Peer Reviewed
External Jugular Vein Thrombosis in an Adolescent With Lemierre Syndrome
AUTHORS:
Krishnamallika Mutyala, MD; Eric J. McGrath, MD; Maria Caridad Davalos, MD; Bhanumathy Kumar, MD; Michael Callaghan, MD; and Jocelyn Y. Ang, MD
Wayne State University School of Medicine
CITATION:
Mutyala K, McGrath EJ, Davalos MC, Kumar B, Callaghan M, Ang JY. External jugular vein thrombosis in an adolescent with Lemierre syndrome. Consultant for Pediatrics. 2012;11(10):316-320.
A 17-year-old girl presented to the emergency department with bilateral ear pain, worsening dysphagia, and throat pain of about 7 days’ duration. She also had fever.
Physical examination revealed a temperature of 39.5ºC (103.1ºF), blood pressure of 95/49 mm Hg, heart rate of 104 beats per minute, respiration rate of 20 breaths per minute, and oxygen saturation of 97% on room air. She had a muffled, high-pitched voice. Head and neck examination revealed pain and decreased range of motion of the neck with 3+ enlarged right tonsil and normal left tonsil without uvular deviation. The remaining examination findings were normal.
Initial laboratory results showed an elevated white blood cell count of 22,700/µL; a hemoglobin level of 11.7 g/dL, hematocrit of 32.6%; and platelet count of 66,000/µL. Electrolyte and initial liver enzyme levels were normal. The patient received 1 g IV ceftriaxone and was transferred to our center for further management.
Prerenal azotemia was noted (with blood urea nitrogen, 59 mg/dL; creatinine, 1.1 mg/dL). The C-reactive protein level was 266.9 mg/L; albumin was 2.1 g/dL. Coagulation studies were abnormal: D dimer, 1.42 mg/L (normal, less than 0.59 mg/L); fibrinogen, 473 mg/dL (normal, 158 to 474 mg/dL); activated partial thromboplastin time (APTT), 50.4 s (normal, 23.2 to 34.1 s); and prothrombin time (PT), 14.8 s (normal, 9.6 to 11.8 s).
The 1 g IV ceftriaxone was continued every 12 hours and 600 mg IV clindamycin every 6 hours. Lateral neck radiographs showed asymmetric soft tissue swelling more prominent on the right. Carotid Doppler ultrasound examination of the neck revealed normal analysis of the bilateral internal jugular veins (IJVs) and bulky bilateral submandibular glands. A CT scan of the neck with contrast revealed a right parapharyngeal abscess and thrombosis of the right external jugular vein (EJV) (Figure).


Figure. A CT scan of the neck with contrast showed a right parapharyngeal abscess (A, arrow) and thrombosis of the right external jugular vein (B, arrow).
After drainage of the right parapharyngeal abscess, respiratory distress with hypoxia developed. A CT scan of the thorax revealed septic emboli to the lungs. Serial chest radiographs showed bilateral opacities and pleural effusions more prominent on the left side and left lower lobe pneumonia. Ultrasound-guided thoracocentesis was performed and 660 mL of nonclotting, serosanguinous fluid was drained. The patient required transfusion with 2 units of platelets and 1 unit of packed red blood cells during the course.
Parapharyngeal abscess anaerobic culture grew clindamycin-resistant Prevotella species. Aerobic cultures of the abscess grew coagulase-negative Staphylococci and
viridans group Streptococci. All blood, respiratory, and pleural fluid culture results were negative.
The CT evidence of EJV thrombosis prompted consultation with a hematologist, who recommended anticoagulation with intravenous heparin for 4 days followed by transition to subcutaneous injection of low molecular weight heparin (LMWH), 60 mg twice daily.
A comprehensive thrombophilia workup revealed a normal lipid profile but abnormal clotting profile: antithrombin III activity, 146% (normal, 78% to 130%); factor II (prothrombin) activity, 166% (normal, 75% to 133%); factor VIII activity, 350% (normal, 63% to 136%); protein C activity, 146% (normal, 73% to 144%); protein S activity, 105% (normal, 70% to 128%); and von Willebrand antigen, 166% (normal, 43% to 138%). Hexagonal phase lupus anticoagulant and PTT-LA (partial thromboplastin time-lupus anticoagulant) were positive, but antinuclear antibody was not detected. Cardiolipin antibodies IgG and IgM were both positive. Genetic testing revealed that the patient was not a carrier of factor V Leiden or prothrombin 20210G>A.
Because of increasing hepatic enzyme levels, the patient’s antibiotic therapy was switched to ampicillin/sulbactam. She was hospitalized for 19 days and discharged home to continue treatment through a peripherally inserted central catheter for 6 weeks. She received anticoagulation with LMWH for 3 months.
At 3-month follow-up, circulating anticoagulant and lupus anticoagulant were no longer detectable; factor VIII activity was persistently elevated at 230% (from 350%) but normalized after 9 months. Chest radiograph findings at treatment completion were normal, and a second CT scan of the neck with contrast showed resolution of the right parapharyngeal abscess and patent bilateral IJVs. The right EJV appeared smaller in caliber but patent.
