Authors:
Nedyalko N. Ivanov, MS-IV
Ohio University Heritage College of Osteopathic Medicine, Athens, Ohio
Maren Gaul, DO
Western Reserve Hospital, Tri-County Dermatology Residency Program, Cuyahoga Falls, Ohio
Kory Patrick Schrom, MD
University Hospitals Cleveland Medical Center, Cleveland, Ohio
Benjamin M. Witkoff, MS-IV
Ohio University Heritage College of Osteopathic Medicine, Athens, Ohio
Schield Wikas, DO
Tri-County Dermatology Residency Program, Cuyahoga Falls, Ohio
Citation:
Ivanov NN, Gaul M, Schrom KP, Witkoff BM, Wikas S. Fox-Fordyce disease. Consultant. 2019;59(2):59-61.
A well-appearing young woman with an unremarkable medical history presented with a 6-month history of an intensely pruritic eruption affecting the axillae, the areolae, and the genital region. Initially, allergic contact dermatitis had been diagnosed; she had been prescribed a lidocaine/prilocaine cream and clobetasol ointment, which had failed to control the pruritus or the rash.
Physical examination. Discrete, follicular, flesh-colored papules on hyperpigmented thin plaques and patches were noted in the axillae (Figures 1 and 2) and on the periareolar and areolar skin (Figure 3). The patient declined a genital examination.
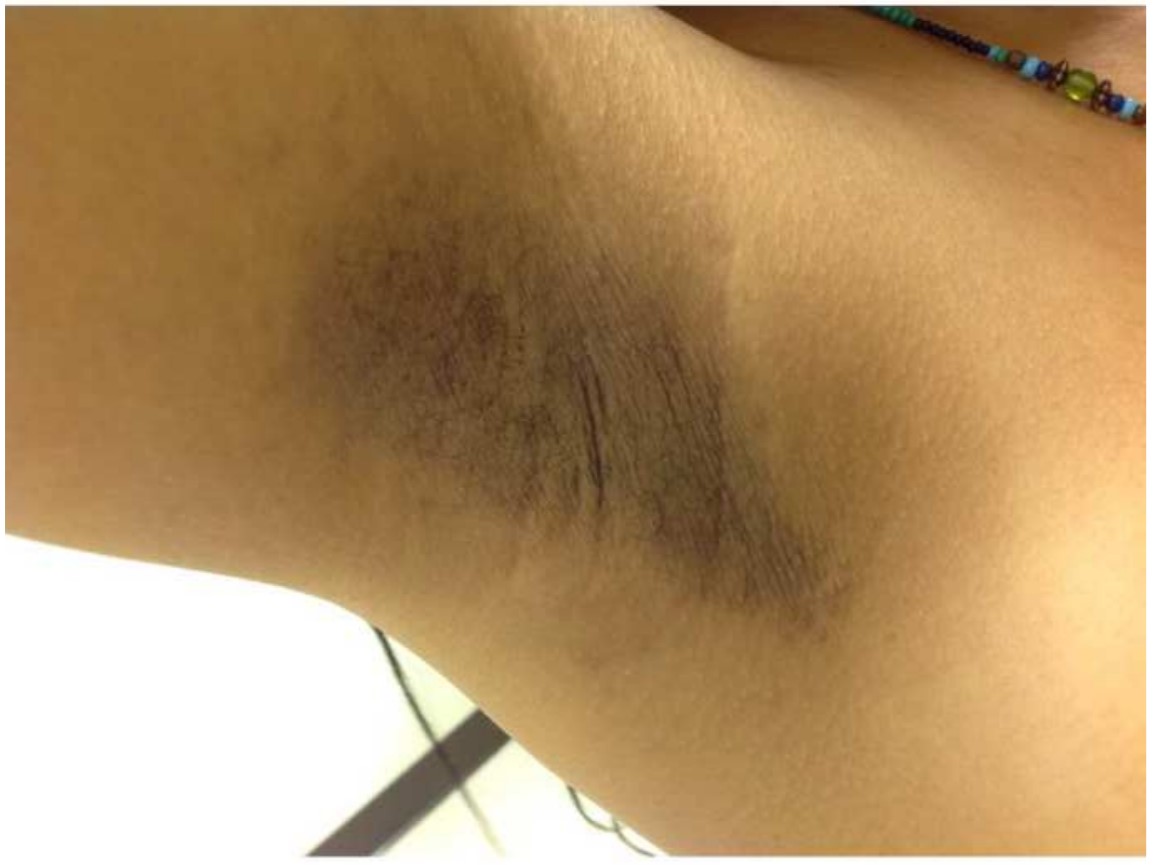
Figure 1. The right axilla with follicular, flesh-colored papules on hyperpigmented thin plaques and patches.
