Peer Reviewed
Anisocoria
Authors:
Diego Kriger, MD; Jana Zawadzki-Longtine, MD; Jane S. Kim, MD; Sarah Strube, DO; and Ignacio Carrillo-Nunez, MD
St. Mary Medical Center, Long Beach, California
Citation:
Kriger D, Zawadzki-Longtine J, Kim JS, Strube S, Carrillo-Nunez I. Anisocoria. Consultant. 2017;57(5):316-317.
A 66-year-old male veteran with a history of posttraumatic stress disorder, alcohol dependence, intravenous drug use disorder, and bipolar disorder was admitted to the intensive care unit for atrial fibrillation with rapid ventricular response and delirium tremens.
On presentation, the patient was noted to have bruising around his left eye, with the face being otherwise symmetric. Computed tomography (CT) scans showed nondisplaced fractures of the medial wall of the left orbit, left maxillary sinus, and left zygomatic arch. On physical examination, the patient had full range of extraocular movements. His pupils were equal, round, and reactive to light, and no nystagmus was noted.
The patient was stabilized and downgraded to the hospital floor for continued management. The patient remained encephalopathic for 2 weeks. Because the patient’s baseline condition was unknown, it was unclear whether he was exhibiting signs and symptoms of a stroke, or of psychosis associated with bipolar disorder, or of withdrawal from alcohol.
Magnetic resonance imaging (MRI) scans of the brain were obtained under anesthesia because the patient was extremely agitated. He required 15 mg of midazolam and 490 mg of propofol to achieve adequate sedation to obtain readable-quality images. The patient was monitored closely throughout the procedure, and his vital signs remained stable. The patient then was sent to the postanesthesia care unit (PACU) for further monitoring given the large amount of propofol required for sedation.
Within 15 minutes of arrival to the PACU, an isolated right anisocoria with mild left-sided facial droop was noted on physical examination (Figure), without evidence of any other obvious focal neurologic signs. Pupils were midline. The right pupil was 6 mm without consensual or direct response to light; the left pupil was 2 mm with normal response to light. A complete neurologic examination could not be obtained given that the patient was still very sedated, nonverbal, and unarousable and thus was unable to follow commands. However, the Babinski sign was negative bilaterally, and no posturing was elicited on examination. Arterial blood gases, serum glucose level, and CT of the head without contrast were obtained, the results of all of which were negative for any acute processes.
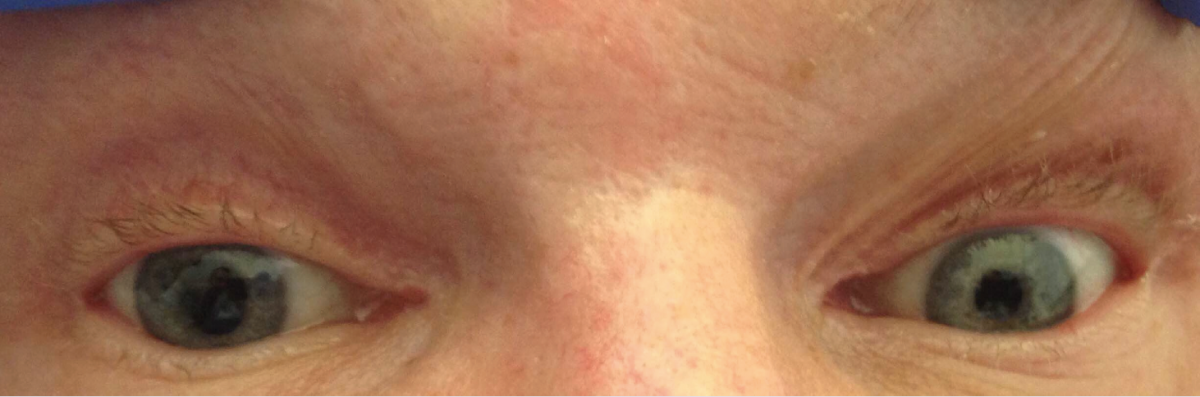
The patient was transferred back to the floor under close monitoring; his right-sided anisocoria resolved 30 hours later, and his left-sided facial droop resolved 48 hours later. Findings of a complete neurologic examination were also normal.
Discussion. Anisocoria, also known as unilateral mydriasis, can be a critically important clinical finding in patients given that it has been associated with severe, life-threatening neurologic conditions such as cerebral herniation, intracranial masses, acute intracranial hemorrhage, Horner syndrome, and other space-occupying lesions compressing cranial nerves.
Several published reports support the rare association between anisocoria and the use of pharmacologic agents such as propofol during general anesthesia for major surgical procedures requiring endotracheal intubation.1-4 However, no reports have described anisocoria associated with the unmasking of a previously sustained but undiagnosed stroke in a patient receiving propofol for sedation but who was not undergoing a major surgical procedure and did not require endotracheal intubation, as occurred in our patient’s case.
Given the spontaneous resolution of the patient’s signs and symptoms, and given the negative results of diagnostic tests, we believe that the right-sided anisocoria was associated with the relatively large quantity of propofol used for sedation, whereas the mild left-sided facial droop was likely secondary to the unmasking of a previously unknown stroke found on brain MRI.
No facial droop was present on initial admission or throughout his hospital course until sedation with propofol. Furthermore, the left-sided facial droop was consistent with an upper motor neuron pattern of injury and was therefore unlikely to be secondary to facial trauma. The patient had a symmetric face on initial presentation because of compensatory muscle tone, which was lost after generalized muscle relaxation was induced by high doses of propofol—a scenario that has been reported by other groups.5
In the setting of anisocoria in critically ill patients in whom a physical examination is difficult, clinicians should act quickly to exclude acute and emergent neurologic conditions, such as cerebral herniation, stroke, and intracranial tumors.6 However, clinicians should be aware that isolated anisocoria and the unmasking of a prior stroke can occur in the setting of sedation with propofol.
REFERENCES:
- Inchingolo F, Tatullo M, Abenavoli FM, et al. Severe anisocoria after oral surgery under general anesthesia. Int J Med Sci. 2010;7(5):314-318.
- Nesioonpour S, Khiabani K, Hassanijirdehi M. Unilateral mydriasis after mandibular fracture fixation surgery. Anesthes Pain Med. 2014;4(2):e13831.
- Sobel AM. Anisocoria during general anesthesia. Anesth Analg. 1965;44(5):522-526.
- Akhlaghi M. Anisocoria under general anesthesia with propofol. J Basic Res Med Sci. 2016;3(4):1-3.
- Lieutaud T, Billard V, Khalaf H, Debaene B. Muscle relaxation and increasing doses of propofol improve intubating conditions. Can J Anaesth. 2003;50(2):121-126.
- Yalcin S, Pampal K, Erden A, Oba S, Bilgin S. Do we really need to panic in all anisocoria cases in critical care? Indian J Anaesth. 2010;54(4):365-366.


