Cervical Spine Injuries in the Geriatric Patient
This article is the second in a continuing series on trauma care and the older adult. The first article of the series, “Trauma in the Elderly: Causes and Prevention,” was published in the January 2010 issue. This series will discuss the growing problem of trauma in the elderly, including its causes and possible ways to prevent it, care in the acute stages, and manifestations and treatment strategies when trauma involves the torso, spine, brain, and hip. Authors include skilled experts in the trauma field representing various specialties at the R Adams Cowley Shock Trauma Center at the University of Maryland Medical Center and the University of Maryland School of Medicine.
Introduction
Traumatic injuries to the spinal column and/or spinal cord can cause significant disability, morbidity, and mortality. Recent literature suggests that there is a misconception in the understanding of these injuries. Most think that these injuries occur in isolation and to adolescents or young adults. Jabbour et al1 report that recent epidemiological studies on patients with spinal cord injury (SCI) depict a bimodal distribution. The first peak occurs in adolescents and young adults as expected; the second peak, however, occurs in the elderly population (age > 65 yr). It is estimated that in the United States, the population of individuals older than age 65 years will double over the next 30 years. Traumatic injuries, and their complications, are the leading cause of unexpected death in this age group. Spinal cord and/or column injury account for a significant number of these traumatic injuries.
Epidemiology
It is estimated that the annual incidence of SCI in the United States is approximately 40 per million, or nearly 12,000 new cases per year. In the past, statistics have shown that SCI primarily affected young adults. The average age of injury was 28.7 years in the 1970s, with most injuries occurring between the ages of 16 and 30. As the population ages, however, we have seen an increase in the average age of injury as well. More recently, the National Spinal Cord Injury Statistical Center is reporting 40.2 years to be the average age at injury.2
Nearly 81% of SCIs occur in males. Most frequently affected are Caucasians (66.1%) and African Americans (27.1%). Two percent are of Asian descent, and the percentage of Hispanic patients affected has increased to over 8% since 2005.2 Motor vehicle crashes account for 42.1% of SCIs. Falls are the next most common cause, followed by acts of violence and recreational sporting events.
The expense of SCIs to both individuals affected and to society is astronomical. SCIs cost the nation an estimated $9.7 billion each year. The cost of living for a patient with a SCI varies according to the level and severity of injury. Patients with high tetraplegia (C1-C4) have a mean expenditure of $801,161 in the first year following injury and $143,507 each subsequent year.2 Lower levels of injury and incomplete injuries are associated with lower overall costs.
Although life expectancy has improved for patients with SCI over the past 20 years or so, it is still not at the level of life expectancy for those people without SCI. For a patient age 60+ with a SCI, the mean life expectancy is just under 18 years, as opposed to over 22 years for the general population. For low tetraplegics (C5-C8) over age 60 years, the mean life expectancy is only 10 years, and for high tetraplegics and ventilator-dependent patients with SCI, life expectancy is only 7.6 and 1.8 years, respectively.2 The first year of injury holds a higher mortality rate than subsequent years. In the past, renal failure was the leading cause of death among patients with SCI. With the improvements in urologic care, this is no longer the case. Currently, the leading causes of death are pneumonia, pulmonary emboli, and septicemia.2
Spine Fractures and Spinal Cord Injuries in Older Adults
Falls are the leading cause of spinal column/cord injury in the elderly followed by motor vehicle crashes. The mechanism involved is often of much lower velocity than in younger patients. There are many factors that predispose the elderly population to these injuries, including osteoporosis, changes in bone density, osteopenia, the development of spinal stenosis, the propensity to fall due to sensory deficits and medications, and an increased rate of motor vehicle crashes per miles driven. Chronic conditions in elderly patients can also contribute to risk factors. Some of these include: diabetes causing peripheral neuropathy; and osteoarthritis, which can contribute to immobility, difficulty maneuvering, and less core stability. Other neurologic disorders such as Parkinson disease can cause rigidity, decreased movement initiation, cognitive impairments, and impaired sensation. Many medications that elderly persons take can cause postural hypotension and impair coordination and sensation, all of which can contribute to a mechanism causing spinal injury.1,3,4
Although there are many types of injuries to the spinal column/cord, this article will focus on those most relevant to the elderly population. Older patients sustaining injury to the spinal column/cord tend to sustain incomplete neurologic injuries, as opposed to complete injuries. This is likely due to the less severe mechanism of injury.1 Upper cervical injuries are the most common location of fractures and SCIs in the elderly population.5 There are three types of injury that appear to be relatively specific to the elderly population: (1) central cord syndrome; (2) cervical extension/distraction injuries; and (3) odontoid fractures.1
Central Cord Syndrome
 Central cord syndrome (CCS) is a disorder of the spinal cord that is thought to occur primarily in the elderly population. It is due to hyperextension of the neck. The elderly are more prone to this because of cervical spondylosis. Patients with CCS tend to have a disproportionate weakness in their upper extremities as compared to their lower extremities. Many of these patients do not have any associated fractures of their cervical vertebrae (Figure 1).
