Adolescent Acne Vulgaris: An Overview of Therapeutic Options
ABSTRACT: Although acne vulgaris generally is considered to be benign and self-limited, it may cause severe psychological problems and disfiguring scars in pediatric patients who develop the condition. Understanding the epidemiology, pathogenesis, clinical presentation, and complications of acne vulgaris helps guide appropriate treatment to offer the best cosmesis and minimize scarring. Therapeutic options include topical medications, oral medications, and physical modalities such as peels, laser therapy, and dermabrasion.
A 16-year-old white adolescent was concerned because of unsightly lesions on his face. The lesions first started when he was 13 years of age, and they waxed and waned. In the past 2 years, the lesions had become more numerous and more bothersome. He had tried many over-the counter products that had helped temporarily. The patient was on no other medications. He was socially withdrawn because of the lesions and the resultant scars. His past health was unremarkable.
Physical examination revealed multiple comedones, papules, and pustules on the adolescent’s face (Figure 1). Some atrophic scars also were present. Physical examination findings were otherwise unremarkable.
This patient has acne vulgaris with resulting scars. He initially was treated with a regimen of oral antibiotics and a topical combination acne product, with good results, followed a few months later with a course of oral isotretinoin, which appeared to have stopped the acne completely. He also underwent a series of treatments for his scarring including dermastamp and ablative fractional laser resurfacing, with minor residual scarring.

Figure 1: The multiple comedones, papules, and pustules on this adolescent’s face, along with the resultant atrophic scarring, had led the 16-year-old to become socially withdrawn.
ACNE VULGARIS OVERVIEW
Acne vulgaris is a disorder of the pilosebaceous unit caused primarily by increased sebum production, hyperkeratinization of the follicle, bacterial colonization, and inflammation. Although generally considered to be a benign, self-limited condition, acne may cause severe psychological problems and disfiguring scars, as illustrated in the present case.
EPIDEMIOLOGY and Pathogenesis
The prevalence of acne in boys increases from 40% at age 12 years to 95% at age 16 years.1 In girls, the prevalence increases similarly from 61% to 83%.1 Predisposing factors include genetic predisposition, stress, premenstruation, the use of topically applied occlusive preparations, and the use of certain medications (eg, anabolic steroids, hydantoin).2
Acne is a chronic inflammatory process of the pilosebaceous unit. It usually occurs with the onset of puberty, due to increased production of androgens. Obstruction of the pilosebaceous canal is caused by hyperkeratinization of the follicle, hypertrophy of the sebaceous gland with increased production of sebum, and shedding of keratinocytes in clumps, which may be under the influence of androgens.1,3,4 When the normal flow of sebum onto the skin surface is obstructed by follicular hyperkeratosis, a microcomedo is formed. As the sebum accumulates, the microcomedo enlarges into a visible comedo.2
In the pilosebaceous gland, triglycerides are hydrolyzed into free fatty acids and glycerol by lipase produced by Propionibacterium acnes, which increases dramatically at the time of puberty.1 The free fatty acids, once released into the skin through follicular breakdown, are cytotoxic and contribute to the inflammatory reaction.1,4 Cytokines, chemokines, and defensins then are produced by the recruited inflammatory cells.
CLINICAL MANIFESTATIONS
Acne manifests most commonly in areas of the body that have abundant sebaceous glands, such as the face and, to a lesser extent, the back and chest.1 The initial stage of the disease begins with the pathognomonic comedo, which may be either open or closed.4 An open comedo, also called a blackhead, is a flat or slightly raised black lesion, measuring 1 to 3 mm in diameter. The black surface of the open comedo is melanin, not dirt or oxidized fat.1 A closed comedo, commonly known as a whitehead, appears as a white or flesh-colored, slightly elevated papule without a readily visible central pore. It is flask-shaped, with the narrowest portion connected to the skin surface.
