Peer Reviewed
Spontaneous Psoas Hematoma Secondary to Anticoagulation
AUTHORS:
Randa T. A. Abd Algayoum, MD1 • Zarak Hassan, MD1 • Mansi Singapori, MD1 • Narendra Khanchandani, MD2
AFFILIATIONS:
1Department of Internal Medicine, St. Mary Mercy Livonia Hospital, Livonia, Michigan
2Medical Director, Intensive Care Unit, St. Mary Mercy Livonia Hospital, Livonia, Michigan
CITATION:
Abd Algayoum RTA, Hassan Z, Singapori M, Khanchandrani N. Spontaneous psoas hematoma secondary to anticoagulation. Consultant. 2022;62(1):e17-e18. doi:10.25270/con.2021.04.00016
Received June 7, 2020. Accepted August 2, 2020. Published online April 29, 2021.
DISCLOSURES:
The authors report no relevant financial relationships.
CORRESPONDENCE:
Randa T. A. Abd Algayoum, MD, Department of Internal Medicine, St. Mary Livonia Hospital, 36475 Five Mile Rd, Livonia, MI 48154 (randatajaldeen.alsayed@stjoeshealth.org)
Spontaneous psoas hematoma is a rare but life-threatening complication that is associated with high rates of morbidity and mortality. The incidence of retroperitoneal hematoma as a complication of anticoagulation ranges from 1.3% to 6.0%.1 Specifically, the incidence of iliopsoas muscle hematoma is reported to range from 0.1% to 0.6%.2 Risk factors for retroperitoneal hematomas include anticoagulation, old age, and hemodialysis.2 The exact mechanism is unknown, but hypotheses include forceful muscular strain, diffuse small-vessel arteriosclerosis, and heparin-induced immune microangiopathy. We present a case of a woman who developed spontaneous retroperitoneal hematoma secondary to anticoagulation.
CASE PRESENTATION
A 72-year-old woman with a history of congestive heart failure, chronic lymphedema, and hypothyroidism presented with worsening bilateral lower-extremity swelling and weakness. She was found to be in atrial fibrillation, with rapid ventricular response. Physical examination revealed 3+ pitting edema in the bilateral lower extremities. Results of initial laboratory tests were unremarkable. She was started on heparin and diltiazem drips for management of new-onset atrial fibrillation, and she was admitted to the medical floor.
On the night of admission, the patient experienced a syncopal episode secondary to hypotension. She was given a normal saline bolus, which led to improvement in her blood pressure. Laboratory tests revealed a drop in hemoglobin from 12 g/dL to 7.4 g/dL. The patient’s partial thromboplastin time was found to be supratherapeutic, and heparin was immediately discontinued. Computed tomography (CT) scanning of the abdomen and pelvis was requested. Shortly thereafter, she developed persistent hypotension that was unresponsive to fluid management. The patient reported having right leg pain, and examination revealed tenderness in the right lower abdominal quadrants. The patient was started on a norepinephrine drip and was transferred to the intensive care unit.
CT scans of the abdomen and pelvis demonstrated a large right abdominopelvic retroperitoneal hematoma, mostly involving the psoas muscle (Figure).
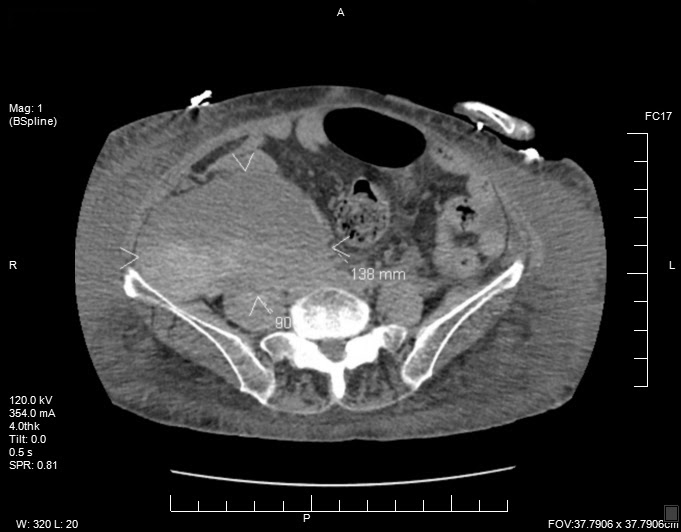
The patient required a total of 4 units of packed red blood cells. She was managed conservatively, did not require surgical intervention, and was weaned from pressors within 48 hours. Follow-up physical examination demonstrated the Grey Turner sign—ecchymotic lesions on the flanks that develop 24 to 48 hours after a retroperitoneal hemorrhage. Her symptoms improved, and her hemoglobin level stabilized.