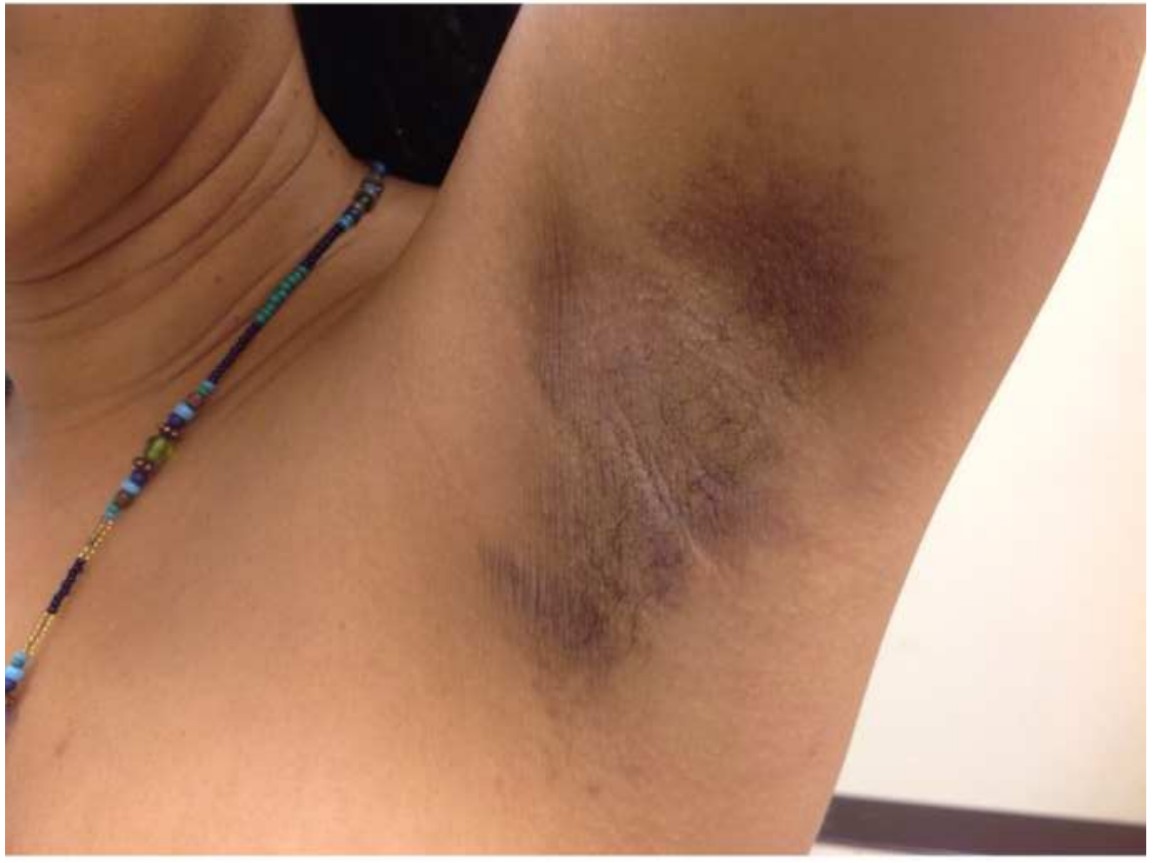
Figure 2. The left axilla with flesh-colored papules on hyperpigmented thin plaques and patches, with accentuated linear markings.