Blackheads generally do not become inflamed unless the pilosebaceous canal is disrupted by external forces, such as may occur by squeezing the lesion; thus, patients are advised not to “play” with their lesions. Whiteheads may open up their pores, resulting in blackheads, or they may rupture. With rupture of the obstructed follicle and release of free fatty acids into the surrounding tissue, an inflammatory reaction ensues, resulting in erythematous papules, pustules, nodules, or cysts, depending on the amount and location of the tissue involved and the magnitude of the inflammatory response.1,4
Acne conglobata, found predominately in males, is a severe, destructive, and highly inflammatory form of acne marked by the presence of multiporous comedones, nodules, cysts, abscesses, and draining sinus tracts on the upper trunk and posterior back with resultant scarring.1
Acne fulminans is a rare form of acne characterized by the abrupt onset of large, necrotic, ulcerating, nodulocystic and suppurative lesions on the back and chest in association with systemic manifestations such as fever, chill, malaise, weight loss, musculoskeletal pain, and polyarthralgia.1,4
DIFFERENTIAL DIAGNOSIS
The diagnosis is mainly a clinical one. Acne should be differentiated from bacterial folliculitis, miliaria, perioral dermatitis, and rosacea.3
COMPLICATIONS
Postinflammatory hyperpigmentation and hypopigmentation may result, with dark-skinned individuals having a higher risk. Scarring may result, especially with severe variants such as acne conglobata and acne fulminans. In general, the deeper the inflammatory process, the more likely it will result in permanent scarring.1 Scarring can vary from small, deep, punched-out pits (“icepick” scars) and “boxcar” scars to deep furrows, keloids, and hypertrophic scars.5 Acne’s occurrence on the face is apt to be embarrassing and psychologically traumatic, and it may result in depression, anxiety, and low self-esteem.2,6 Self-consciousness related to acne can have an adverse effect on dating, participation in social activities, and quality of life.1
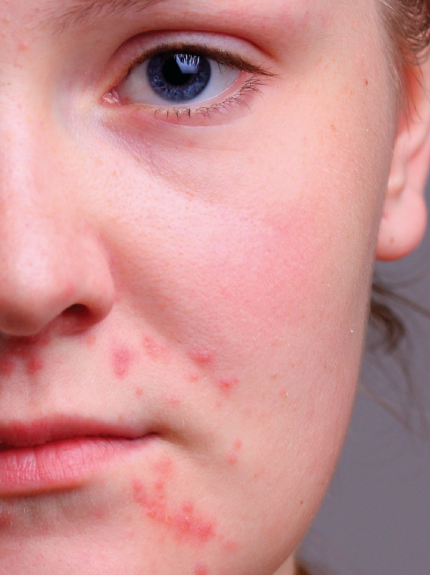
Figure 2: Although it is generally considered benign, acne may cause severe psychological problems and disfiguring scars in adolescents with it.
MANAGEMENT
The goals of treatment are to provide the patient with the best appearance possible and to minimize scarring. The aims of therapy are to prevent follicular hyperkeratosis, reduce P acnes, inhibit sebum secretion and fatty acid production, and eliminate comedones.1 In general, topical treatments are the first line of treatment for mild to moderate acne and can be used as combination therapy for more severe acne.2
Topical retinoids are the treatment of choice in cases of mild acne.7 These agents reduce obstruction of the follicle and have a marked anti-inflammatory effect.2 The major side effects are dryness, erythema, a burning sensation, and irritation.1 Depending on the severity of the acne, topical retinoids may be used alone or in combination with another agent such as benzoyl peroxide and topical or oral antibiotics.7,8 Retinoid dosing should be slowly titrated up to minimize irritation, which may impact adherence.
Antibiotics should not be used as monotherapy; combination therapy with topical retinoids or benzoyl peroxide will provide better results and reduce antibiotic resistance.8 Topical antibiotics that have been used successfully and are available for the treatment of acne include erythromycin and clindamycin.3
Benzoyl peroxide is a potent topical antimicrobial with rapid bactericidal action.1 The bactericidal effect on P acnes is due to the oxidation of bacterial proteins. Benzoyl peroxide inhibits the lipolysis of sebum triglycerides and decreases the inflammation of acne lesions.1 In addition, benzoyl peroxide has a keratolytic and comedolytic effect.3,7
A short course of topical (and occasionally oral) corticosteroids may be helpful in treating severe acute inflammatory lesions. Fluorinated corticosteroids should not be used, since they may cause corticosteroid acne in susceptible individuals.