The patient's hospital course was further complicated with hospital-acquired pneumonia and a congestive heart failure exacerbation requiring intravenous antibiotics and diuresis. The risks and benefits of anticoagulation were discussed with the patient, and the decision was made to hold off resuming anticoagulation therapy. The patient was discharged in stable condition to subacute rehabilitation and was advised to follow up with her primary care physician.
Discussion. Iliopsoas hematoma is a retroperitoneal collection of blood involving the iliopsoas, which refers to the combined psoas muscle and iliacus muscle. Patients with iliopsoas hematoma often present with nonspecific lower back pain, occasionally radiating to the thigh and groin area. In cases of large retroperitoneal hematomas, ecchymotic lesions in the flanks (Grey Turner sign) or in the periumbilical area (Cullen sign) may be noted, as in our patient’s case, and may progress to hypovolemic shock. The femoral nerve is one of main branches of the lumbar plexus. It forms within the psoas muscle and runs laterally above the inguinal ligament. It courses down between the iliopsoas muscle and behind the inguinal ligament into the thigh. It is susceptible to compression anywhere along its course, and patients can present clinically with one or more of the following symptoms: paralysis of the quadriceps, weakness of the Iliopsoas, loss of the knee jerk reflex, and paresthesias in the anteromedial aspect of the lower extremity.3 The first 2 cases of anticoagulant-associated iliopsoas hematoma were reported in 1966 by DeBolt and Jordan.4
CT is highly sensitive and is the most commonly employed diagnostic modality.4,5 Most cases of iliopsoas hematoma are managed conservatively with supportive therapy, allowing the hematoma to spontaneously resorb. Severe cases with profound neurological deficits or hemodynamic instability have been managed with angiographic evaluation followed by transcatheter arterial embolization.6 Surgical intervention is reserved for patients with failed angiographic procedures, concurrent surgical conditions, or with significant compressive symptoms on nervous system structures from hematoma formation.7
Early diagnosis of spontaneous psoas hematoma is crucial to avoid its potentially fatal sequelae. It should be considered in patients on anticoagulation therapy who present with sudden-onset back pain with no other plausible etiology. Our case highlights the importance of timely recognition and management of iliopsoas hematoma in patients on anticoagulation due to its subtle presentation and potential lethality.
References
1. Tosun A, İnal E, Keleş I, et al. Conservative treatment of femoral neuropathy following retroperitoneal hemorrhage: a case report and review of literature. Blood Coagul Fibrinolysis. 2014;25(7):769-772. doi:10.1097/MBC.0000000000000110
2. Llitjos JF, Daviaud F, Grimaldi D, et al. Ilio-psoas hematoma in the intensive care unit: a multicentric study. Ann Intensive Care. 2016;6(1):8. doi:10.1186/s13613-016-0106-z
3. DeBolt WL, Jordan JC. Femoral neuropathy from heparin hematoma: report of two cases. Bull Los Angeles Neurol Soc. 1966;31(2):45-50.
4. Giuliani G, Poppi M, Acciarri N, Forti A. CT scan and surgical treatment of traumatic iliacus hematoma with femoral neuropathy: case report. J Trauma. 1990;30(2):229-231. doi:10.1097/00005373-199002000-00019
5. Tamai K, Kuramochi T, Sakai H, Iwami N, Saotome K. Complete paralysis of the quadriceps muscle caused by traumatic iliacus hematoma: a case report. J Orthop Sci. 2002;7(6):713-716. doi:10.1007/s007760200127
6. Zissin R, Gayer G, Kots E, Ellis M, Bartal G, Griton I. Transcatheter arterial embolisation in anticoagulant-related haematoma—a current therapeutic option: a report of four patients and review of the literature. Int J Clin Pract. 2007;61(8):1321-1327. doi:10.1111/j.1742-1241.2006.01207.x
7. Sunga KL, Bellolio MF, Gilmore RM, Cabrera D. Spontaneous retroperitoneal hematoma: etiology, characteristics, management, and outcome. J Emerg Med. 2012;43(2):e157-e161. doi:10.1016/j.jemermed.2011.06.006


