6-Year-Old Girl With Painful Oral Lesion
What's Your Diagnosis?
Sharpen Your Physical Diagnostic Skills

HISTORY
A 6-year-old girl with painful oral lesion. The pain intensified when she ate or drank anything sour or salty. She had similar painful lesions in the oral cavity before. No history of trauma.
PHYSICAL EXAMINATION
Afebrile child. Oral mucosal ulcer, with circumscribed margin, erythematous halo, and yellow floor. Physical examination findings otherwise normal. In particular, she had no enlarged cervical lymph nodes and no rash on the palms or soles.
WHAT'S YOUR DIAGNOSIS?
What's Your Diagnosis?
ANSWER: APHTHOUS STOMATITIS
Aphthous stomatitis (also known as aphthous ulcers, aphthae, or canker sores) is one of the most painful ulcerative conditions affecting the oral mucosa of children.1-3
EPIDEMIOLOGY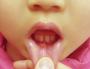 About 1% of children in developed countries—up to 40% of children and teens (15 years or younger) worldwide—may have a history of aphthous stomatitis.4 In the United States, aphthous stomatitis is 3 times more common in whites than in African Americans.2 The condition is slightly more common in females.4 Onset during childhood, particularly during adolescence, is common; severity and frequency tend to diminish with age.3,5
About 1% of children in developed countries—up to 40% of children and teens (15 years or younger) worldwide—may have a history of aphthous stomatitis.4 In the United States, aphthous stomatitis is 3 times more common in whites than in African Americans.2 The condition is slightly more common in females.4 Onset during childhood, particularly during adolescence, is common; severity and frequency tend to diminish with age.3,5
ETIOLOGY
Most cases are idiopathic and occur in otherwise healthy children.1,6 Although the exact cause is unknown, it is probably multifactorial with various precipitating factors. A genetic predisposition has been shown by an increased frequency of certain human leukocyte antigen subtypes and a positive family history in some affected patients.2,4,7,8 The most likely precipitating factors are stress and local trauma.2,5,9 Predisposing factors that might account for recurrent aphthous stomatitis in a minor subset of patients include hormonal changes (related to the onset of menstruation or luteal phase), hematinic (iron, vitamin B12, folic acid) deficiencies, and drugs (NSAIDs, ß-blockers).4
CLINICAL MANIFESTATIONS
A localized burning sensation or pain that lasts 24 to 48 hours may precede the ulceration.9 Aphthous stomatitis is characterized by painful, solitary or multiple ulcers, which are round or oval, with well defined erythematous margins and a central yellowish-gray fibrinous pseudomembrane.5 The lesions usually develop on the nonkeratinized oral mucosa (buccal and labial mucosa, floor of the mouth, or ventral surface of the tongue).5,6 They rarely occur on the tongue dorsum, hard palate, or gingiva.6
Aphthous stomatitis can be classified according to its clinical characteristics3:
•Minor aphthae, the most common variety, account for 80% to 85% of all aphthae.3 These ulcers are superficial, small (less than 1 cm), and few (less than 3 lesions); they heal without scarring within 10 days.10
•Major aphthae (Mikulicz aphthae, Sutton aphthae, periadenitis mucosa necrotica) are deeper and larger (greater than 1 cm) than minor aphthae.3,10 These lesions have a predilection for the lips, soft palate, and fauces.7 The ulcers usually develop at puberty.8 Major aphthae often take longer than 2 weeks to resolve and sometimes heal with scar formation.
•Herpetiform aphthae, the least common variety, are characterized by multiple recurrent crops of 10 or more small (1 to 3-mm) ulcers that may coalesce into larger irregular ulcers.3,9,11 Age of onset is usually in the second or third decade of life.3,8 An individual lesion heals within 7 to 10 days with no scar formation.4
Aphthous lesions are rarely documented as a single episode in the clinical history of patients; recurrence is the hallmark of the disease.3 The oral ulcers generally have a periodic course and are thus described as recurrent aphthous stomatitis.3
DIAGNOSIS
There is no specific diagnostic test for aphthous stomatitis. Clinicians should perform a detailed history and complete physical examination to rule out systemic disease, which may be associated with aphthous-like ulceration.