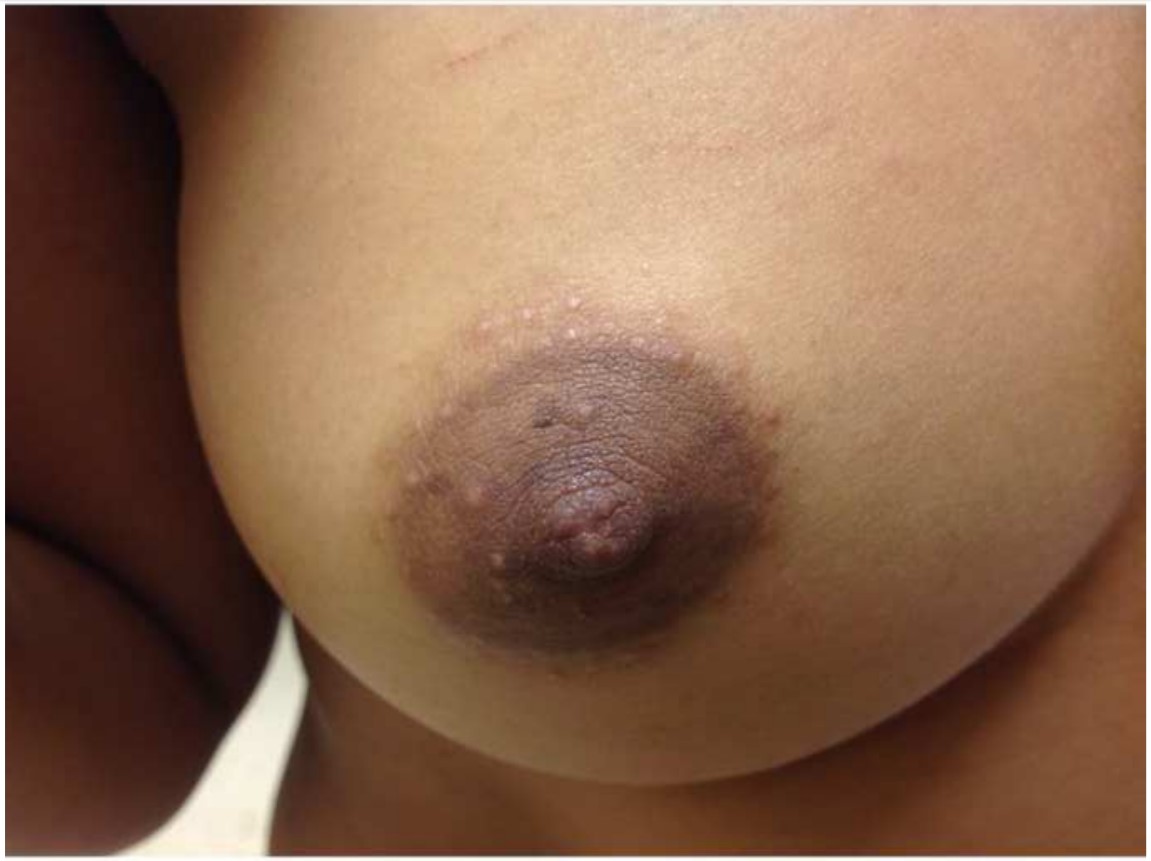
Figure 3. Flesh-colored follicular papules of the periareolar and areolar skin.
Diagnosis. The differential diagnoses included Fox-Fordyce disease (FFD), lichen planopilaris, lichen nitidus, and amyloidosis lichenoides, which can present with flesh-colored papules with pruritus. She received a clinical diagnosis of FFD, given that her presentation was classic for the condition.
Outcome of the case. After being educated about the benign nature of FFD, the patient declined a biopsy and opted to simply start therapy with topical tretinoin gel, 0.08%, along with clobetasol ointment. At her 1-month follow-up visit, there had been no improvement in her symptoms, so she stopped her current therapy and opted to try alternative forms of medicine. She was receptive when we recommended turmeric due to its anti-inflammatory effects. She was subsequently lost to follow-up.
Discussion. Apocrine miliaria, better known as FFD, is an apocrine gland disorder marked by debilitating pruritus that is very challenging to treat. First described by Fox and Fordyce in 1902, FFD primarily affects women aged 13 to 35 years, which implicates an underlying hormonal component. FFD classically presents as discrete, dome-shaped, flesh-colored, follicular papules predominantly affecting axillary, anogenital, and periareolar skin.1,2 The characteristic papules may also occur in the lower presternal region, abdomen, umbilicus, vulva, and the medial upper thigh.1,3-5 Affected areas generally lack normal apocrine sweating and may have decreased hair density.1
The etiology and pathogenesis of FFD remains unknown; however, several case reports have suggested the possibility of familial penetrance. Rare reports exist of patients with FFD without pruritus and FFD onset after laser hair removal.4,6-8 Hormonal mechanisms have also been implicated, given symptomatic improvement with pregnancy and oral contraceptive pills (OCPs) and general remission in postmenopausal women.2 FFD may also be aggravated in the summer months and by emotional stress.1,9
The diagnosis of FFD is based on distinctive clinical and nonspecific histopathological features. Histological features vary but may include infundibulum dilation, hyperkeratosis, keratin plugging of apocrine ducts, acanthosis, lymphohistiocytic infiltrate, perifollicular xanthomatosis, and infundibular spongiosis.4,5,7-13 Brau Javier and colleagues reported perifollicular foam-cell infiltrates as the most distinct pathologic feature of FFD.10 Foam-cell infiltration is thought to be a consequence of infundibular plugging, which leads to apocrine rupture and phagocytosis of excess debris by perifollicular histiocytes.
