Peer Reviewed
Is This a Puss Caterpillar Sting or Something Else? How a Common Medical Error Can Delay a Diagnosis
AUTHOR:
Nathan F. Bradford, MD
AFFILIATION:
Medical University of South Carolina/AnMed Health Clinical Campus, AnMed Health Oglesby Center, Greenville, South Carolina
CITATION:
Bradford NF. Is this a puss caterpillar sting or something else? How a common medical error can delay a diagnosis. Consultant. 2020;60(6):e2. doi:10.25270/con.2020.03.00011
Received October 16, 2019. Accepted February 25, 2020.
DISCLOSURE:
The author reports no relevant financial relationships.
CORRESPONDENCE:
Nathan F. Bradford, MD, AnMed Health Oglesby Center, 2000 East Greenville St, Ste 5115, Anderson, SC 29621 (nathan.bradford@anmedhealth.org)
Sometimes a patient’s self-diagnosis can be helpful—one should always keep in mind the maxim “Stop talking! The patient is trying to tell you what is wrong with her!” On the other hand, a patient also can lead the diagnostician astray. The 3 A’s—attribution, availability, and anchoring—come into play here. The power of suggestion can cause the clinician to anchor on one part of the history or physical examination, a common heuristic error. Furthermore, friendship with a patient, while enriching to the patient–physician relationship, often can lead to attribution error—for example, “Bill’s wife calls me about every little problem he has!”
That is what occurred in this case. The patient, an 83-year-old man with multiple myeloma, was not only a patient but also a family friend, along with his wife of more than 50 years. Due to her husband’s medical problems, she had learned to be his outspoken advocate. Two years prior, he had stepped on a puss caterpillar while mowing his grass, causing blisters on his foot and making a strong impression on his wife. So when she called the office and told the nurse that he had developed another rash from a puss caterpillar, we were tempted to discount the complaint. Instead, knowing the man to be immunocompromised, the receptionist scheduled an appointment.
The puss caterpillar is the larval form of the southern flannel moth (Megalopyge opercularis) and is native to the southeastern and southern United States. Its hair-like spines grow long during the summer months, resembling a fluffy cat (Figure 1). When touched, the caterpillar stings the skin with its venomous hairs as opposed to biting with its mouth, causing an extremely painful vesicular rash. The treatment is usually observation and palliative measures, and the lesions eventually resolve.

Upon presentation, the patient stated that he had mown the grass several days before the rash had developed, just as before. However, he did not remember seeing any puss caterpillars this time. Although he had had no fever, he reported that the lesions on his arm and hand were more painful than the foot lesions had been last time. On physical examination, he was afebrile with normal vital signs and no adenopathy. His left forearm and hand showed vesicles and erythema, mostly on the extensor surfaces. The lesions were slightly tender to the touch. The provider in the office that day agreed with the wife’s assessment that this was a puss caterpillar sting and prescribed a topical corticosteroid cream.
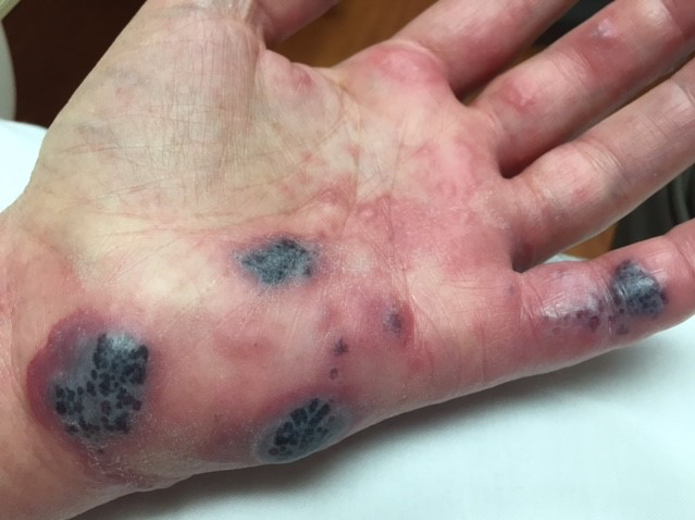
Over the next few days, the rash worsened and became more painful. The patient returned to the office for a recheck. On examination, he now had tender, necrotic plaques on the left hand and forearm (Figures 2-4).


The patient’s medical history included multiple myeloma, for which he had been taking lenalidomide for 2 years with good results. He also had a history of coronary artery disease, narcolepsy, and hypertension.
After considering a wide differential diagnosis for the rash, including insect bites and stings, herpes zoster, bullous impetigo, dermatitis herpetiformis, pemphigus vulgaris, and other autoimmune blistering diseases, he received a clinical diagnosis of herpes zoster. Because of the patient’s immunocompromised state, he was admitted to the hospital and was started on intravenous acyclovir, 10 mg/kg every 8 hours. A dermatopathologist biopsied the lesions, and the results of pathology tests were consistent with herpes zoster.
Over the next few days, the patient’s pain and rash slowly improved. He developed no worsening symptoms such as fever, headache, or cough. He was discharged to complete a 7-day course of acyclovir. Since that episode 3 years ago, he has had persistent postherpetic neuralgia (PHN) but has had no further lesions.
In retrospect, the question arises as to whether earlier diagnosis and treatment may have prevented this patient’s PHN.1,2 Study findings have been inconsistent about whether antiviral therapy decreases the incidence of PHN.3 Early treatment may indeed shorten the duration of PHN. There is some evidence that the addition of systemic corticosteroids can also decrease the incidence of PHN.4 Our patient was not a candidate for systemic corticosteroids because of his immunocompromised state. Of note, the patient had not received the shingles vaccine prior to this episode. There is a lower incidence of PHN following the outbreak of zoster in vaccinated individuals.5
One should always heed Osler’s maxim, “Listen to the patient.” In fact, with unexplained signs and symptoms, it is often helpful to ask the patient what he or she believes to be the problem. However, one must balance that information, knowing that it is tempting to anchor on a piece of patient history. In addition, one must always try to separate the condition from the patient's psychosocial background: The boy who cried “Wolf!” eventually had a life-threatening emergency.
In summary, this patient’s diagnosis of herpes zoster was delayed by a week due to common heuristic errors—attribution error and anchoring. Being more aware of common errors while listening to the patient can avoid complications and morbidity.
REFERENCES:
- Gnann JW Jr, Whitley RJ. Herpes zoster. N Engl J Med. 2002;347(5):340-346. doi:10.1056/NEJMcp013211
- Gabutti G, Valente N, Sulcaj N, Stefanati A. Evaluation of efficacy and effectiveness of live attenuated zoster vaccine. J Prev Med Hyg. 2014;55(4):130-136.
- Alper BS, Lewis PR. Does treatment of acute herpes zoster prevent or shorten postherpetic neuralgia? J Fam Pract. 2000;49(3):255-264.
- Wareham DW, Breuer J. Herpes zoster. BMJ. 2007;334(7605):1211-1215. doi:10.1136/bmj.39206.571042.AE
- Oxman MN, Levin MJ, Johnson GR, et al; Shingles Prevention Study Group. A vaccine to prevent herpes zoster and postherpetic neuralgia in older adults. N Engl J Med. 2005;352(22):2271-2284. doi:10.1056/NEJMoa051016