Central cord syndrome (CCS) is a disorder of the spinal cord that is thought to occur primarily in the elderly population. It is due to hyperextension of the neck. The elderly are more prone to this because of cervical spondylosis. Patients with CCS tend to have a disproportionate weakness in their upper extremities as compared to their lower extremities. Many of these patients do not have any associated fractures of their cervical vertebrae (Figure 1).
Because these patients do not have any fractures and their mechanism is thought to be of low velocity, they are often initially misdiagnosed. Treatment of this injury may include surgical fixation or external immobilization. Risks and benefits of both must be evaluated before a decision is made. Some patients with CCS will have some recovery of function over time, but it is felt that surgical decompression of the spinal cord will maximize recovery and prevent repeated SCI.1 Currently in the literature there is much discussion over the timing of when to perform this surgery. The surgery that is typically performed in patients with this injury is laminectomy, either with or without fusion.
Cervical Extension/Distraction Injuries
Cervical extension/distraction injury is another type that disproportionately affects the elderly population. This occurs because older individuals tend to have stiffness in their spinal column as their disc spaces collapse, and many have osteophyte formation as a result of degenerative spondylosis. All of this leads to decreased range of motion in the cervical spine. If an elderly patient presents with abrasions on his/her forehead or face and describes a hyperextensive injury, one should be highly suspicious of a cervical extension or distraction injury. These fractures are also referred to as “open book” fractures because they are associated with an opening or lengthening of the anterior column of the spine.1
Cervical extension or distractive fractures can often be overlooked because radiographs tend to display only minimal changes. Initial reads may indicate prevertebral soft-tissue swelling or distraction in a spondylitic disc space. If there is any question as to the presence of a fracture, a magnetic resonance imaging (MRI) scan should be obtained. An MRI can confirm the diagnosis because it tends to be more sensitive to soft tissue, ligament, and disc injury. An MRI will also demonstrate any injury to the spinal cord. These fractures are considered unstable, and most patients require surgical fixation and external immobilization. It is important to treat these patients with extreme care because any manipulation can worsen the fracture and potentially cause SCI.
Odontoid Fractures
Odontoid fractures are the third type of spine injury relatively unique to the elderly patient population. This is a fracture of the C2 vertebral body, specifically the odontoid process (Figure 2). These fractures usually occur from falling and hitting the head. Although these fractures can cause neurologic deficit, the majority of patients do not present with this. This is felt to be due to the generous width of the spinal column at this level, which allows for fracture displacement without spinal cord impingement. The goal in treating this injury is to protect the spinal cord while aligning the spinal column to promote stability and to decrease pain.1 Many of these patients are treated with external fixation in a rigid cervical collar or halo vest. A halo vest tends to cause significant mobility and respiratory issues in elderly patients, and therefore some surgeons will choose to do internal fixation in this population. Inhospital mortality rates in patients with these types of fractures are disproportionately high, however, often due to the morbidity of immobilization in elderly patients.

Stabilization of Fractures
Definitive treatment for the elderly population with spine fractures is a matter of some debate in the literature. Halo vest immobilization and surgical repair each carry a significant risk of morbidity. Jabbour et al1 state that immobilization of this population, despite use of a halo vest, still has a less than 70% union rate. Additionally, halo vest immobilization has its own set of complications in the elderly population. Some of this complications include: mobility issues; respiratory issues such as atelectasis and pneumonia; skin breakdown; pressure sores; pin-site irritation (loosening of the pins or infection of the site itself); and swallowing issues, which can lead to decreased nutritional intake in a population that already is at high risk for malnutrition. Majercik et al6 report that elderly patients placed in halo vest immobilization had high rates of cardiac and pulmonary morbidity and mortality. They also state that elderly patients treated in a halo vest have significantly higher mortality than younger patients. Halo vest immobilization in elderly patients showed an increase in “death, pneumonia, and acute cardiac or respiratory failure than elderly patients treated with surgery or in a hard collar.” Fassett et al3 found that elderly patients treated with halo vest immobilization had a 20-fold increase in mortality rates.