Oral antibiotics are an important therapy for the more inflammatory types of acne lesions, including pustules, cysts, and abscesses.1 They should be used in combination with a topical retinoid or benzoyl peroxide.7 Tetracycline-class agents and erythromycin, administered systemically, produce a significant reduction in P acnes. In addition, they have intrinsic anti-inflammatory properties, exerting their action through the inhibition of neutrophil chemotaxis and alteration of macrophage and cytokine production.7
Oral isotretinoin decreases sebum production, follicular keratinization, and intrafollicular concentration of P acnes.1 In addition, it has a direct anti-inflammatory effect. The medication usually is reserved for more severe cases of acne but often is used in moderate cases where scarring is evident or other treatments have failed.8 Adverse effects are dose-related and include cheilitis, xerosis, conjunctivitis, pruritus, epistaxis, drying of the nasal mucosa, and dry mouth. Other adverse reactions include alopecia, photosensitivity, nausea, vomiting, palmoplantar desquamation, musculoskeletal symptoms, delayed wound healing, headache, and increased intracranial pressure.1 Laboratory abnormalities associated with the use of isotretinoin include hypertriglyceridemia, hypercholesterolemia, abnormal liver function test results, elevated erythrocyte sedimentation rate, thrombocytosis, anemia, and leukopenia.1 Because the medication has potential teratogenic effects, women of childbearing age should not be given oral isotretinoin until pregnancy has been excluded and an effective form of contraception is being used during treatment and for 1 month after stopping the medication.1,4
The use of estrogens in the form of oral contraceptives in the treatment of acne is based on the ability of estrogen to suppress the stimulatory effect of androgens on sebum production. Typically, they should be used in females older than 16 years of age with moderate to severe, recalcitrant, pustulocystic acne that does not respond to conventional therapy, as well as in those with polycystic ovary syndrome.1
Several physical modalities can help manage acne scars.1 Chemical peels and microdermabrasion can be used to treat superficial scars, preferably after acne has been controlled. Trichloroacetic acid, α-hydroxyl acid, retinoic acid, salicylic acid, and combination chemical peels (eg, Jessner peel) have been used with success in this regard.9 Dermabrasion can help treat superficial scars if it is carried out carefully. Deeper scars can be smoothed by dermal fillers such as hyaluronic acid, polymethyl methacrylate, and autologous fibroblasts.9 Other options include ablative and nonablative fractional lasers, dermaroller and dermastamp, radiofrequency, punch excision, and subcision.9
Alexander K. C. Leung, MD, is a clinical professor of pediatrics at the University of Calgary and a pediatric consultant at the Alberta Children’s Hospital in Calgary.
Benjamin Barankin, MD, is medical director and founder of the Toronto Dermatology Centre.
Kam-Lun Ellis Hon, MD, is a professor of pediatrics at the Chinese University of Hong Kong.
References
1. Leung AKC. Acne. In: Leung AKC, ed. Common Problems in Ambulatory Pediatrics: Specific Clinical Problems. Vol 2. New York, NY: Nova Science Publishers; 2011:275-282.
2. Basak SA, Zaenglein AL. Acne and its management. Pediatr Rev. 2013; 34(11):479-497.
3. Dawson AL, Dellavalle RP. Acne vulgaris. BMJ. 2013;346:f2634.
4. Hon KLE, Leung AKC. Acne: Causes, Treatment and Myths. New York, NY: Nova Science Publishers; 2010:1-89.
5. Krowchuk DP. Managing adolescent acne: a guide for pediatricians. Pediatr Rev. 2005;26(7):250-261.
6. Magin, P, Adams, J, Heading G, Pond D, Smith W. Psychological sequelae of acne vulgaris: results of a qualitative study. Can Fam Physician. 2006;52(8):978-979.
7. Zaenglein AL, Thiboutot DM. Expert committee recommendations for acne management. Pediatrics. 2006;118(3):1188-1199.
8. Sandoval LF, Hartel J, Feldman SR. Current and future evidence-based acne treatment: a review. Expert Opin Pharmacother. 2014;15(2):173-192.
9. Rose AE. Therapeutic update on acne scarring. J Drugs Dermatol. 2014;13(6):651-654.