FFD has no definitive treatment. Although it is an inflammatory disorder, systemic corticosteroids are impractical due to significant systemic adverse effects and rapid disease relapse after cessation. Attempted therapies with variable effectiveness include topical and/or intralesional corticosteroids, topical clindamycin, OCPs, topical tretinoin, oral isotretinoin, UV phototherapy, electrocautery, excision of periareolar skin, topical adapalene gel, topical pimecrolimus, benzoyl peroxide, topical calcineurin inhibitors, antiperspirants, and fractional carbon dioxide lasers.2-9,11,12,14
More novel therapeutic approaches have also been recently described. González-Ramos and colleagues reported complete resolution of pruritus as well as marked reduction in papules after intradermal injections of botulinum toxin type A.8 Another report showed a significant reduction of pruritus after several sessions of pulsed dye laser. While this treatment modality did not show any improvement in papules, it was well tolerated by patients.14 A microwave technology by Miramar Labs Inc has also been reported. This technology targets hair follicles, apo-eccrine, eccrine, and apocrine sweat glands with significant improvement after two treatments. Despite this method being effective at improving the appearance of papules, the procedure is costly, and adverse effects included altered sensation to the skin overlying the treatment area.9
In summary, first-line therapies including topical high-dose corticosteroids and vitamin A derivatives are not consistently effective. OCPs can be considered in affected patients who also wish to avoid pregnancy. However, the eruption would be expected to recur with cessation. Varying results in treatment have been reported, warranting further research to explore alternative treatments. Novel approaches such as intradermal injections of botulinum toxin type A, application of pulsed dye laser, and microwave technology have potential in the treatment of FFD, but these methods need to be studied in larger populations to ensure efficacy. This may be rather impractical, however, due to the rarity of FFD.
References:
- Shelley WB, Levy EJ. Apocrine sweat retention in man. II. Fox-Fordyce disease (apocrine miliaria). AMA Arch Derm. 1956;73(1):38-49.
- Miller JL. Diseases of the eccrine and apocrine sweat glands. In: Bolognia JL, Jorizzo JL, Schaffer JV, eds. Dermatology. Vol 1. 3rd ed. Philadelphia, PA: Elsevier Saunders; 2012:587-60
- Ballester I, López-Ávila A, Ortiz S. Fox-Fordyce disease with an atypical clinical presentation. Actas Dermosifiliogr. 2013;104(9):832-834.
- Helou J, Maatouk I, Moutran R, Obeid G. Fox-Fordyce-like disease following laser hair removal appearing on all treated areas. Lasers Med Sci. 2013;28(4):1205-1207.
- Gurusamy L, Jegadeesan M, Jayakumar S. Fox-Fordyce disease of the vulva. Indian J Sex Transm Dis. 2016;37(1):65-67.
- James WD, Berger TG, Elston DM. Diseases of the skin appendages In: James WD, Berger TG, Elston DM. Andrews’ Diseases of the Skin: Clinical Dermatology. 12th ed. Philadelphia, PA: Elsevier; 201
- Alés-Fernández M, Ortega-Martínez de Victoria L, García-Fernández de Villalta MJ. Lesions in the axilla after hair removal using intense pulsed light. Actas Dermosifiliogr. 2015;106(1):61-62.
- González-Ramos J, Alonso-Pacheco ML, Goiburú-Chenú B, Mayor-Ibarguren A, Herranz-Pinto P. Successful treatment of refractory pruritic Fox-Fordyce disease with botulinum toxin type A. Br J Dermatol. 2016;174(2):458-459.
- Taylor D, Au J, Boen M, Fox S, Aronson IK, Jacob C. A novel modality using microwave technology for the treatment of Fox-Fordyce disease (FFD). JAAD Case Rep. 2016;2(1):1-3.
- Brau Javier CN, Morales A, Sanchez JL. Histopathology attributes of Fox-Fordyce disease. Int J Dermatol. 2012;51(11):1313-1318.
- Kassuga LEdBP, Medrado MM, Chevrand NS, Salles SdAN, Vilar EG. Fox-Fordyce disease: response to adapalene 0.1%. An Bras Dermatol. 2012;87(2):329-331.
- Blasco-Morente G, Naranjo-Díaz MJ, Pérez-López I, Martínez-López A, Ruiz-Villaverde R, Aneiros-Fernández J. Fox-Fordyce disease. Sultan Qaboos Univ Med J. 2016;16(1):e119-120.
- Liu WC, Cao T, Ho MSL, Chong W-S, Lee JSS. In vivo features of Fox-Fordyce disease in high-definition optical coherence tomography. J Dtsch Dermatol Ges. 2016;14(1):62-63.
- Uzuncakmak TK, Karadag AS, Ozlu E, Akdeniz N, Cobanoglu Simsek B. Effective treatment of Fox-Fordyce disease with pulsed dye laser. Photodermatol Photoimmunol Photomed. 2016;32(5-6):311-313.