Aphthous stomatitis must be differentiated from herpetic gingivostomatitis, herpes labialis, and herpangina as well as hand, foot, and mouth disease. Aphthous-like ulceration can be found in systemic disorders, such as Behçet disease, Reiter disease, Crohn disease, ulcerative colitis, gluten-sensitive enteropathy, and immunodeficiency syndromes. Such immunodeficiency syndromes include cyclic neutropenia or HIV infection, PFAPA syndrome (periodic fever, aphthous stomatitis, pharyngitis, and cervical adenitis), MAGIC syndrome (mouth and genital ulcers with inflamed cartilage), and Sweet syndrome (acute febrile neutrophilic dermatosis).1,2,5,7
COMPLICATIONS
Aphthous stomatitis can cause considerable pain and may interfere with talking, eating, and swallowing.3 Dehydration from poor fluid intake is a potential major complication.
MANAGEMENT
The goals of treatment are to alleviate pain, expedite resolution, and prevent dehydration. This involves elimination of predisposing factors, when possible.
Patients should avoid foods that are hard, acidic, spicy, and salty as well as alcoholic beverages.12 They should also avoid teeth cleaning products and toothpastes that contain sodium lauryl sulfate.8,12
Simple measures to maintain good oral hygiene are important for symptom relief.11 Chlorhexidine gluconate mouthwash has been used to decrease mucosal pain and to prevent secondary infection of ulcers.
Topical analgesics, such as lidocaine, polidocanol, and benzocaine, can be used for pain relief. Systemic ibuprofen or acetaminophen can also be used if necessary.
Topical corticosteroids, such as triamcinolone and clobetasol, when used for a short period, have a safe profile and are the mainstay of treatment.6,7,11,13 These agents interfere with the formation of autoantibodies and stabilize lysosomes, thus reducing necrosis of the oral mucosa and inflammatory symptomatology.13 Triamcinolone acetonide dental paste with carboxymethylcellulose sodium is often the drug of choice; the tissue adhesive, which prevents the medication from being rapidly washed away, increases therapeutic efficacy.14 ■
REFERENCES
1. Oh SH, Han EC, Lee JH, Bang D. Comparison of the clinical features of recurrent aphthous stomatitis and Behçet’s disease. Clin Exp Dermatol. 2009;34:e208-e212.
2. Scully C, Porter S. Oral mucosal disease: recurrent aphthous stomatitis. Br J Oral Maxillofac Surg. 2008;46:198-206.
3. Femiano F, Lanza A, Buonaiuto C, et al. Guidelines for diagnosis and management of aphthous stomatitis. Pediatr Infect Dis J. 2007;26:728-732.
4. Natah SS, Konttinen YT, Enattah NS, et al. Recurrent aphthous ulcers today: a review of the growing knowledge. Int J Oral Maxillofac Surg. 2004;33:221-234.
5. Akintoye SO, Greenberg MS. Recurrent aphthous stomatitis. Dent Clin North Am. 2005;489:31-47, vii-viii.
6. Scully C. Aphthous ulceration. N Engl J Med. 2006;355:165-172.
7. Jurge S, Kuffer R, Scully C, Porter SR. Mucosal disease series. Number VI. Recurrent aphthous stomatitis. Oral Dis. 2006;12:1-21.
8. Messadi DV, Younai F. Aphthous ulcers. Dermatol Ther. 2010;23:281-290.
9. Gallo Cde B, Mimura MA, Sugaya NN. Psychological stress and recurrent aphthous stomatitis. Clinics. 2009;64:645-648.
10. Bruce AJ, Rogers RS 3rd. Acute oral ulcers. Dermatol Clin. 2003;21:1-15.
11. Bischoff EW, Uijen A, van der Wel M. Aphthous ulcers. BMJ. 2009;339:b2382.
12. Altenburg A, Abdel-Naser MB, Seeber H, et al. Practical aspects of management of recurrent aphthous stomatitis. J Eur Acad Dermatol Venereol. 2007;21:1019-1026.
13. Rodríguez M, Rubio JA, Sanchez R. Effectiveness of two oral pastes for the treatment of recurrent aphthous stomatitis. Oral Dis. 2007;13:490-494.
14. Eisenberg E. Diagnosis and treatment of recurrent aphthous stomatitis. Oral Maxillofac Surg Clin North Am. 2003;15:111-122.


