Peer Reviewed
Limited Joint Mobility Syndrome
Jesus (Jesse) D. Bracamonte, DO
Assistant Professor of Family Medicine, Department of Family Medicine, Mayo Clinic Scottsdale, Arizona
Gretchen Anderson, FNP
Department of Family Medicine, Mayo Clinic Scottsdale, Arizona
Molly Kresin, DO
Assistant Professor of Family Medicine, Department of Family Medicine, Mayo Clinic Scottsdale, Arizona
Citation:
Bracamonte JD, Anderson G, Kresin M. Limited joint mobility syndrome. Consultant. 2020;60(3):91-93. doi:10.25270/con.2020.03.00007
A 42-year-old woman presented to our primary care clinic with a 1-year history of progressive hand pain manifested by stiffness, fullness of the digits, tight skin, and an inability to fully flex the digits. Her symptoms affected the small digits of both hands but spared the thumbs.
Her capillary refill was normal, and neurologic examination findings were unremarkable, but she was unable to fully extend the digits of both hands upon examination.
She had a history of poorly controlled diabetes type 1 due to nonadherence, with a hemoglobin A1c level of 13.6%, which correlated with the onset of her symptoms. Her diabetes was being managed with basal insulin via an insulin pump. Her hypertension was adequately controlled with lisinopril and metoprolol, and her cholesterol was well treated with atorvastatin. She continued to smoke a half a pack of cigarettes a day and had done so for 20 years. She had tried acetaminophen without relief. She had no additional history of occupational risks or rheumatologic conditions, and there was no known family history of rheumatologic disease.
She had undergone extensive clinical evaluations by her primary care team and during subsequent specialty consultations with orthopedics, endocrinology, and plastic surgery specialists. Laboratory evaluation and specialty consultation excluded other potential etiologies including complex regional pain syndrome, Dupuytren contracture, flexor tenosynovitis, trigger finger, and other inflammatory conditions. Upon final consultation with a rheumatologist, LJMS was diagnosed based on the pathognomonic positive tabletop and prayer signs (Figures 1 and 2). Ultrasonography revealed fibrous thickening of the flexor tendon sheaths. She was informed that LJMS is a chronic condition, but that optimization of diabetes control and tobacco cessation may help to alleviate her symptoms.
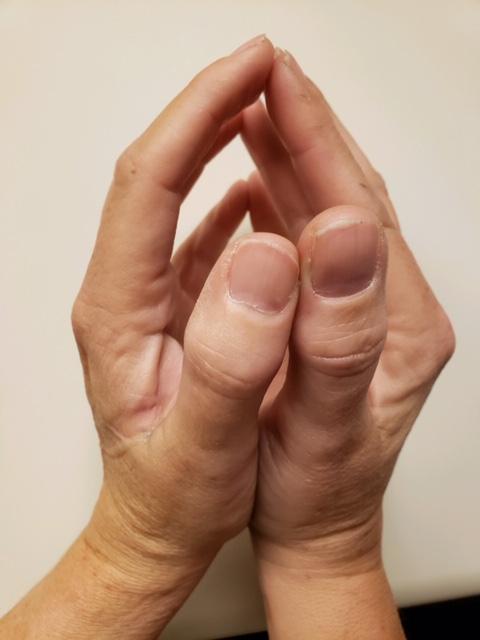
Figure 1. The prayer sign, which tests the patient’s ability to flatten the palmar surfaces together as in the act of prayer; an inability to articulate the palmar surfaces of the digits or hands represents a positive result for LJMS.
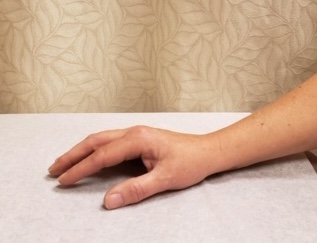
Figure 2. The tabletop test is positive for LJMS when the patient is unable to fully place the palmar aspect of the hand against the surface of a table.
Discussion
Although LJMS does occur in the general population with a prevalence of 6% to 25%, it is highly prevalent in the diabetic population, with rates ranging from 8% to 58%.1-4 Musculoskeletal disorders in general, such as Dupuytren contracture, trigger finger, frozen shoulder, carpal tunnel syndrome, and rotator cuff tendinopathies, are more common in individuals with diabetes. Some reports indicate that LJMS is the most common musculoskeletal disorder manifested in diabetes.5
Common symptoms include stiffness, pain, limited motion, impaired grip strength, waxy skin contractures, and decreased quality of life. In 1957 Lundbæk first described the stiff hands and fingers and associated flexion contractures in patients with diabetes mellitus.6 Formerly known as diabetic cheiroarthropathy or stiff hand syndrome, LJMS is currently considered an irreversible disorder, with case reports documenting improved symptoms with better glycemic control, use of nonsteroidal anti-inflammatory drugs, and physical therapy. It is equally prevalent in men and women. The risk increases with long-term diabetes and in those with higher hemoglobin A1c levels.5
The pathogenesis of LJMS is due to the damaging effects of hyperglycemia on collagen.7-10 Microvascular disease is thought to play a role in tendinopathy, leading to tissue hypoxia and overproduction of free radicals that leads to an apoptotic environment.9,10 The reduced neovascularization in the degenerative tendons leads to decreased levels of endothelial growth factor; fibrous thickening thus ensues. High oxidative stress and the formation of advanced glycation end-products leads to an inflammatory cascade that produces cytokines and growth factors allowing excessive collagen deposition in the tendons.8,9 Over time, such a cascade of effects leads to joint impairment.
