A Collection of Rashes
Granuloma Annulare
Amor Khachemoune, MD, and Mana Ogholikhan, MD
Several asymptomatic, erythematous papules and plaques had appeared on the hands of an otherwise healthy 11-year-old girl. The personal and family medical histories were noncontributory. A punch biopsy from the largest lesion on the palm confirmed the clinical diagnosis of localized granuloma annulare, a self-limited inflammation of the dermis.
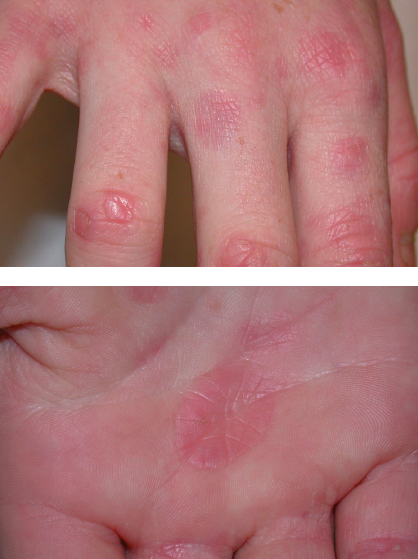
Discussion. Lesions of granuloma annulare usually disappear spontaneously within several months to several years. Although the eruption clears in most patients within 2 years, lesions may persist for more than 8 years in up to 25% of those with the disease. These lesions are self-limited but can recur.1 Most granuloma annulare lesions occur locally; they can also be subcutaneous, perforating, macular, and disseminated.
Perforating granuloma annulare is rare. It presents as skin-colored to erythematous, scaly and crusted, umbilicated papules. Lesions tend to improve in the winter and worsen in the summer. Papules of perforating disease evolve more slowly, are more pustular, and are more likely to scar than the lesions of localized disease.2
The flat, slightly palpable lesions of the macular variant tend to arise on the feet, ankles, and thighs. Individual lesions are typically between 1 cm and 4 cm in diameter but can be much larger. Small papules may be palpated; papules or small annular lesions can be seen when the skin is stretched.
Disseminated disease presents as multiple skin-colored or erythematous papules that can fuse to form annular rings.
The cause of granuloma annulare is unclear; it can occur following viral infections, insect bites, tuberculin skin tests, cell-mediated hypersensitivity reactions, trauma, vitamin D excess, and ultraviolet light exposure. Although the existence of a relationship between granuloma annulare and diabetes is debatable, this skin disease occurs in up to 10% of adults with diabetes.2 Iritis, sarcoidosis, autoimmune thyroiditis, and neoplasms are other associated diseases. Results of a complete blood cell count, blood chemistry panel, rheumatoid factor level,
and erythrocyte sedimentation rate can help confirm the diagnosis of an associated disease.
The natural history of granuloma annulare in persons with HIV infection is unknown. However, the skin disorder has developed in patients in all stages of HIV disease.
Differential diagnosis. The differential diagnosis includes tinea, nummular eczema, the herald patch of pityriasis rosea, urticaria, erythema chronicum migrans (Lyme disease), and erythema multiforme. A skin biopsy can confirm the diagnosis. Histologic features are well-demarcated foci of collagenous degeneration. The focal mucinous degeneration of collagen, or necrobiosis, is surrounded by lymphocytes and fibroblasts, often in a palisading pattern. Giant cells are rarely found.
Diagnostic studies. Reassurance and observation are sufficient therapy. To hasten resolution, both intralesional and topical superpotent corticosteroids may be tried; however, limit their use to avoid secondary atrophy, telangiectases, and pigmentary changes. Cryotherapy, lasers, surgical excision, pentoxifylline, oral vitamin E, antimalarials, alkylating agents, various NSAIDs, and radiation therapy also have been used. Psoralen-UVA therapy, isotretinoin, dapsone, and antituberculosis medications have been used successfully to treat perforating granuloma annulare.3
One case study reported that a lesion rapidly resolved after 2 separate biopsies, whereas the lesions that were not biopsied remained unchanged.4 This report raised speculation that biopsy may induce resolution of granuloma annulare. ■
References:
1. Barron DF, Cootauco MH, Cohen BA. Granuloma annulare. A clinical review. Lippincotts Prim Care Pract. 1997;1:33-39.
2. Odom RB, Arnold HL, James WD, Berger TG. Andrews' Diseases of the Skin: Clinical Dermatology. 9th ed. Philadelphia, PA: WB Saunders Company; 2000.
3. Fang KS, Lawry M, Haas A. Papules on the hands. Granuloma annulare. Arch Dermatol. 2001;137:1647-1652.
4. Levin NA, Patterson JW, Yao LL, Wilson BB. Resolution of patch-type granuloma annulare lesions after biopsy. J Am Acad Dermatol. 2002;46:426-429.
Pruritic Eruption on a Woman’s Arms, Thighs, and Buttocks
David L. Kaplan, MD
This pruritic eruption appeared on the arms, thighs, and buttocks of a 28-year-old woman after the uneventful delivery of her second child.

Discussion. Keratosis pilaris can be exacerbated following pregnancy.1 Pruritus is not a common feature but has been reported.
A staphylococcal infection would be painful, and the distribution on the arms, legs, and buttocks is not typical of a fungal folliculitis. Scabies is a possibility, but one would expect lesions on the trunk, hands, finger webs, and wrists. Follicular eczema is also possible, although this rash usually is preceded by itching; in patients with keratosis pilaris, the papules precede the itching. ■
Reference:
1. Jackson JB, Touma SC, Norton AB. Keratosis pilaris in pregnancy: an unrecognized dermatosis of pregnancy? W V Med J. 2004;100:26-28.
Young Girl with Vesicular Rash
David Effron, MD, and Alex Green, DO
The patient had contracted rhus dermatitis after playing in a bush that was infested with poison ivy. Rhus dermatitismay be caused by poison ivy, poison sumac, or poison oak. The oil on the leaves, roots, and stems contain urushiols, highly allergenic compounds that cause a type IV hypersensitivity reaction. Allergic persons are sensitized to the compound before reacting to the oil. Our patient had a previous case of poison ivy. Because this is a delayed hypersensitivity reaction, the vesicles appear 8 to 72 hours after contact.

