Peer Reviewed
Subacute Hypertensive Urgency in a Healthy Young Man: Pheochromocytoma
Authors:
George Cockey, MD, PhD
Assistant Professor, University of Central Florida College of Medicine, Orlando, Florida; North Florida Regional Medical Center, Gainesville, Florida
Josue Hernandez, MD
Resident Physician, University of Central Florida College of Medicine, Orlando, Florida; North Florida Regional Medical Center, Gainesville, Florida
Angela Fernandez, MD
Resident Physician, University of Central Florida College of Medicine, Orlando, Florida; North Florida Regional Medical Center, Gainesville, Florida
Ranjit Banwait, MD
Resident Physician, University of Central Florida College of Medicine, Orlando, Florida; North Florida Regional Medical Center, Gainesville, Florida
Citation:
Cockey G, Hernandez J, Fernandez A, Banwait R. Pheochromocytoma. Consultant. 2019;59(11):350-351.
A 23-year-old man was referred to our hospital by his primary care physician due to headaches, palpitations, and recent-onset hypertensive urgency.
History. The man recently had presented to an outside hospital with headaches; he had received a diagnosis of hypertension and hypokalemia and had been sent home with hydrochlorothiazide. His primary care physician had arranged for a magnetic resonance imaging (MRI) scan of the brain; the results revealed sinusitis, which had been treated with amoxicillin-clavulanic acid. His headache, palpitations, diaphoresis and hypertension worsened, and he also reported feeling agitation and extreme weakness, so his primary care physician sent him to the hospital for admission and workup. He had no history of hypertension, and his parents denied a family history of hypertension.
Physical examination. At presentation, the patient was a thin man who appeared healthy but anxious. He reported the recent onset of diffuse headache, palpitations, diaphoresis, muscular spasms, and numbness in his extremities. His blood pressure was 181/120 mm Hg, with a pulse 93 beats/min. Physical examination findings were unremarkable, with normal pulses in the upper and lower extremities.
Diagnostic tests. Abnormal laboratory test results included a potassium level of 3.1 mEq/L (reference range, 3.5-5.1 mEq/L), a creatinine level of 1.55 mg/dL (reference range, 0.6-1.3 mg/dL), a total calcium level of 10.3 mg/dL (reference range, 8.5-10.1 mg/dL), an ionized calcium level of 3.8 mg/dL (reference range, 3.8-4.8 mg/dL), and a white blood count of 13,800/µL (reference range, 4500-11,000/µL). Results of a urine drug screen were negative for drugs of abuse, including cocaine, amphetamines, and phencyclidine.
Results of Doppler ultrasonography of the renal arteries were normal, but renal ultrasonography revealed a mass in either the liver or adrenal glands. A computed tomography (CT) scan of the abdomen revealed a 3.9 × 3.0 × 3.9-cm right adrenal mass. Subsequent MRI scans of the abdomen showed 4.6 × 2.9 × 3.6-cm right adrenal mass that was not consistent with adenoma.
Twenty-four-hour urine collection revealed a markedly elevated norepinephrine level of 2796 µg/24 h (reference range, 0-135 µg/24 h) and urine normetanephrine level of 9015 µg/24 h (reference range, 82-500 µg/24 h). Plasma norepinephrine and normetanephrine levels also were markedly elevated at greater than 23,440 pg/mL (reference range, 0-874 pg/mL) and 4050 pg/mL (reference range, 0-145 pg/mL), respectively. Twenty-four-hour urine collection results for cortisol were normal at 47 µg/24 h (reference range, 0-64 µg/24 h). All other secondary causes of hypertension (including normal thyrotropin and parathyroid hormone) were excluded except pheochromocytoma.
Phenoxybenzamine was not available, so doxazosin was initiated for 72 hours followed by propranolol to control his hypertension and tachycardia. Early intravenous hydration corrected his acute kidney insufficiency. The tumor was successfully removed via robot-assisted laparoscopic adrenalectomy (Figure).
