Aplasia Cutis Congenita
A boy of 40 weeks’ gestational age was born via primary cesarean delivery due to recurrent late decelerations to a 33-year-old mother. The pregnancy had been otherwise uneventful. The newborn cried at birth, with an Apgar score of 9 at 1 minute and 9 at 5 minutes.
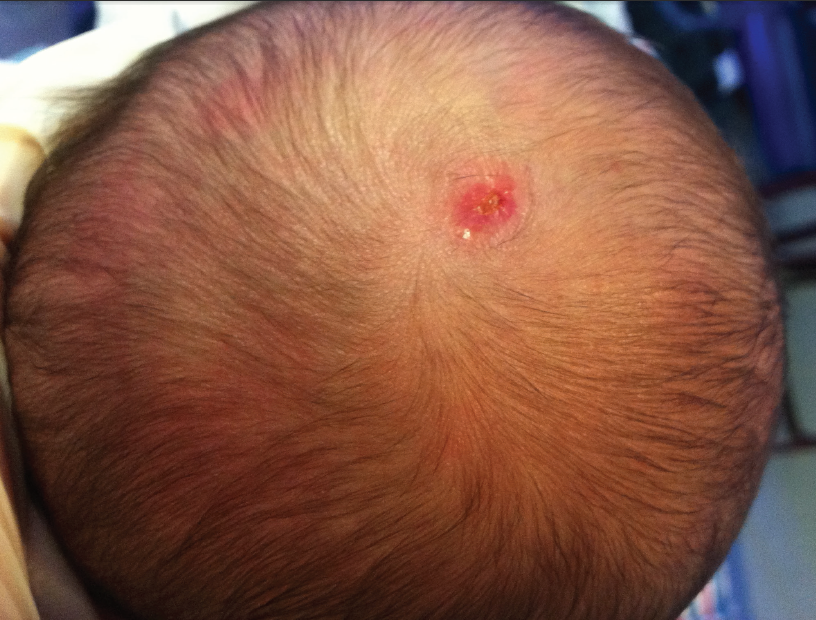
On examination in the delivery room, a round area of alopecia on the scalp with a healed skin defect of approximately 1 cm was noted. The lesion was at the lambdoid suture’s midline, extending to the right of the midline. No other lesions were noted on the newborn’s body. Physical and neurological examination findings were normal. Results of ultrasonography of the head were unremarkable. After initially ruling out iatrogenic causes, a diagnosis of isolated aplasia cutis congenita was made.
 Aplasia cutis congenita is a rare congenital defect in which skin, usually on the scalp (84% of cases), does not close completely.1 Depending on the extent of developmental arrest of the skin, the appearance of the lesion can vary from a superficial, circular, atrophic scar with alopecia to an ulcer extending down to the bone. These lesions are first noticed immediately after birth and usually present as solitary lesions near the vertex of scalp, lateral to the midline. However, they also can appear on the face, trunk, and limbs.2
Aplasia cutis congenita is a rare congenital defect in which skin, usually on the scalp (84% of cases), does not close completely.1 Depending on the extent of developmental arrest of the skin, the appearance of the lesion can vary from a superficial, circular, atrophic scar with alopecia to an ulcer extending down to the bone. These lesions are first noticed immediately after birth and usually present as solitary lesions near the vertex of scalp, lateral to the midline. However, they also can appear on the face, trunk, and limbs.2
The incidence is approximately 1 in 10,000 births.3 The etiology of this condition is unclear; however, genetic components, teratogens, amniotic adhesions, vascular anomalies, pharmacologic agents (eg, methimazole, benzodiazepines), and intrauterine trauma have all been implicated.4-6 A mutation in the GTPase BMS1 coding protein that delays 18S ribosomal RNA maturation and consequently reduces cell proliferation recently has been linked to aplasia cutis congenita.7
Aplasia cutis congenita can be accompanied by other congenital malformations. It is classified into 9 groups in accordance with coexisting anomalies as follows8: no other anomalies (as in our case), group 1; transverse defects of the limbs, group 2; epidermal and sebaceous nevi, group 3; central nervous system abnormalities, group 4; fetus papyraceus, group 5; blistering or skin fragility, group 6; and any other malformation syndromes, group 9. Lesions that present only on the limbs without accompanying scalp lesions are classified as group 7, and lesions caused by teratogens (eg, drugs, viruses) are categorized into group 8.
