Young Woman With Weakness in Her Arms and Legs
A 20-year-old woman presents with weakness in her arms and legs. The symptoms began about 4 days earlier with tingling in her hands and feet and have progressed to the point of her stumbling frequently and dropping weighty objects. She is also having trouble with writing. She denies bowel or bladder symptoms, dizziness, dyspnea, or other difficulties in breathing.
HISTORY
She is an otherwise healthy young woman who lives in an apartment with friends while attending college. Her only medication is an oral contraceptive. She does state that she had a severe diarrheal illness 2 weeks earlier along with several of her roommates.
PHYSICAL EXAMINATION
Vital signs are normal; no postural changes to her pulse or blood pressure are noted. There is no nystagmus. Heart and lungs are normal. Rectal examination shows good sphincter tone. On neurological examination, cranial nerves are intact. The patient has symmetrical weakness of the arms and hands as well as the muscles of the legs. Reflexes are diffusely hyporeflexic to areflexic.
LABORATORY RESULTS
A complete blood cell count and blood chemistry test results are within normal limits. Arterial blood gas measurement shows a PaO2 level of 96 mm Hg and a PCO2 level of 41 mm Hg. A lumbar puncture is performed, with normal opening pressure. There are no cells in the cerebrospinal fluid (CSF), but the protein level is 170 mg/dL.
Which of the following statements about this case
is correct?
A. Immunization against herpes simplex viruses after recovery is indicated to prevent recurrences.
B. The prognosis at 6 months after recovery from the acute illness is uniformly good.
C. The most common epidemiologic association for the patient’s illness is infection with Campylobacter jejuni.
D. The optimal therapy during the acute illness is a course of high-dose corticosteroids initiated within 5 days of onset.

Correct Answer: C
The clinical scenario presented is that of Guillain-Barré syndrome. The patient experienced the typical prodromal symptoms of distal numbness, paresthesia and pain in her limbs, followed by relatively symmetrical progressive (“ascending”) weakness of the limbs. Physical findings revealed the common hyporeflexia/areflexia pattern. The CSF examination demonstrated the classic “albuminocytologic dissociation” in which the CSF protein level is elevated, often remarkably so, in the absence of a pleocytosis. In clinical practice, this combination of physical findings of acute peripheral neuropathy and typical CSF findings allows the presumptive diagnosis of Guillain-Barré syndrome. If nerve conduction studies are performed, they will demonstrate and confirm the symmetrical sensory and motor peripheral neuropathy.
EPIDEMIOLOGY
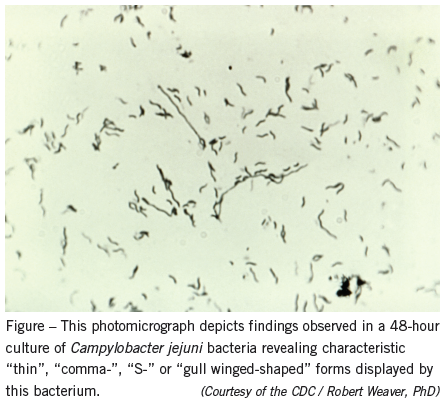
Ongoing research indicates an autoimmune cause for Guillain-Barré syndrome, very likely related to cross-reactive antibodies to components of a variety of microbial antigens.1 This fact correlates with the epidemiology of the syndrome. In two thirds of cases, a history of previous upper respiratory tract or diarrheal illness can be elicited. Meta-analysis has identified significant percentages of specific infections preceding a Guillain-Barré syndrome.1,2 The most common are C jejuni (30%), cytomegalovirus (10%) and, to a lesser extent, Epstein-Barr virus, varicella-zoster virus, and Mycoplasma pneumoniae.1,2 Thus, choice C is correct (Figure), while choice A (involvement, therapy, and prophylaxis for herpes simplex) is not.
TREATMENT
Therapeutics involve strict attention to general measures appropriate to neurologic disease and more specific immunotherapies. Decompensation of ventilation to the point of requiring mechanical ventilation is a major risk; thus, careful monitoring of vital capacity, hypercarbia, and hypoxemia is mandatory, as is evaluation of the risk of swallowing dysfunction and aspiration. Another significant morbidity in these patients is deep vein thrombosis and pulmonary embolism such that these patients should receive an effective prophylaxis regimen when they are unable to walk.
Specific treatment aimed at the presumed autoimmune pathogenesis involves a variety of immunotherapies. Good experience and data indicate that plasma exchange and intravenous immunoglobulin (IVIG) are equally and significantly effective at hastening recovery when administered within 2 weeks of disease onset.3 Counterintuitively, the corticosteroids prednisolone and methylprednisolone do not hasten recovery or affect long-term outcome when used alone nor do they enhance efficacy if added to plasmapheresis or IVIG therapy. Thus, choice D is not correct.
PROGNOSIS
The usual course of Guillain-Barré syndrome is stabilization and recovery within 28 days of onset. The clinical course is often quite hectic: 66% of patients cannot walk independently at the point of maximum weakness and 25% receive mechanical ventilation.1,2 And, the intermediate prognosis is also more guarded than usually appreciated, with 20% of severely affected patients still unable to walk 6 months after disease onset.1 Thus, choice B is far too optimistic and not correct. Happily, recurrences are quite uncommon once a patient has recovered from Guillain-Barré syndrome.
OUTCOME OF THIS CASE
The presumptive diagnosis of Guillain-Barré syndrome was confirmed by nerve conduction studies. Neurologic function and ventilation were carefully monitored, and stabilization occurred at 2 weeks without the need for ventilation. The patient required assistance with walking. Improvement began thereafter, and at 6 months she had completely regained normal neurologic function.
1.Yuki N, Hartung HP. Guillain-Barré syndrome. N Engl J Med. 2012;366:2294-2304.
2. van Doorn PA, Ruts L, Jacobs BC. Clinical features, pathogenesis, and treatment of Guillain-Barré syndrome. Lancet Neurol. 2008;7:939-950.
3. Hughes RAC, Swan AV, Raphael JC, et al. Immunotherapy for Guillain-Barré syndrome: a systematic review. Brain. 2007;130:2245-2257.