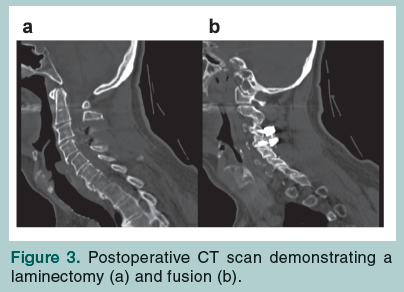
In elderly patients with multiple trauma, neurologic deficit, and/or fractures that are more than six weeks old, operative internal fixation remains a viable option. The majority of the literature on surgical fixation of cervical fractures in elderly patients has been retrospective with varied results reported.1 Advanced age is well known to negatively influence fracture healing, despite optimal immobilization or surgical management. Malik et al5 suggest that the management of cervical spine injuries is complicated in elderly patients due to a number of factors including pre-existing medical conditions, inability to tolerate halo vest immobilization, and reduced rate of fusion (Figure 3).
Acute Management
Despite the advances that have been made in medical treatment for a wide variety of conditions over the years, marked advances in the management of patients with SCI have been slow in coming. Due to an improving pathophysiologic understanding of the injury, however, guidelines for management of patients with SCI have been developed that not only guide acute management, but help to establish future directions to guide research efforts.7,8 Management of elderly patients with spinal injuries must take into account their pre-existing conditions, pathophysiologic characteristics, and age-related disorders that affect the population. The literature has indicated that elderly patients with spinal column/cord injury have increased morbidity and mortality as compared to younger patients with similar injuries.1,3-5,9
When caring for any patient with a SCI in the acute setting, the primary goal of treatment is to prevent secondary injury to the spinal cord. Primary injury occurs at the time of impact, and there is nothing that can be done to reverse that damage. The goal of caring for patients with acute cervical SCI is to stop the biochemical cascade of events that can cause “secondary injury,” which causes additional insults to the spinal cord resulting in more neurologic deficit.
In the acute care setting, the first and most important concern is early establishment of adequate airway, oxygenation, and ventilation. All patients with spinal injury are at risk for airway compromise. Early elective intubation is preferred, rather than waiting until loss of airway necessitates emergent intubation in a patient with an unstable cervical SCI. Local edema, parasympathetic stimulation causing an increase in secretions, decreased innervation of chest and abdominal muscles that inhibits generation of an adequate cough, and ventilation all contribute to airway compromise and respiratory failure.10,11 In elderly patients with underlying medical conditions, these difficulties are exaggerated. Data have suggested that over 90% of patients with cervical SCI will require mechanical ventilation.12 Fassett et al3 suggest that elderly patients with complete SCI are more likely to require tracheostomy than younger patients with the same injury. It is well known that patients who are ventilated have an increased chance of developing pneumonia and atelectasis, as well as pleural effusions, pulmonary edema, and pulmonary embolism. Additionally, patients who are ventilated have a suppressed cough reflex, further compromising respiratory status. In the patient with injury to the spinal cord, these issues are exacerbated by lack of innervation causing additional ventilatory compromise.
The goal is to prevent respiratory complications and promote oxygenation and spinal cord perfusion in order to prevent secondary injury.10 Some of the ways in which this is accomplished is with early mobilization as soon as the spinal column is stabilized and the patient is cleared to get out of bed. Chest physiotherapy also helps in preventing atelectasis and promoting gas exchange. In the acute care setting, the goal is to maintain the arterial oxygen saturation rate of greater than 90%.7 Early tracheostomy may also help facilitate weaning patients from the ventilator if their level of injury allows liberation from mechanical ventilation.
Cardiovascular complications include hypotension. Hypotension can be a result of neurogenic shock; however, often due to the nature of their traumatic injuries, other injuries resulting in hypotension secondary to hemorrhage need to ruled out. The goal in treating hypotension is to maintain a mean arterial pressure (MAP) of greater than 85 mm Hg to adequately perfuse the spinal cord.7 This strategy of intentional hypertension becomes more complicated in the elderly patients because many of them have pre-existing cardiac history and will not tolerate an increased MAP or the vasoactives required to maintain this level of systemic perfusion. Bradycardia can also be a complication of SCI. This is thought to be related to the interruption of the sympathetic nervous system. Due to unopposed vagal stimulation, even simple tracheal suctioning of patients may cause bradycardia. Many elderly patients are often on pre-injury beta blockers, calcium-channel blockers, or antiarrhythmic agents, which may further exacerbate bradycardia.