LEMIERRE SYNDROME: AN OVERVIEW
Lemierre syndrome, also known as postanginal septicemia or necrobacillosis, classically consists of oropharyngeal infection with bacteremia and suppurative thrombophlebitis of the cervical veins complicated by metastatic septic emboli.1 Andre Lemierre first characterized the disease in 1936 in a series of 20 cases.1,2 The mortality rate at that time was 90%.
The usual etiologic agent, Fusobacterium necrophorum, is a normal inhabitant of the oral cavity, female genital tract, and GI tract.3 Other organisms, including Bacteroides species, Peptostreptococcus species, group B and C streptococci, Streptococcus oralis, Staphylococcus epidermidis, Enterococcus species, Proteus mirabilis, Eikenella corrodens, Lactobacillus species, and Candida species, have been reported to cause a Lemierre-like syndrome, and the infection may be polymicrobial.3-5
Most cases occur in young adults aged 16 to 25 years.4 Classic Lemierre syndrome has 4 findings:
- A primary oropharyngeal infection.
- Bacterial sepsis with at least one positive blood culture.
- Clinical or radiologic demonstration of thrombosis of a vein in the head or neck.
- Infection in at least one distant site.1,4
When pretreatment with antibiotics is given before a blood culture is obtained, as in this case, the blood culture may be negative. Serious thrombotic complications are associated with this syndrome and may involve nearly all body systems, but commonly the IJV.6 EJV thrombosis is a rare complication of Lemierre syndrome.1,7-10
THROMBOSIS IN LEMIERRE SYNDROME
Thrombosis in Lemierre syndrome and Lemierre-like syndromes is likely to be a multifactorial process that may result in chronic complications.6 An underlying prothrombotic tendency may be caused by genetic mutations (ie, factor V Leiden mutation) or by increased lipoprotein or factor VIII activity and antiphospholipid antibody production.1,11 This is consistent with the results in this case, including elevated factor VIII activity and detectable anticardiolipin and lupus anticoagulant antibodies. The D dimer level was only slightly elevated. This is in contrast to other thrombotic disorders in which values much greater than 1.0 mg/L represent elevated thrombolysis
Our patient had elevated PT and APTT commonly found in the early post-thrombotic setting. Increased PT, APTT, and coagulation factor activity may be the result of circulating anticoagulants. The presence of these anticoagulants is almost universal in previous reports of thrombosis in Lemierre syndrome.6 Circulating anticoagulants may behave more like prothrombotic anticoagulants than like transient anticoagulants (seen in other childhood infections) and thus increase the risk
of thrombosis.6
In addition to inherent host factors, another proposed mechanism of thrombosis in patients with Lemierre syndrome is vascular inflammation associated with infection adjacent to the jugular veins. Fusobacterium is known to induce endothelial damage and cause platelet aggregation factor effects,5,7 which may increase thrombosis risk.
Thrombosis of the jugular veins may be secondary thrombophlebitis of the tonsillar veins from underlying pharyngeal infection, causing thrombus propagation to the IJV—and potentially to the EJV—or cause perivenous inflammation.1,4 EJV thrombosis may represent an extension or progression of the inciting infectious process with associated venous stasis and thrombophlebitis occurring in anatomical close proximity to the more commonly involved IJV via connecting venous vasculature.
The findings of 6 pediatric cases of EJV thrombosis in Lemierre syndrome, including our case, are listed in the Table.1,7-10 All 6 cases had similar presenting features, with most having fever, sore throat or pharyngitis, and neck pain. Three of the 6 cases, including our case, had isolated EJV thrombosis; the other 3 cases reported concomitant IJV thrombosis. One EJV thrombosis was noted intraoperatively with tonsillectomy and peritonsillar abscess drainage.10 EJV thrombosis was missed on Doppler ultrasound examination in 2 cases, including ours.