Classic signs include the prayer sign (Figure 1) and the tabletop sign (Figure 2), as demonstrated by our patient. The prayer sign tests the patient’s ability to flatten the palmar surfaces together as in the act of prayer; an inability to articulate the palmar surfaces of the digits or hands represents a positive test result for LJMS. A tabletop test is positive for LJMS when the patient is unable to fully place the palmar aspect of the hand against the surface of a table. These signs are pathognomonic for the diagnosis.
Imaging is not required for diagnosis; however, ultrasonography may demonstrate thickening of the flexor tendon sheaths, and magnetic resonance imaging findings also may demonstrate thickening and edema of the flexor tendon sheaths.1,10-13
The clinician must exclude additional pathology that may coexist, such as Dupuytren contracture, carpal tunnel syndrome, and tenosynovitis, all of which can be treated. LJMS involves the 4 digits of the hands, whereas Dupuytren contracture usually involves the fourth and fifth digits, and trigger finger often only affects one digit.
LJMS is a common finding in patients with a long history of diabetes mellitus, particularly in individuals with poorly controlled diabetes. LJMS is a musculoskeletal complication of diabetes mellitus and a harbinger of microvascular disease since the incidence is higher in individuals with LJMS.2 Although there is no cure for LJMS, optimization of diabetes control, tobacco cessation, and physical therapy may help improve the associated symptoms. Medications such as penicillamine and aminoguanidine have not proven useful in investigational trials; the cornerstone of therapy remains optimization of glucose control and mechanisms designed to promote increased mobility.
Increasing awareness of LJMS among clinicians and encouraging them to perform the tabletop and prayer sign tests during diabetic checkups provides another tool to assist with early recognition of associated comorbid microvascular disease.7,8,10
References:
- Gerrits EG, Landman GW, Nijenhuis-Rosien L, Bilo HJ. Limited joint mobility syndrome in diabetes mellitus: a minireview. World J Diabetes. 2015;6(9):1108-1112.
- Chergaoui R, McKenzie S, Nunlee-Bland G. Diabetic cheiroarthropathy: a case report and review of the literature. Case Rep Endocrinol. 2013;2013:257028.
- Douloumpakas I, Pyrpasopoulou A, Triantafyllou A, Sampanis Ch, Aslanidis S. Prevalence of musculoskeletal disorders in patients with type 2 mellitus: a pilot study. Hippokratia. 2007;11(4):216-218.
- Attar SM. Musculoskeletal manifestations in diabetic patients at a tertiary center. Libyan J Med. 2012;7. doi:10.3402/ljm.v7i0.19162.
- Aydeniz A, Gursoy S, Guney E. Which musculoskeletal complications are most frequently seen in type 2 diabetes mellitus? J Int Med Res. 2008;36(3):505-511.
- Lundbæk K. Stiff hands in long-term diabetes. Acta Med Scand. 1957;158(6):447-451.
- Larkin ME, Barnie A, Braffett BH, et al; Diabetes Control and Complications Trial/Epidemiology of Diabetes Interventions and Complications Research Group. Musculoskeletal complications in type 1 diabetes. Diabetes Care. 2014;37(7):1863-1869.
- Abate M, Schiavone C, Salini V, Andia I. Management of limited joint mobility in diabetic patients. Diabetes Metab Syndr Obes. 2013;6:197-207.
- Papanas N, Maltezos E. The diabetic hand: a forgotten complication? J Diabetes Complications. 2010;24(3):154-162.
- Serban AL, Udrea GF. Rheumatic manifestations in diabetic patients. J Med Life. 2012;5(3):252-257.
- Ismail AA, Dasgupta B, Tanqueray AB, Hamblin JJ. Ultrasonographic features of diabetic cheiroarthropathy. Br J Rheumatol. 1996;35(7):676-679.
- Duffin AC, Lam A, Kidd R, Chan AK, Donaghue KC. Ultrasonography of plantar soft tissues thickness in young people with diabetes. Diabetes Med. 2002;19(12):1009-1013.
- Khanna G, Ferguson P. MRI of diabetic cheiroarthropathy. AJR Am J Roentgenol. 2007;18(1):W94-W95.


