Peer Reviewed
Chickenpox
Author:
Nishit Harishbhai Patel, MD
Assistant Professor, Department of Pediatrics, Division of Pediatric Emergency Medicine, UT Southwestern Medical Center, Dallas, Texas
Citation:
Patel NH. Chickenpox [published November 14, 2018]. Consultant360.
A 10-month-old girl, who had been born prematurely at 33 weeks of gestation and had a history of failure to thrive, presented to the emergency department with a low-grade fever, malaise, decreased oral intake for 3 to 4 days, and a pruritic rash for 2 days. The rash had started on the torso, then had spread to the face and entire body. She had no known sick contacts. She had received her priming doses of immunizations and was up-to-date for her age.
Physical examination findings were unremarkable except for multiple papules and vesicles all over her body (Figures 1 and 2). The lesions were different stages of development and healing (maculopapular, pustular, vesicular, and crusting), and the lesions on the back appeared in crops—the classic “dewdrops on a rose petal” presentation of chickenpox.
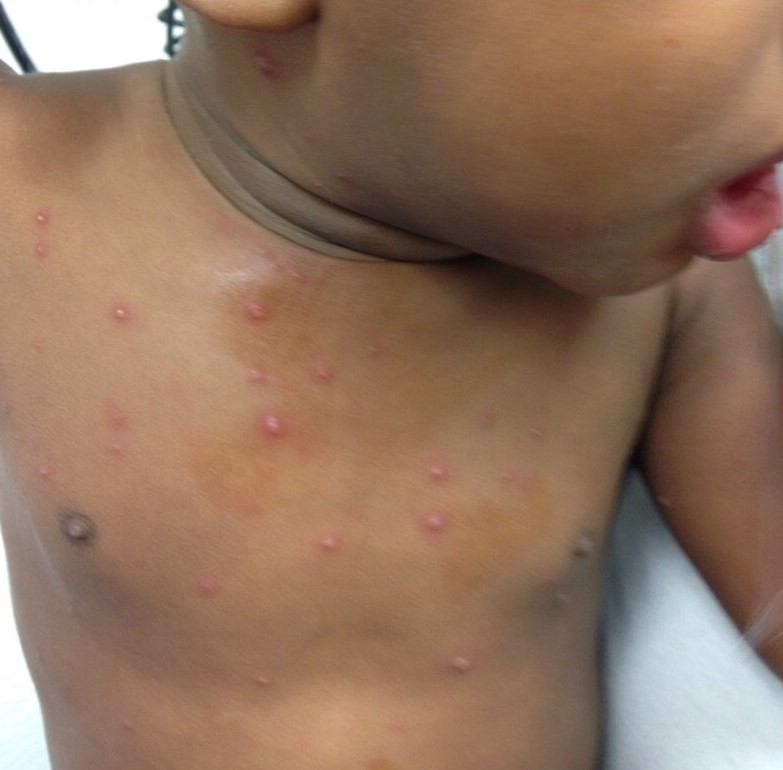
Figure 1. Lesions on the girl’s face and trunk in different stages of healing.

Figure 2. Lesions on the girl’s back appeared in crops, in different stages of healing.
Discussion. Chickenpox is caused by the varicella-zoster virus (VZV), a member of the Herpesviridae family. It is preventable and is now relatively uncommon, but it remains a highly contagious disease, spreading via direct contact, airborne droplets, and transplacental passage.1,2
Chickenpox manifests as a prodrome of fever, malaise, headache, and abdominal pain before the development of pruritic blister-like rashes that appear in centripetal distribution. The lesions are classically described as “dewdrops on a rose petal” in different stages of healing. Patients are contagious from 1 to 2 days before the onset of the rash until all lesions have crusted.1,2 The incubation period usually ranges from 10 to 21 days after exposure to the rash. Immunized children with breakthrough varicella typically have a milder disease course, with fewer than 100 to 200 lesions.
Our patient tested positive for VZV from a skin lesion sample using polymerase chain reaction testing, which is the current diagnostic method of choice.2
Varicella is usually a self-limited illness in healthy children, but it tends to have more complications and higher severity in adults, infants, and in immunocompromised persons. Complications can include bacterial superinfection of skin lesions, bacterial sepsis, pneumonia, neurologic complications (acute cerebellar ataxia, encephalitis meningitis, and demyelinating processes), thrombocytopenia, glomerulonephritis, arthritis, hepatitis, and Reye syndrome.1,2 The decision to use antiviral therapy should be determined by host factors such as immunosuppression, underlying medical conditions, and the extent of infection.2,3
Outcome of the case. Our patient received intravenous hydration and symptomatic therapy in the emergency department. She was subsequently admitted and treated with intravenous acyclovir while an inpatient, with transition to oral acyclovir to complete a 7-day course. After discharge, the patient had complete resolution of her rash in 2 weeks.
- Berkoff MC, Brown WD. Varicella After the perinatal period. Pediatr Rev. 2013;34(11):537-538.
- American Academy of Pediatrics. Varicella-zoster virus infections. In: Kimberlin DW, Brady MT, Jackson MA, Long SS, eds. Red Book: 2018 Report of the Committee on Infectious Diseases. 31st ed. Itasca, IL: American Academy of Pediatrics; 2018:869-88
- Harris D, Redhead J. Should acyclovir be prescribed for immunocompetent children presenting with chickenpox? Arch Dis Child. 2005;90(6):648-650.