Other complications that occur frequently in patients with SCI include deep vein thrombosis (DVT) and gastrointestinal (GI) complications. Patients with SCI are at high risk of DVT due to immobility. If left untreated, fatal pulmonary embolism can occur. Patients should receive prophylaxis against DVT, with mechanical compression starting on admission and low-molecular-weight heparin as soon as it is deemed safe after injury or surgical stabilization. Prophylactic inferior vena caval filters are not recommended for prevention of DVT unless chemical prophylaxis is contraindicated.13 In our institution, per protocol, low-molecular-weight heparin is initiated 72 hours after injury or surgery. Care must be taken to adjust dosing accordingly in elderly patients with renal insufficiency, or to use unfractionated subcutaneous heparin as an alternate regimen.
Frequent GI complications include paralytic ileus and gastric or duodenal ulceration or gastritis leading to GI bleeding. Early use of high-dose methylprednisolone may contribute to the risk of GI bleeding complications. Many centers are no longer using high-dose steroids in the initial treatment of SCI. Some studies have suggested that high-dose steroids may result in neurologic improvement when started early in patients with SCI,14 but others question the benefits.15 Many feel that the risks of sepsis, pneumonia, and GI complications outweigh the benefits of steroid use and do not use them for patients with SCI.8,16 Due to the risk of stress ulcerations and GI bleeding, all patients with SCI are given histamine receptor antagonists or proton pump inhibitors. Tube feeding should be initiated as quickly as possible to help prevent ulcer formation and maximize nutritional status.
Due to the risk of paralytic ileus, patients with SCI should have a naso- or orogastric tube placed initially to decompress the stomach. This reduces the risk for vomiting and aspiration. If an ileus develops, nasogastric decompression should be continued until it is resolved, usually within 72 hours. Attempts at enteral nutrition with postpyloric tube feedings may be attempted and are usually well tolerated.
Bowel function may also be compromised depending on the level of injury. This is important to keep in mind with the elderly population because many older patients have issues with chronic constipation prior to their injury. It is important to start these patients on an aggressive bowel regimen with stool softeners and prokinetic agents. Manual disimpaction should be performed as needed.
All patients with SCI should have an indwelling Foley catheter to promote bladder emptying. Urinary output should also be monitored. It is important to note that patients with SCI may have oliguria related to sympathetic inactivity during the acute phase.10 Fluid resuscitation should be done carefully to minimize the risk of pulmonary edema while maintaining euvolemia. Many elderly patients may have pre-existing renal or urinary dysfunction that may be complicated by SCI.
Skin breakdown is a huge concern in any immobilized patients. Integumentary issues such as pressure ulcers can occur as a result of immobility, decrease in sensation, and muscle atrophy. Patients’ skin should be assessed frequently, and patients should be repositioned no less than every 2 hours.17 When patients are out of bed they should still be getting pressure relief by lifting or adjusting positioning. Heel protectors should be provided to relieve pressure. Some patients may also develop skin breakdown on their chin from cervical collars that may be needed for spinal immobilization. Collars should be removed and the area of skin under the collar should be assessed, cleansed, and dried before reapplication of the collar. Patients should remain flat in bed, or cervical immobilization should be applied when removing the collar. The back of the collar should remain intact when removing the front, and vice versa.
Long-Term Management
General practitioners who manage patients with SCI in the community need to consider the impact of the SCI as well as the pre-existing conditions that many older patients have. Some of the complications that are relatively unique to patients with SCI in the chronic phase of their injury include bladder dysfunction, GI dysfunction, and autonomic dysreflexia (AD).
Because SCI disrupts bladder control, patients with these injuries may have an indwelling catheter for years, or they may perform clean intermittent catheterization. Depending on the level of injury and the dexterity of the patient, intermittent catheterization is often possible. It is important to monitor the intake and output of patients before initiating an intermittent catheterization program. Patients should be aware of their fluid status and expect to have an equal intake and output. Intermittent catheterization may be more difficult for the elderly patient because of decreased manual dexterity related to arthritis and compounded by SCI. Poor vision may also further exacerbate these difficulties.