Suspected cases of aplasia cutis congenita call for immediate ultrasonography to evaluate for any accompanying intracranial malformations. If the diagnosis is uncertain, dermatoscopy can be performed to determine whether hair follicles are present.9
Treatment usually involves a conservative approach for less severe cases such as ours. Such cases usually resolve within weeks to months, but alopecia tends to persist. Surgical excision can be performed for lesions that fail to heal or for any cosmetic reason.10 Surgical repair using skin flaps and grafts is recommended for severe cases, such as those extending down to the dura mater, to prevent any hemorrhage and infection.11,12
References:
1. Demmel U. Clinical aspects of congenital skin defects. I. Congenital skin defects on the head of the newborn. Eur J Pediatr. 1975; 121(1):21-50.
2. Morelli JG. Cutaneous defects. In: Kliegman RM, Stanton BF, St. Geme JW III, Schor NF, Behrman RE, eds. Nelson Textbook of Pediatrics. 19th ed. Philadelphia, PA: Elsevier Saunders; 2011:2220-2222.
3. Casanova D, Amar E, Bardot J, Magalon G. Aplasia cutis congenita: report on 5 family cases involving the scalp. Eur J Pediatr Surg. 2001;11(4):280-284.
4. Kruk-Jeromin J, Janik J, Rykała J. Aplasia cutis congenita of the scalp: report of 16 cases. Dermatol Surg. 1998;24(5):549-553.
5. Moros Peña M, Labay Matías M, Valle Sánchez F, Valero Adán T, Martín-Calama Valero J, Muñoz Albillos M. Aplasia cutis congenita in a newborn: etiopathogenic review and diagnostic approach [in Spanish]. An Esp Pediatr. 2000;52(5): 453-456.
6. Iljin A, Kruk-Jeromin J. Aplasia cutis congenita. Adv Clin Exp Med. 2010;19(1):121-125.
7. Marneros AG. BMS1 is mutated in aplasia cutis congenita. PLoS Genet. 2013;9(6):e1003573.
8. Frieden IJ. Aplasia cutis congenita: a clinical review and proposal for classification. J Am Acad Dermatol. 1986;14(4):646-660.
9. Neri I, Savoia F, Giacomini F, Raone B, Aprile S, Patrizi A. Usefulness of dermatoscopy for the early diagnosis of sebaceous naevus and differentiation from aplasia cutis congenita. Clin Exp Dermatol. 2009;34(5):e50-e52.
10. Galbraith SS. Neonatal dermatology. In: Rudolph CD, Rudolph AR, Lister GE, First LR, Gershon AE, eds. Rudolph’s Pediatrics. 22nd ed. New York, NY: McGraw-Hill; 2011:chap 357.
11. Kim CS, Tatum SA, Rodziewicz G. Scalp aplasia cutis congenita presenting with sagittal sinus hemorrhage. Arch Otolaryngol Head Neck Surg. 2001;127(1):71-74.
12. Shivakumar SK, Dwarakanath S, Swaroop G, Venkataramana NK. Aplasia cutis congenita of the scalp: therapeutic modalities. Neurol India. 2006;54(3):312-313.
Deepak M. Kamat, MD, PhD—Series Editor:Dr Kamat is professor of pediatrics at Wayne State University in Detroit. He is also director of the Institute of Medical Education and vice chair of education at Children’s Hospital of Michigan, both in Detroit.


