What is the cause of this asymptomatic blister?

Case 1: For 2 weeks, an 87-year-old man has had an asymptomatic blister on the dorsum of the left hand. He has chronic renal failure and is receiving dialysis.
Which of the following would you include in the differential?
A. Porphyria cutanea tarda.B. Bullous disease of dialysis.
C. Photodrug reaction.
D. Bullous pemphigoid.
E. Lupus erythematosus.
Case 1: Bullous disease of dialysis
This patient had bullous disease of dialysis, B, which resembles porphyria cutanea tarda, A; both disorders are characterized by asymptomatic bullae that develop on sun-exposed areas of the hands. A serum test to detect elevated porphyrin levels is required to rule out porphyria cutanea tarda.
The cause of bullous disease of dialysis remains uncertain, although the location suggests a photosensitizing metabolite—other than porphyrin—that has not been identified. No standard therapy exists; however, there are recent reports of patients who responded to oral N-acetylcysteine after 1 to 2 months of treatment.1,2
Photodrug reactions, bullous pemphigoid, and lupus erythematosus are all symptomatic and usually involve multiple lesions. Moreover, bullous pemphigoid is not confined to sun-exposed surfaces. In patients with lupus erythematosus, the typical lupus lesions would usually be present in addition to the rare bullous lesions.
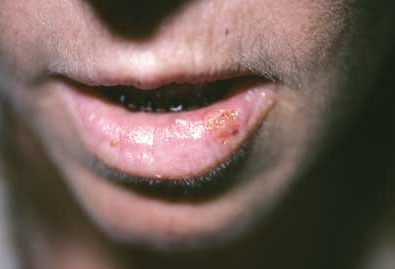
Case 2: A 48-year-old woman presents for treatment of a fever blister. This is a recurrent episode.
Which of the following statements is not true?
A. 80% of oral herpetic lesions are caused by herpes simplex virus type 1 (HSV-1).B. 80% of adults in the United States are seropositive for HSV-1.
C. Tzanck tests are highly reliable, with greater than 90% sensitivity.
D. Tzanck tests do not distinguish between HSV-1 and HSV-2.
E. Ultraviolet light can precipitate an outbreak of herpes simplex.
Which of the following treatments is not an appropriate choice?
F. At least 1 g of l-lysine daily.G. Application of acyclovir ointment every 2 hours while the patient is awake.
H. Valacyclovir, 500 mg bid, for 5 days.
I. Valacyclovir, 2 g bid, for 1 day.
J. Famciclovir, 250 mg bid, for 5 days.
K. Famciclovir, 1.5 g in a single dose.
Case 2: HSV-1 infection
Tzanck tests are sensitive less than 65% of the time in experienced hands and are not considered reliable. Thus,thestatementthat Tzanck tests are highly sensitive, C, is not true.
Acyclovir ointment, oral valacyclovir and famciclovir, and l-lysine1-3 are all appropriate treatment choices for HSV-1 infection.

Case 3: A 30-year-old man has a 3-year history of arthritis of unknown origin that finally responded to etanercept. He now presents with an asymptomatic rash of 2 months' duration that is distributed over the trunk and the extremities.
What is the most likely cause of the rash?
B. Tinea versicolor.
C. Pityriasis rosea.
D. Granuloma annulare.
E. Secondary syphilis.
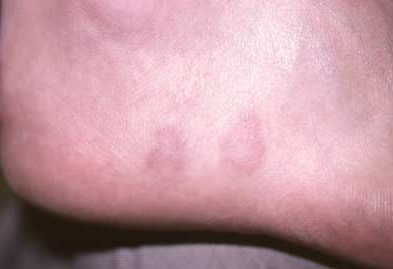
Case 3: Granuloma annulare
A skin biopsy confirmed the suspected diagnosis of granuloma annulare, D; it was not related to the patient's arthritis. The cause of granuloma annulare is unknown. Most treatments are ineffective for this condition, which runs a self-limited course before resolving.
The lesions of granuloma annulare are not scaly. All the other conditions in the differential (tinea corporis, tinea versicolor, pityriasis rosea, and secondary syphilis) are associated with scale.
1. Cooke NS, McKenna K. A case of haemodialysis-associated pseudoporphyria successfully treated with oral N-acetylcysteine. Clin Exp Dermatol. 2007;32:64-66.
2. Massone C, Ambros-Rudolph CM, Di Stefani A, Müllegger RR. Successful outcome of haemodialysis-induced pseudoporphyria after short-term oral N-acetylcysteine and switch to high-flux technique dialysis. Acta Derm Venereol. 2006;86:538-540.
3. Kagan C. Lysine therapy for herpes simplex. Lancet. 1974;1:137.
4. Griffith RS. A multicentered study of lysine therapy in herpes simplex infection. Dermatologica. 1978;156:257-267.
5. Griffith RS. Success of L-lysine therapy in frequently recurrent herpes simplex infection. Treatment and prophylaxis. Dermatologica. 1987;175:183-190.