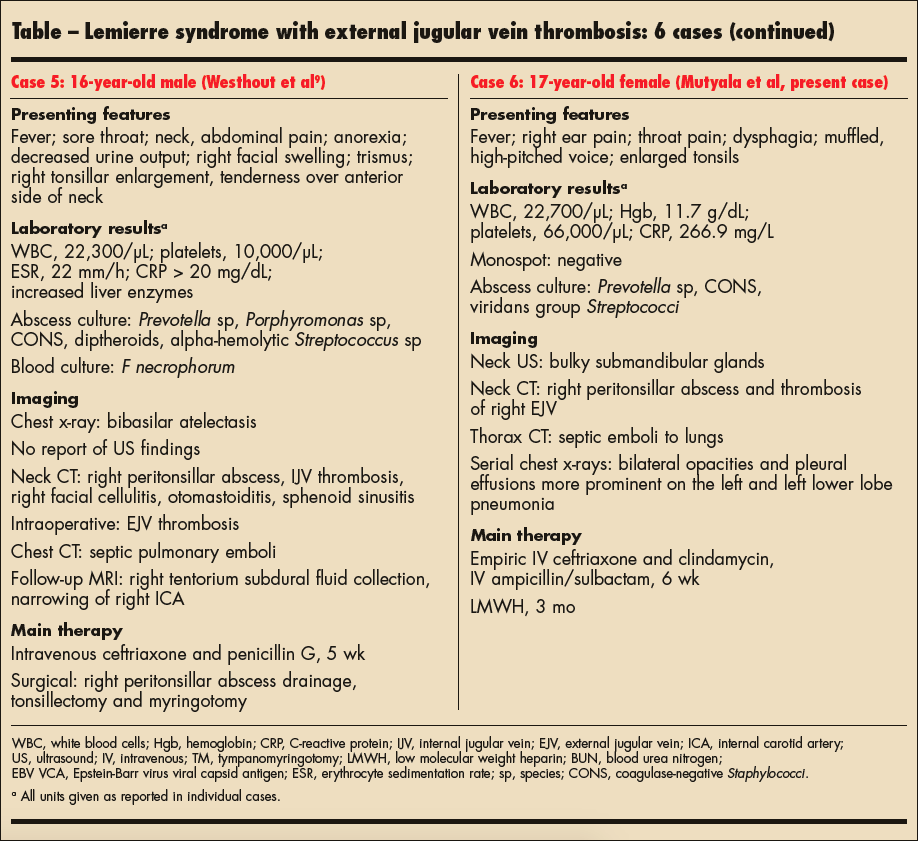
All 6 cases had evidence of septic pulmonary emboli on chest imaging. Four of the 6 patients, including our patient, received anticoagulation therapy, namely with LMWH, with varying degrees of return of patency.1,8,9 All 6 patients were treated with prolonged intravenous antibiotics and had apparent recovery at therapy completion.
MANAGEMENT OF LEMIERRE SYNDROME
Treatment of Lemierre syndrome consists of antimicrobial therapy with surgical drainage of neck abscesses when present.1,7 Because ß-lactamase production has been documented in cases of Lemierre syndrome caused by Fusobacterium species, antimicrobial therapy often includes intravenous ß-lactamase–resistant antibiotics, such as ticarcillin/clavulanate, ampicillin/sulbactam, metronidazole, and clindamycin.1,3,4,7 How-ever,no treatment guideline exists. Prolonged antimicrobial therapy for 3 to 6 weeks may be necessary to eradicate infection due to its endovascular nature.4
Anticoagulation in Lemierre syndrome is controversial.4,6 Anticoagulation may help rapidly dissolve septic emboli and thrombi and may potentially limit the duration of bacteremia and propagation of further embolic events leading to less chronic vascular occlusion.6,7 However, consideration must be given to the risk of bleeding in the setting of thrombocytopenia (such as in our patient), and particularly after septic brain emboli. Although it took 9 months for factor VIII activity to normalize in our patient, the right EJV thrombus resolved after only 3 months of anticoagulation therapy.

REFERENCES:
1. Ridgway JM, Parikh DA, Wright R, et al. Lemierre syndrome: a pediatric case series and review of literature. Am J Otolaryngol. 2010;31(1):38-45.
2. Lemierre A. On certain septicemias due to anaerobic organisms. Lancet. 1936;1:701-703.
3. Rathore MH, Barton LL, Dunkle LM. The spectrum of fusobacterial infections in children. Pediatr Infect Dis J. 1990;9(7):505-508.
4. Chirinos JA, Lichtstein DM, Garcia J, Tamariz LJ. The evolution of Lemierre syndrome: report of 2 cases and review of the literature. Medicine (Baltimore). 2002;81(6):458-465.
5. Hoehn KS, Capouya JD, Daum RS, et al. Lemierrelike syndrome caused by community-associated methicillin-resistant Staphylococcus aureus complicated by hemorrhagic pericarditis. Pediatr Crit Care Med. 2010;11(3):e32-e35.
6. Goldenberg NA, Knapp-Clevenger R, Hays T, Manco-Johnson MJ. Lemierre’s and Lemierre’s-like syndromes in children: survival and thromboembolic outcomes. Pediatrics. 2005;116(4):e543-e548.
7. Ramirez S, Hild TG, Rudolph CN, et al. Increased diagnosis of Lemierre syndrome and other Fusobacterium necrophorum infections at a Children’s Hospital. Pediatrics. 2003;112(5):e380.
8. Morris P, O’Sullivan E, Choo M, et al. A rare cause of sepsis in an 18 year old. Lemierre’s syndrome with external jugular vein thrombosis. Ir Med J. 2006; 99(1):24.
9. Waterman JA, Balbi HJ, Vaysman D, et al. Lemierre syndrome: a case report. Pediatr Emerg Care. 2007;23(2):103-105.
10. Westhout F, Hasso A, Jalili M, et al. Lemierre syndrome complicated by cavernous sinus thrombosis, the development of subdural empyemas, and internal carotid artery narrowing without cerebral infarction. Case report. J Neurosurg. 2007;106 (1 suppl):53-56.
11. Oestreicher-Kedem Y, Raveh E, Kornreich L, et al. Prothrombotic factors in children with otitis media and sinus thrombosis. Laryngoscope. 2004;114(1):90-95


