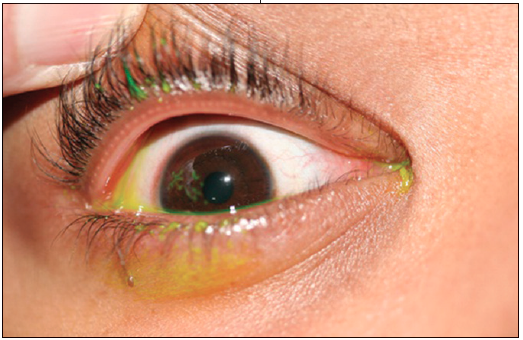
HSV keratitis may be classified into 4 categories: epithelial, stromal, endotheliiltis, and neurotropic keratopathy. While epithelial keratitis is more likely to occur with the first episode, stromal keratitis occurs more often in recurrent cases. Breakdown of the normal epithelial barrier may result in a corneal ulcer. Epithelial keratitis may be detected by a dendritic pattern in the cornea when fluorescein stain is applied to the eye (Figure 5). Diagnosis is confirmed by viral culture.
Recurrent ocular HSV infection. After the initial cutaneous facial infection or mucus membrane infection, the virus gains access to the sensory nerve endings and travels up the axons to the sensory ganglion. It remains sequestered in the ganglion and recurrent ocular HSV infections occur when the virus reactivates and travels down the sensory nerve and infects the cornea or eyelids.
Clinical manifestations are similar to the primary HSV infection and consist of vesicles on eyelids and conjunctivitis but may be more severe. Recurrence may present as symptomatic dendritic, disciform, and necrotizing forms of keratitis. In the dendritic form, branching lesions of the cornea result in corneal ulceration and scarring. Disciform keratitis involves the cornea and is caused by the immune response to the virus. The cornea becomes anesthetized as a result of sensory nerve damage, and corneal scarring can occur.
Recurrent ocular HSV infection is always unilateral. Prompt recognition and treatment prevents blindness. Recurrent, unilateral eye redness should raise the suspicion for herpes infection.
Treatment. Topical 1% trifluorothymidine or trifluridine (Viroptic) solution in the dose of 1 drop every 2 hours or vidarabine ointment may be used in primary cases of ocular HSV infection. Topical ganciclovir 0.15% gel has been shown to be effective in some studies for treatment of HSV keratitis. In a retrospective case series, Schwartz and colleagues5 showed that oral acyclovir as an adjunctive to topical therapy may help in resolution of the infection in children.5 Recurrent cases should also be treated with topical trifluridine solution. Prophylactic oral acyclovir may reduce recurrence.6
Hemorrhagic conjunctivitis. Common causes of hemorrhagic conjunctivitis are picornaviruses, such as enterovirus and coxsackievirus; however, it can also be caused by adenoviruses type 11. Acute hemorrhagic conjunctivitis is highly contagious and usually occurs in epidemics. There is sudden development of hyperemic conjunctiva, subconjunctival hemorrhages, chemosis, lid swelling, tearing, photophobia, and pain. Symptoms last for 3 to 5 days and gradually resolve.
Neurological complications occur rarely with certain adenoviruses and range from mild palsies to permanent flaccid paralysis. These neurological symptoms occur 2 to 3 weeks after the onset of conjunctivitis. Treatment is mainly supportive with artificial tears, cold compresses, and topical decongestants.
BACTERIAL CONJUNCTIVITIS
Normal conjunctiva may harbor common skin bacteria. In addition, any viral conjunctivitis may be complicated by bacterial superinfection. In a study of children who presented to a pediatric emergency department with a red or pink eye and/or had a diagnosis of conjunctivitis, Patel and colleagues7 noted that conjunctival culture was positive for bacteria in 78%.

