Peer Reviewed
Laugier-Hunziker Syndrome
AUTHORS:
Brooke Evans, MPH1 • Richard Byrd, MD1,2
AFFILIATIONS:
1Texas A&M College of Medicine, Houston, Texas
2Kelsey-Seybold Clinic, Houston, Texas
CITATION:
Evans B, Byrd R. Laugier-Hunziker syndrome. Consultant. 2020;60(12):24-26. doi:10.25270/con.2020.06.00009
Received February 13, 2020. Accepted May 11, 2020.
DISCLOSURES:
The authors report no relevant financial relationships.
CORRESPONDENCE:
Richard Byrd, MD, Kelsey-Seybold Clinic, 7010 Hwy 6, Missouri City, TX 77459 (richard.byrd@kelsey-seybold.com)
During a routine wellness examination, an otherwise healthy 12-year-old boy of Indian descent had concerns about dark areas on his tongue. He had first noticed them 1 year ago, and they had gradually increased in number and size.
He denied any associated discomfort, and results of a review of systems were negative for fatigue, weight loss, weakness, abdominal pain, vomiting, rectal bleeding, anemia, drug exposure, bone pain, or precocious puberty. His family history was positive for similar spots on his mother’s tongue (findings of a biopsy had been benign). There was no family history of intestinal polyps or gastrointestinal (GI) tract malignancy. He denied taking any long-term medications.
Physical examination findings were significant for several hyperpigmented macules measuring 1 to 5 mm over the dorsolateral tongue, hyperpigmentation along the maxillary and mandibular gingiva, a 1-cm area of gray-brown pigmentation on the buccal mucosa at the opening of the parotid duct bilaterally, and longitudinal hyperpigmented bands on the nails of both index fingers and the left second toe (Figures 1-6). His lips and genitalia were without altered pigmentation.

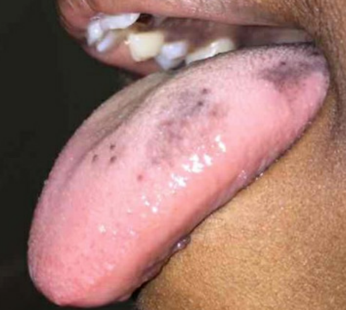
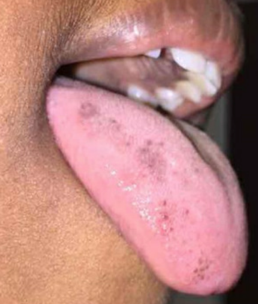
Figures 1-3. Bilateral hyperpigmentation of the patient’s tongue.
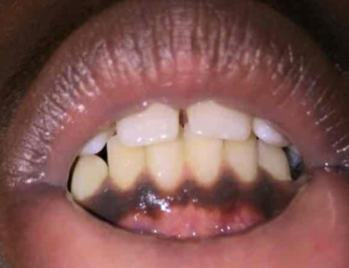
Figure 4. Mandibular gingival hyperpigmentation.
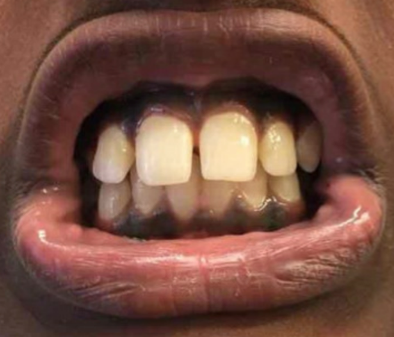
Figure 5. Maxillary and mandibular gingival hyperpigmentation.
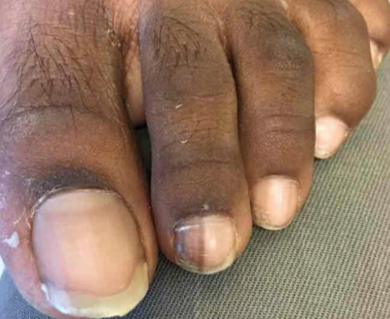
Figure 6. Longitudinal melanonychia on the patient’s left second toe.
Given the patient’s oral and ungual hyperpigmentation with onset at puberty, gradual progression, absence of systemic symptoms, and negative family history of intestinal polyps or GI tract malignancy, a diagnosis of Laugier-Hunziker syndrome (LHS) was made. The patient and his mother were counseled regarding its benign nature.
