Peer Reviewed
Patent Omphalomesenteric Duct Fistula
Authors:
Rachael Lester, MD
Department of Pediatrics, University of North Carolina, Chapel Hill, North Carolina
Rebecca Smith, MD
Department of Pediatrics, University of North Carolina, Chapel Hill, North Carolina
Sean McLean, MD
Division of Pediatric Surgery, University of North Carolina, Chapel Hill, North Carolina
Jacob Lohr, MD
Department of Pediatrics, University of North Carolina, Chapel Hill, North Carolina
Citation:
Lester R, Smith R, McLean S, Lohr J. Patent omphalomesenteric duct fistula. Consultant. 2019;59(4):120-121.
A newborn boy, who had been born at 39 weeks and 1 day of gestation via primary cesarean delivery due to transverse lie, was noted at delivery to have an enlarged umbilical cord.
Physical examination showed a large umbilical cord insertion with two translucent yellow-colored areas near the proximal end of the cord; the underside had darker areas but without evidence of bowel contents. The patient had a normal newborn nursery course and was discharged on day 2 of life with a recommended 24- to 48-hour follow-up visit. At the newborn follow-up with the pediatrician, the umbilical cord was noted to be very thick without surrounding erythema.
At 13 days of age, the patient presented to his pediatrician for evaluation of a residual thick umbilical stump (Figure 1).
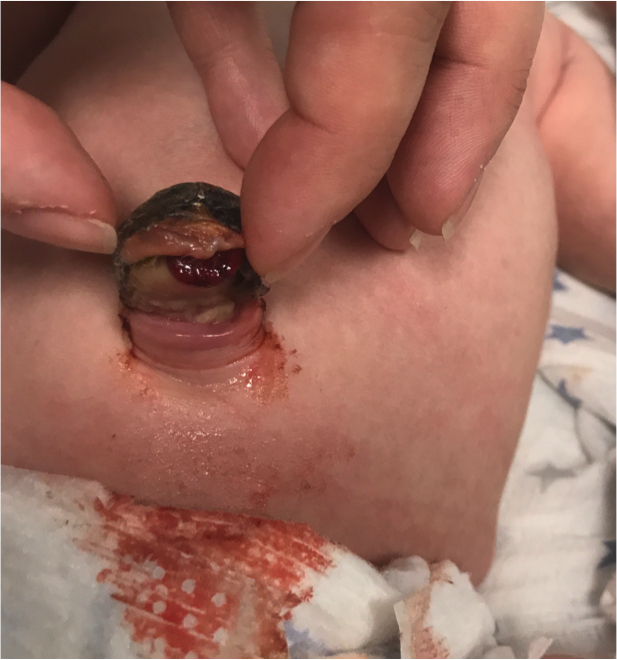
Figure 1. The newborn presented to his pediatrician at 13 days of age for a residual thick umbilical stump.
On examination, the cord appeared to be drying on the dorsal aspect, with the skin-abutting ventral aspect remaining soft and oozing rust-colored fluid, thought to be blood. The mother had noted a malodor but no surrounding erythema. At the office visit, the provider attempted to cinch the umbilical stump just above the skin; but application of an umbilical tie elicited immediate crying and thus was removed. The patient was sent to a pediatric surgery clinic for further evaluation (Figure 2).
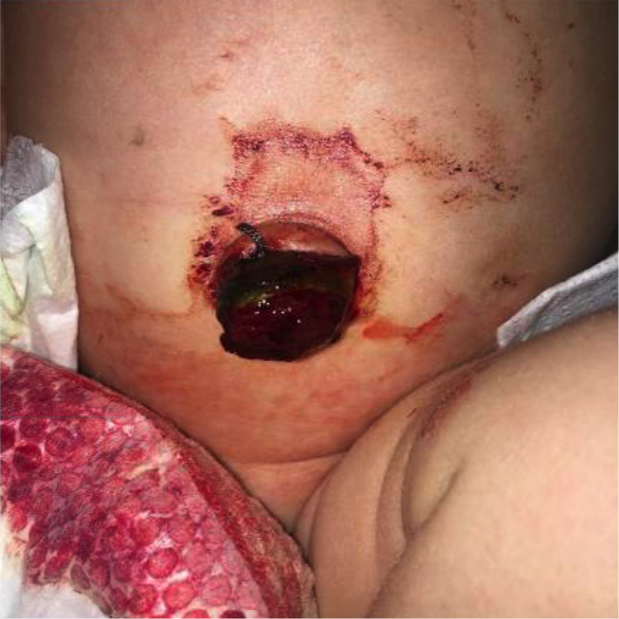
Figure 2. Umbilical stump at presentation to a pediatric surgeon due to persistent bleeding.
The patient later underwent surgical correction of the umbilical stump. Intraoperatively, it was noted that there was residual patent omphalomesenteric fistula connected to the skin. Pathological test results confirmed small bowel mucosa tracking to the surface of the specimen. Based on clinical presentation, intraoperative findings, and pathology findings, the newborn received a diagnosis of a patent omphalomesenteric duct (OMD) fistula.
The boy was seen 4 weeks postoperatively, at which time he was treated for surrounding cellulitis that was believed to have resulted from infected suture material, but otherwise he was doing well. He had an uneventful recovery with no further sequelae to date.
Discussion. The OMD is a temporary structure essential to normal fetal development, connecting the yolk sac to the primitive gastrointestinal tract in the developing embryo. Normally, the OMD completely involutes by week 9 of intrauterine life.1,2 OMD remnants are uncommon, with an occurrence rate of 2% and with the rarest being an OMD fistula,3,4 as in this patient’s case. There are no known risk factors, although many reports show a male predominance in symptomatic cases.3,4
The presentation of OMD varies depending on the degree and location of duct patency. Complete patency results in the OMD connecting the umbilicus to the terminal ileum. This can lead to intestinal drainage from the umbilicus, similar to a stoma, as in this patient’s case. A persistent OMD at the umbilicus but with no intestinal connection results in an umbilical sinus. Persistent tissue at the ileum with no connection to the umbilicus results in a Meckel diverticulum. Finally, patent OMD with closure at both ends results in an OMD cyst, which can lead to small bowel obstruction given that both ends are fixed.
Often, ultrasonography or a fistulogram may be required to visualize the anatomy. Symptomatic OMD remnants require surgical intervention, which is curative.
Given the risk of catastrophic outcome with ileum incarceration or strangulation, it is important that physicians remain vigilant and diagnose this abnormality to allow prompt surgical intervention.
- Cilley RE. Disorders of the umbilicus. In: Grosfeld JL, O’Neill JA Jr, Fonkalsrud EW, Coran AG, eds. Pediatric Surgery. Vol 2. 6th ed. Philadelphia, PA: Mosby Elsevier; 2006:chap 72.
- Snyder CL. Current management of umbilical abnormalities and related anomalies. Semin Pediatr Surg. 2007;16(1):41-49.
- Vane DW, West KW, Grosfeld JL. Vitelline duct anomalies: experience with 217 childhood cases. Arch Surg. 1987;122(5):542-547.
- Moore TC. Omphalomesenteric duct malformations. Semin Pediatr Surg. 1996;5(2):116-123.


