Peer Reviewed
What Caused This 8-Year-Old Girl’s Limp?
AUTHORS:
Micah Kadden, MD1 • Sheri Balsara, MD2 • Chandani Patel DeZure, MD3AFFILIATION:
1Children’s National Health System, Washington, DC
2The Children’s Hospital of Philadelphia, Philadelphia, Pennsylvania
3Lucile Packard Children’s Hospital, Stanford University, Palo Alto, California
CITATION:
Kadden M, Balsara S, DeZure C. What caused this 8-year-old girl’s limp? Consultant. 2022;62(2);e14-e16. doi:10.25270/con.2021.06.00009Received January 22, 2021. Accepted April 23, 2021. Published online June 14, 2021.
DISCLOSURES:
The authors report no relevant financial relationships.CORRESPONDENCE:
Chandani DeZure, MD, Division of Neonatology, Center for Academic Medicine, Lucile Packard Children’s Hospital, MC: 5660, 453 Quarry Road, Palo Alto, CA 94304 (cdezure@stanford.edu)
An 8-year-old nonverbal autistic girl presented with her parents to our emergency department (ED) with a 6-week history of a progressively worsening limp. At onset, the patient had a mild limp, left-sided antalgic gait, avoidance of using the left leg, and expressed discomfort with its manipulation, according to her parents. She was admitted to the hospital for further evaluation of worsening limp.
History. She did not have a history of a musculoskeletal disorders or extremity pain. She had been referred to an orthopedist one month prior to presenting at the ED, at which time Sever disease was diagnosed and a walking boot was prescribed.
Her parents reported that the patient’s gait did not improve with the walking boot. Within 2 days of wearing the boot, she had developed a shuffling gait and a fever of 38.2 °C, which had resolved without intervention. Given her continued abnormal gait, new fever, and lack of improvement, an outpatient lower extremity magnetic resonance imaging (MRI) scan was performed by another health care provider, results of which were negative for acute process, according to the parents.
A review of systems revealed that the patient had always been below her optimal weight for her age. Her parents reported that the patient was as an extremely picky eater. Notably, during a recent dental visit, an oral lesion was identified and removed from her hard palate, after which her oral intake had decreased further. A biopsy specimen of the oral lesion was sent for pathology.
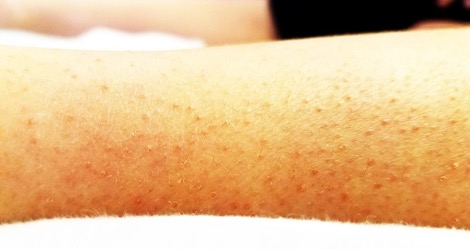
Over the 3 months prior to presentation, she had also developed a nonspecific diffuse red rash on the upper and lower extremities. The rash was not painful and was more prominent on the lower extremities (Figure 1). Even though the patient was nonverbal, she was able to sign a limited number of words and follow simple commands.
Physical examination. At presentation, she was afebrile with vital signs within the normal limits. The only significant finding was a low weight of 16.4 kg (0.04 percentile for age; body mass index, 0.9 percentile for age). An oral examination was notable for poor dentition with multiple visible caries and one pustular lesion located centrally along the palate near 2 appropriately healing biopsy sites.
The patient had full range of motion of the bilateral lower extremities without edema, erythema, or tenderness to palpation. Sensation and reflexes were within normal limits throughout. Ambulation demonstrated a slightly wide-based gait with small steps; she appeared visibly uncomfortable with ambulation.
Results of a dermatologic examination revealed diffuse perifollicular hyperkeratotic papules with surrounding petechiae and coiled hairs most prominent on the bilateral lower extremities (Figure 1).
Diagnostic testing. Results of a laboratory workup were significant for elevated levels of aspartate aminotransferase at 71 U/L, alanine aminotransferase at 63 U/L, and lactate dehydrogenase at 283 U/L. Results of a complete blood cell count (CBC), electrolyte panel, erythrocyte sedimentation rate (ESR), and uric acid test were all within normal limits. Previous outpatient testing for Lyme disease, antinuclear antibody, and rheumatoid factor were within normal limits.
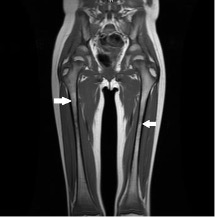
A repeat MRI scan of the bilateral lower extremities was performed because of the inability to obtain the previous MRI scan. Results showed bilateral low T1 and high T2 signal involving the metaphyses of the femurs, tibias, and fibulas (Figure 2). During the workup, the biopsy taken during the patient’s dental surgery returned results significant for a pyogenic granuloma caused by Actinomyces.
Answer and discussion on next page.