Physical examination. Vesicle location depends on the site of exposure and whether the oil was transmitted along the skin by a vector, including scratching. Scratching creates a linear pattern. Lesions persist for 10 to 21 days. Vesicle fluid does not contain urushiol and does not cause further spread of the rash if the vesicle is ruptured. Clothing, tools, and other objects that are exposed to the oil must be washed because of the continued possibility of transmission.
Because the patient had no secondary infection, her treatment was symptomatic. Management included daily colloidal oatmeal baths, topical over-the-counter lotions, and cold, wet compresses followed by topical hydrocortisone 2.5% to relieve pruritus and swelling. The tongue vesicles were treated with topical anesthetics. In more severe cases, oral corticosteroids are taken daily and tapered over a 3-week period.
Discussion. Dyshidrotic eczema (pompholyx) is a chronic relapsing and recurring eruption of vesicles on the palms, lateral fingers, and soles. The rash is highly pruritic and features symmetric vesicles that range from 0.1 cm to 0.5 cm. Although several causes have been proposed, the pathophysiology of dyshidrotic eczema is not yet understood. Sweat gland dysfunction was originally thought to be the principal cause, but this has been disputed.
Dyshidrotic eczema may be triggered by exogenous factors (eg, infection or contact dermatitis), emotional stress, or environmental factors (eg, seasonal changes or humidity). Many patients have associated atopic dermatitis. The vesicles generally resolve in about 3 weeks. Treatment includes high-potency topical corticosteroids, oral corticosteroids, and antihistamines.
In patients with varicella, lesions at different stages—vesicles, pustules, and crusts—are present simultaneously. The 0.2 cm to 0.4 cm vesicles are described as “dew on a rose petal” because of the clear fluid and erythematous base. The disease is contagious as long as the vesicles are not all in the crust stage. Vesicles can form all over the body, including the oral cavity and vagina. Although our patient was vaccinated against varicella, the seroconversion rate after 1 dose is 95%. This leaves open the possibility of a less severe form called “breakthrough varicella.” Treatment of varicella consists of antihistamines and mild antipruritic lotions.
Impetigo, which is most commonly caused by Staphylococcus aureus, has 2 clinical presentations—bullous and nonbullous. It typically appears on the face but can also involve the scalp, arms, and legs. Nonbullous impetigo usually has a honey-yellow crust that forms after the vesicles or pustules rupture. The erythematous base does not typically extend beyond the lesions.
Treatment. The treatment for localized infections consists of topical antibiotic agents, such as mupirocin 2%. An oral antibiotic, such as cephalexin or dicloxacillin, is recommended for systemic disease. ■
Nummular Eczema
David Kaplan, MD
A 26-year-old woman presents with a pruritic rash on her trunk that erupted when she started swimming over the summer. She has seasonal allergies that are well-controlled with an oral nonsedating antihistamine. She owns a cat and works indoors. Her only other medication is an oral contraceptive.
Outcome of the case. This patient had a flare of atopic dermatitis caused by excessive time in the water, which removed the protective oils from her skin. As a result, nummular eczema developed. Application of moisturizer before and after swimming and use of a mid-potent corticosteroid cream helped resolve the rash.

Discussion. It would be unusual for tinea corporis to be as extensive as the eruption seen here. Pityriasis is a reasonable consideration, although the presence of a herald patch, a “fir tree” distribution, a preceding viral illness, and confinement to the trunk and proximal extremities would better support this diagnosis. Urticaria typically comes and goes and is not scaly or crusty. The distribution of this patient’s rash is slightly patchy for a contact dermatitis, and she does not have a strong history of contactant exposure. ■
Norwegian Scabies
Ted Rosen, MD
A 52-year-old white man presented with a pruritic eruption on the neck of 3 months’ duration. The rash had not responded to a potent topical corticosteroid prescribed by another practitioner for the presumed diagnosis of eczema.
The patient reported no current health problems. His history included a pubic louse infestation and several episodes of uncomplicated urethral gonorrhea. He readily admitted to having unprotected sexual intercourse with prostitutes.

A heavily crusted, fissured plaque encircled the patient’s neck and extended to the upper chest and ears. The differential diagnosis included chronic contact dermatitis; Hailey-Hailey disease; severe atopic eczema; and crusted, or Norwegian, scabies. Innumerable scabies mites were revealed by microscopic examination of a skin scraping placed in mineral oil; Norwegian scabies was diagnosed.
Discussion. Norwegian scabies is a severe, although rare, form of scabies caused by the mite Sarcoptes scabiei. Crusting dermatitis of the hands and feet and erythematous scaling plaques on the neck, head, and back are characteristic. Lymphadenopathy and eosinophilia may also be present, as was the case in this patient.
Outcome of the case. The infestation was successfully treated with 3 oral doses of ivermectin, 200 µg/kg, administered 2 weeks apart and topical applications of permethrin cream. The patient’s history of recurrent sexually transmitted disease and the Norwegian scabies infestation suggested immunosuppression and possible HIV disease. Serologic examination determined the patient was seropositive for HIV. He was lost to follow-up. ■


