Peer Reviewed
What Is This Progressively Growing Lesion on a Man’s Lower Extremity?
AUTHOR:
Gregory A. Lawson, MD, MPHAFFILIATIONS:
1Sparrow Health System, Lansing Michigan
2Michigan State University, College of Human Medicine, Department of Family Medicine, East Lansing, MichiganCITATION:
Lawson G. What is this progressively growing lesion on a man’s lower extremity? Consultant. 2022;62(2):e12-e13. doi:10.25270/con.2021.04.00013Received December 28, 2020. Accepted January 12, 2021. Published online April 22, 2021.
DISCLOSURES:
The author reports no relevant financial relationships.CORRESPONDENCE:
Gregory A. Lawson, MD, MPH, Sparrow Medical Group Ionia, 500 South Washington Street, Ionia, MI 48846 (greggslawson@gmail.com)
A 62-year-old man presented to the clinic with an enlarging lesion on his left shin. The lesion had progressively grown in size and, in the last few weeks, has been associated with a yellowish discharge, which prompted the patient to seek care.
Six months prior to presentation, the patient had had a biopsy for a nonhealing ulcer, which he had developed after experiencing trauma to the shin, at the location of the current lesion. According to him, the initial lesion was about 1 cm in diameter. However, since the biopsy, the lesion has changed in size and characteristic.
The patient had a 25 pack-year smoking history and diagnoses of hypertension, hyperlipidemia, osteoarthritis, and chronic obstructive pulmonary disease. He denied pain, fever, and chills. His current medications included lisinopril, atorvastatin, and diclofenac sodium/misoprostol.
A physical examination was conducted, findings of which were significant for an approximately 3-cm violaceous, brownish plaque on an atrophic, telangiectatic base on the left shin (Figure). The lesion had a moderate amount of yellow crusting and perilesional erythema. No tenderness was appreciated on the lesion. Diminished pedal pulses bilaterally were also noted.
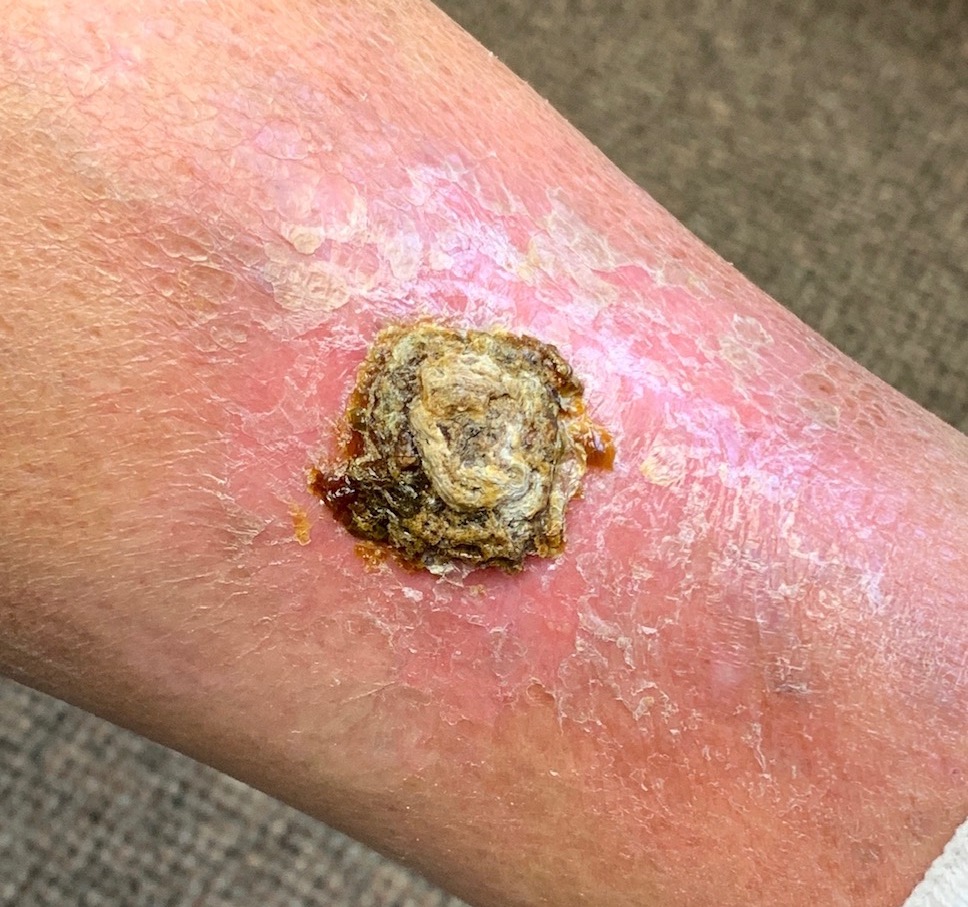
Answer and discussion on next page.