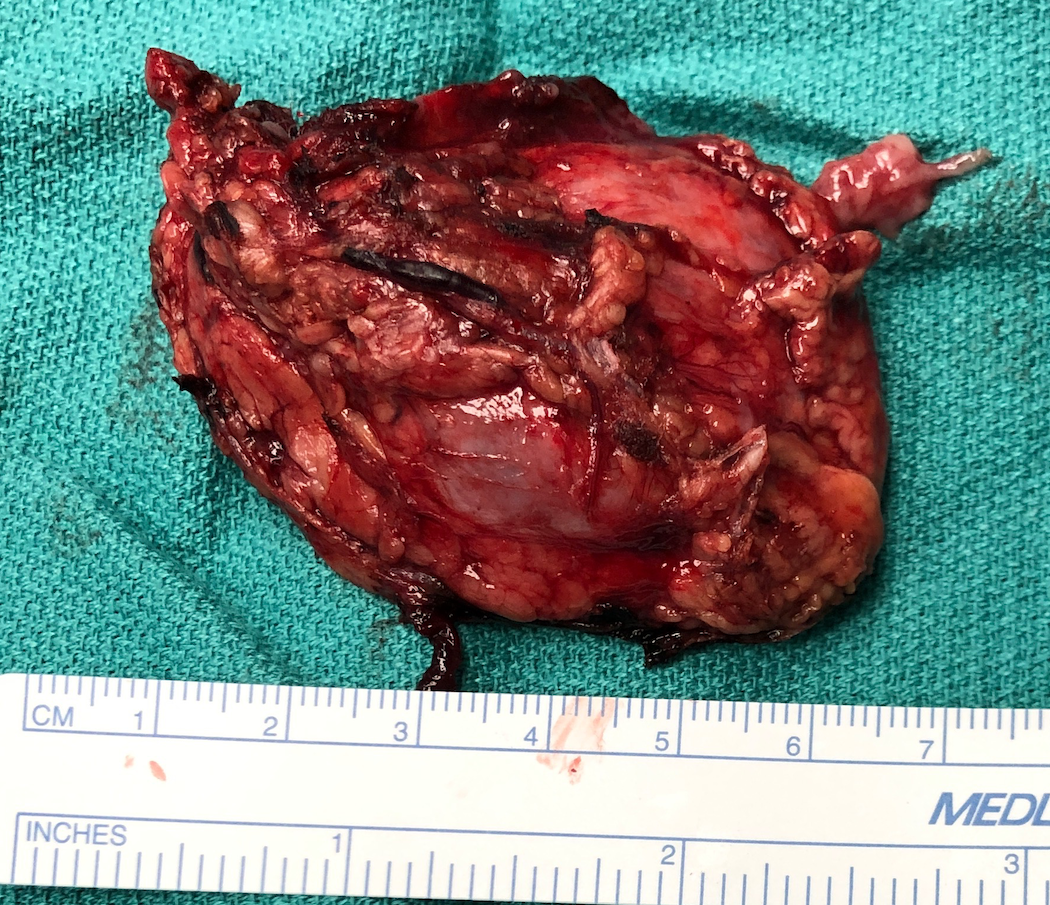
Figure. A large right adrenal mass was removed via robot-assisted laparoscopic adrenalectomy.
Postoperatively, the patient developed right-sided pneumothorax after central line placement, requiring chest tube placement, but he recovered from this and eventually was discharged home.
Discussion. Secondary causes of hypertension include the following: elevated levels of cortisol (Cushing syndrome) or aldosterone, bilateral renal artery stenosis, primary kidney disease, obstructive sleep apnea, coarctation of the aorta, hypothyroidism, primary hyperparathyroidism, and pheochromocytoma. A workup for secondary causes of hypertension was performed in our patient’s case due to his young age and the sudden onset of and lack of family history of hypertension.
Pheochromocytoma may present with paroxysmal hypertension, headache, diaphoresis, anxiety, and palpitations.1 Only approximately 50% of patients present with hypertension. However, orthostatic hypotension may be a diagnostic clue because of volume contraction associated with the catecholamine surge.2 Most pheochromocytomas are located in the abdomen, with approximately 85% in the adrenal glands.3 Today, some are found asymptomatically because of the frequency of CT scans.4
The most reliable diagnostic test is a 24-hour urine collection test for catecholamines and metanephrines (sensitivity, 97%; specificity, 98%), although plasma measurements may be preferred in high-risk patients.5
Laparoscopic adrenalectomy is the preferred treatment.6 However, preoperative medical treatment with α- and β-blockers, calcium-channel blockers, or metyrosine is required 10 to 14 days prior to surgery to help prevent hypertensive intraoperative crisis.7 Ideally, initiate treatment with α-blockers for the first 72 hours, followed by β-blockers to control hypertension and tachycardia. Avoid β-blockers initially, since they may aggravate hypertension. These patients tend to be volume-depleted because of catecholamine surge, so aggressive hydration and a high-sodium diet (>5 g/d) are warranted.7
REFERENCES:
- Gunawardane PTK, Grossman A. Phaeochromocytoma and paraganglioma. Adv Exp Med Biol. 2017;956:239-259.
- Stein PP, Black HR. A simplified diagnostic approach to pheochromocytoma: a review of the literature and report of one institution’s experience. Medicine (Baltimore). 1991;70(1):46-66.
- Gruber M, Därr R, Eisenhofer G. Pheochromocytoma: update on diagnosis and therapy [in German]. Dtsch Med Wochenschr. 2014;139(10):486-490.
- Kudva YC, Young WF Jr, Thompson GB, Grant CS, van Heerden JA. Adrenal incidentaloma: An important component of the clinical presentation spectrum of benign sporadic adrenal pheochromocytoma. Endocrinologist. 1999;9(2):77-80.
- Sawka AM, Jaeschke R, Singh RJ, Young WF Jr. A comparison of biochemical tests for pheochromocytoma: measurement of fractionated plasma metanephrines compared with the combination of 24-hour urinary metanephrines and catecholamines. J Clin Endocrinol Metab. 2003;88(2):553-558.
- Shen WT, Grogan R, Vriens M, Clark OH, Duh Q-Y. One hundred two patients with pheochromocytoma treated at a single institution since the introduction of laparoscopic adrenalectomy. Arch Surg. 2010;145(9):893-897.
- Butz JJ, Weingarten TN, Cavalcante AN, et al. Perioperative hemodynamics and outcomes of patients on metyrosine undergoing resection of pheochromocytoma or paraganglioma. Int J Surg. 2017;46:1-6.