Discussion. LHS, also known as idiopathic lenticular mucocutaneous pigmentation, is a benign pigmentary disorder without systemic symptoms. It is associated with lenticular or linear hyperpigmented macules that can be isolated or confluent and that can present in various mucocutaneous tissues. It can be either familial or sporadic, with the latter being most common.1,2 The average age of onset is 52 years, and the condition most commonly occurs in white adults.3 A higher incidence in females has been described.4
The most common sites of involvement are the mouth (especially the buccal mucosa) and lips. Less frequent locations include the corners of the mouth, gingivae, tongue, fingers, and plantar aspect of feet.5 Nail lesions are present in about 60% of adult cases, and such findings include pigmented bands of the nail plate (longitudinal melanonychia). This finding, however, is far less common in the pediatric population.6 In the absence of systemic symptoms or specific drug or heavy metal exposure, the presence of both oral and nail pigmentation is highly suggestive of LHS.7
A biopsy of lesions, although not necessary, may help to confirm the diagnosis. Histopathologic findings include increased pigmentation of the basal layer with normal quantity and morphology of melanocytes, epidermal basement membrane pigmentation, and pigment-laden macrophages in the papillary dermis.3,8 Dermoscopic findings are tissue-specific: A parallel banded pattern is found in lesions of the lips and genitalia, and a single homogenous longitudinal band of pigmentation is shown in nail lesions.9
LHS is a clinical diagnosis of exclusion. Other conditions such as Peutz-Jeghers syndrome, Addison disease, subungual melanoma, drug-related hyperpigmentation, heavy metal exposure, and benign racial hyperpigmentation should be considered (Table).3,5,7,10-13

Because of the nonsystemic and benign nature of LHS, no treatment is indicated. However, patients may seek therapies for cosmetic purposes. Treatments using laser therapy and cryotherapy have been used to reduce areas of skin hyperpigmentation.10
Our patient, a 12-year-old boy of Indian descent, represents a patient population that is not well represented in the LHS literature. At a follow-up appointment 4 months later, his pigmentation remained unchanged. The family was again reassured of the syndrome’s benign nature.
REFERENCES:
- Aboobacker S, Gupta G. Laugier-Hunziker syndrome. StatPearls. Updated November 14, 2019. Accessed May 14, 2020. https://www.statpearls.com/kb/viewarticle/24116/
- Makhoul EN, Ayoub NM, Helou JF, Abadjian GA. Familial Laugier-Hunziker syndrome. J Am Acad Dermatol. 2003;49(suppl 2):143‐145. doi:10.1067/mjd.2003.300
- Paul J, Harvey VM, Sbicca JA, O’Neal B. Laugier-Hunziker syndrome. Cutis. 2017;100(3):E17‐E19.
- Yago K, Tanaka Y, Asanami S. Laugier-Hunziker-Baran syndrome. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2008;106(2):e20‐e25. doi:10.1016/j.tripleo.2008.03.037
- Wang W-M, Wang X, Duan N, Jiang H-L, Huang X-F. Laugier–Hunziker syndrome: a report of three cases and literature review. Int J Oral Sci. 2012;4(4):226‐230. doi:10.1038/ijos.2012.60
- Sardana K, Mishra D, Garg V. Laugier-Hunziker syndrome. Indian Pediatr. 2006;43(11):998‐1000.
- Montebugnoli L, Grelli I, Cervellati F, Misciali C, Raone B. Laugier-Hunziker syndrome: an uncommon cause of oral pigmentation and a review of the literature. Int J Dent. 2010;2010:525404. doi:10.1155/2010/525404
- Barman PD, Das A, Mondal AK, Kumar P. Laugier–Hunziker syndrome revisited. Indian J Dermatol. 2016;61(3):338‐339. doi:10.4103/0019-5154.182429
- Gencoglan G, Gerceker-Turk B, Kilinc-Karaarslan I, Akalin T, Ozdemir F. Dermoscopic findings in Laugier-Hunziker syndrome. Arch Dermatol. 2007;143(5):631‐633. doi:10.1001/archderm.143.5.631
- Choi ME, Jung CJ, Lee WJ, et al. A case of recurrent pigmented macules in Laugier-Hunziker syndrome treated using a Q-switched Nd-YAG laser. J Cosmet Laser Ther. 2019;21(7-8):395‐397. doi:10.1080/14764172.2019.1680850
- Burleigh A, Lam JM. Pediatric longitudinal melanonychia. CMAJ. 2017;189(34):E1093. doi:10.1503/cmaj.170256
- Goettmann-Bonvallot S, André J, Belaich S. Longitudinal melanonychia in children: a clinical and histopathologic study of 40 cases. J Am Acad Dermatol. 1999;41(1):17‐22. doi:10.1016/s0190-9622(99)70399-3
- Sreeja C, Ramakrishnan K, Vijayalakshmi D, Devi M, Aesha I, Vijayabanu B. Oral pigmentation: a review. J Pharm Bioallied Sci. 2015;7(suppl 2):S403‐S408. doi:10.4103/0975-7406.163471