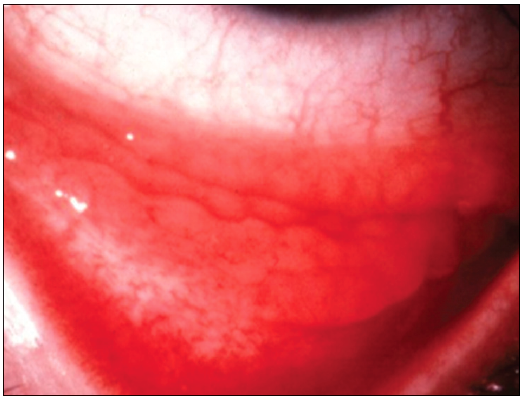
Patients with bacterial conjunctivitis present with injected bulbar conjunctiva, episcleral vessels, and papillae in the palpebral conjunctiva (Figure 6). Thick mucopurulent discharge, which causes eyelash matting and eyelid closure on waking up in the mornings, is usually present. A history of gluey or sticky eyelids and physical findings of mucoid or mucopurulent discharge is highly predictive of bacterial etiology.7
Although mild discomfort and photophobia may exist, pain is usually absent and vision is preserved. Preauricular lymphadenopathy is also less frequent. The most commonly implicated organisms are S aureus, Haemophilus influenzae, Streptococcus pneumonia, and Pseudomonas aeroginosa. In the Patel study, 82% of the conjunctivitis was secondary to nontypeable H influenzae.7 Occasional outbreaks of conjunctivitis due to Haemophilus aegypticus have occurred.
Treatment. Although bacterial conjunctivitis is usually self-limited, treatment probably helps shorten the duration of the infection and helps prevent person-to-person spread. Although cultures can guide management, they are expensive and often impractical and should be reserved for cases in which treatment has failed.
Excellent initial broad-spectrum antibiotics include combination polymixin B sulfate and trimeth-oprim sulfate, 0.3% gentamicin, 0.5% erythromycin, and 0.3% tobramycin drops or ointments. These agents are effective against both gram-negative and gram-positive organisms; aminoglycosides are not that effective against Staphylococcus. Excellent alternatives include fluoroquinolones, such as ciprofloxacin, ofloxacin, and moxifloxacin.
Therapy for the first few days should be aggressive and antibiotics should be instilled in the eyes at least every 6 hours. Ointment may be preferable in children and in those in whom application is difficult. A study by Abelson and colleagues,8 found that therapy with 1% azithromycin drops for 5 days was safe and well-tolerated in children and adults with bacterial conjunctivitis.
Aminoglycosides may be associated with toxicity to the corneal epithelium and may cause a reactive keratoconjunctivitis after several days of use. Fluroquinolones may be particularly indicated in children who wear contact lenses because of the high incidence of pseudomonas infection. Any child who is a contact lens user should be advised to remove and discard the lenses until complete clearing of the eye and absence of discharge. If there is no significant corneal disruption, a corticosteroid may be prescribed along with the antibiotic.
Hyperacute conjunctivitis. The most common cause of hyperacute conjunctivitis is N gonorrhea—a dangerous pathogen with the propensity to penetrate the cornea. Patients with hyperacute conjunctivitis have profuse and purulent discharge within 12 hours of inoculation. The clinical course rapidly progresses with development of redness, irritation, tenderness, marked chemosis, lid swelling, and tender preauricular lymphadenopathy. Keratitis and perforation can occur. Gram stain reveals gram-negative diplococci.
Treatment. Hyperacute conjunctivitis requires hospitalization for parenteral antibiotics and close monitoring.
Parinaud’s oculoglandular syndrome. This unilateral conjunctivitis is associated with a nodule in the tarsal conjunctiva; it results in local swelling and ptosis and is most commonly caused by cat scratch disease. The causative organism is Bartonella henselae. The lid mass is associated with ipsilateral submandibular or preauricular lymph node enlargement. Rarely optic neuritis and macular stellate neuroretinitis may occur.
The patient often has a history of being around a kitten with or without being scratched by it. Positive antibody titers usually support the diagnosis. Other causes of oculoglandular syndrome include tuberculosis, S aureus infection, group A ß hemolytic streptococci infection, and tularemia.
Treatment. Some studies have shown resolution after a 2-week course of treatment with tetracyclines, trimethoprim/sulfamethoxazole, or fluroquinolones. Prognosis is excellent.