These patients, whether they have an indwelling catheter or perform clean intermittent catheterization, are at high risk for urinary tract infections, nephrolithiasis, epididymo-orchitis, and urethral strictures. Rarely, bladder cancer can occur.18 Some patients may present without any or with minimal symptomatology, however, due to lack of sensation and muscle dysfunction. It is important to remember that elderly patients with SCI are also at risk of the same conditions that affect the general population but may have minimal symptoms; therefore, a full evaluation should always be performed.
Bowel dysfunction after SCI is exceptionally common. Many of these patients experience constipation, bloating, and fecal incontinence. Bowel distention can also occur in these patients but may not be associated with abdominal pain or discomfort due to lack of sensation from their SCI. It is important that these patients are maintained on an individualized bowel regimen and that it is reviewed frequently. Again, when caring for the elderly patient with SCI, a careful review of pre-injury bowel dysfunction should be discussed, as the symptomatology he/she previously experienced may be masked by his/her injury.
AD is a life-threatening syndrome that can affect any patient with SCI at the level of T6 or above.10,18,19 It is triggered by noxious stimuli that occur below the level of injury. This stimulus triggers activity of the sympathetic nervous system, which produces severe vasoconstriction and increases blood pressure. Parasympathetic activity then produces vagal stimulation, bradycardia, and vessel dilatation.18 Patients may also present with acute sweating and headache.19
AD can be caused by a wide variety of stimuli, most commonly, bladder distention, urinary tract infections, constipation, or pressure ulcers, and, less commonly, from acute illnesses such as fractures or appendicitis.18 The first-line therapy for AD is recognition of the inciting event and prompt treatment of the noxious stimuli. A classic example of this is a patient who is assisted out of bed who suddenly develops symptoms of AD. The patient is assessed, and the clinician realizes that the Foley catheter is kinked, causing bladder distention. By unkinking the catheter, the bladder can then drain and the patient’s symptoms subside.
If a patient presents with AD it is important not to leave him/her alone. Ask the patient if he/she knows what is precipitating the event. Loosen tight clothing while checking for a cause, monitor blood pressure every five minutes, remove noxious stimuli, and administer medication if needed for increased blood pressure. First-line agents should be direct vasodilators. Beta blockers should be avoided to prevent unopposed alpha-receptor stimulation and worsening of hypertension. AD can be potentially life-threatening. If it is left untreated or unrecognized, patients may develop intracranial hemorrhage, encephalopathy, seizures, and/or cardiac dysrhythmia, which can lead to death.18
It is important for the primary care physician to remember that in addition to the disease processes that are relatively specific to the patient with SCI, common diseases still commonly occur in the patient with SCI and should be considered. Due to lack of sensation, many patients with SCI often will not present with the same signs and symptoms as a patient without SCI, which came make diagnosis of diseases even more challenging.
Conclusion
As the baby boomer population continues to age, the incidence of SCI in elderly patients increases. Although data suggest that there is an increase in morbidity in elderly patients with SCI that precludes successful recovery, the medical community must strive to develop appropriate medical management for these patients.9 Many elderly patients with SCI have incomplete injuries and can recover significant neurologic function. It is the responsibility of healthcare providers to give them the opportunity to do so.
In a study done by Furlan et al,20 it was determined that “age does not adversely affect neurological recovery assessed by motor and sensory function at acute or chronic stages following SCI.” Although mortality was higher in the elderly within all the stages of SCI, postmortem spinal cord tissue from spinal cord–injured and uninjured individuals showed that elderly and younger individuals do not significantly differ in the number of axons within the sensory, motor, and autonomic spinal cord tracts at high thoracic level. This indicates that elderly patients can have neurological recovery despite their age. Although the elderly do have a significant increase in mortality as compared to younger patients with SCI due to low physiologic reserve and pre-existing conditions,9 it is very possible for elderly patients to live with SCI when provided with the proper preventive care and early and aggressive treatment of complications.
The authors report no relevant financial relationships.
Ms. Aresco is from the R Adams Cowley Shock Trauma Center, University of Maryland School of Medicine, Baltimore. Dr. Stein is Chief of Critical Care, R Adams Cowley Shock Trauma Center, and Associate Professor of Surgery, Department of Surgery, University of Maryland School of Medicine. Dr. Gambert is Professor of Medicine and Co-Director, Division of Gerontology and Geriatric Medicine, Department of Medicine, University of Maryland School of Medicine, Director of Geriatric Medicine, University of Maryland Medical Center and R Adams Cowley Shock Trauma Center, and Professor of Medicine, Division of Gerontology and Geriatric Medicine, Johns Hopkins University School of Medicine, Baltimore, MD.


