Abdominal Pain: A Rational Approach, Part 1
Because abdominal pain is such a common chief complaint, arriving at an exact diagnosis is often challenging. The dangerous triad of vascular emergencies (mesenteric ischemia, abdominal aortic aneurysm [AAA], and myocardial infarction) can cause abdominal pain of a severity that is out of proportion to the tenderness observed on physical examination. The only methods to “rule out” mesenteric ischemia are specific vessel contrast-enhanced studies (magnetic resonance angiography, multi-row detector computer tomographic angiography, or traditional angiography) and surgery; however, traditional CT often will provide important alternative diagnoses. Bedside ultrasonography and CT are the tests of choice when AAA is included in the differential of a patient with abdominal pain. The most important laboratory test in a woman of childbearing age with pelvic pain is urine qualitative beta-hCG measurement.
Key words: abdominal pain, mesenteric ischemia, abdominal aortic aneurysm, ectopic pregnancy
Most cases of abdominal pain do not result from a life-threatening condition. When they do, they may not differ obviously from cases in which the cause of pain is benign.
As many as half of patients who are evaluated for abdominal pain do not receive a precise diagnosis. And for about half of those who are given a diagnosis, the diagnosis is wrong.1,2 Misdiagnosis can divert attention from a serious disorder or lead to ill effects of unnecessary treatment.
In this two-part series, we will use actual cases (not “textbook” examples) to illustrate an approach to abdominal pain that begins with a careful differential diagnosis. We also offer some general guidelines for evaluating patients (Box).
Here, in Part 1, we present cases of mesenteric ischemia, abdominal aortic aneurysm (AAA), and ectopic pregnancy. In Part 2, in a coming issue, we will discuss ovarian torsion, intussusception, and appendicitis during pregnancy.

CASE 1:
OLDER WOMAN WITH EPIGASTRIC PAIN
Initial evaluation. An 86-year-old woman presented to the emergency department (ED) with epigastric pain of sudden onset, which awoke her from sleep; she reported that it felt as if something had “burst” in her abdomen. The pain was accompanied by nausea and diarrhea but without vomiting, dyspnea, or dysuria. She rated the severity of the pain at 9 on a scale of 1 to 10.
Her past medical history was significant for coronary artery disease, hypertension, an appendectomy, and diverticular disease. Medications included digoxin, furosemide, nisoldipine, alendronate, and diazepam at night. She lived with her daughter and was independent in all of her basic and instrumental activities of daily living.
The patient was a thin woman who was anxious and in moderate pain. Blood pressure was 150/90 mm Hg; heart rate, 71 beats per minute; respiration rate, 24 breaths per minute; oxygen saturation, 95% on room air; and temperature, 36.0°C (96.8°F). Her abdomen was soft, with hypoactive bowel sounds and mild epigastric tenderness. She had no rebound, guarding, or rigidity, and she had a palpable aorta of normal diameter. The results of her rectal examination were normal, and a stool guaiac test was negative for occult blood. Her extremities and pulses were normal.
Differential diagnosis of pain out of proportion to examination findings. The dangerous triad of vascular emergencies (AAA, mesenteric ischemia, and myocardial infarction [MI]) can cause abdominal pain of a severity that is out of proportion to the tenderness observed on physical examination. In this case, the patient’s past medical history, medications, and age suggested a broader differential that also included the following:
•Biliary tract obstruction.
•Bowel obstruction.
•Digoxin toxicity.
•Pancreatitis.
•Pyelonephritis.
•Perforated diverticula.
•Perforated duodenal/peptic ulcer.
An abdominal radiograph revealed no evidence of an acute process. An ECG showed a right bundle branch block with left ventricular hypertrophy, which was unchanged from a previous ECG. Laboratory studies revealed a white blood cell (WBC) count of 17,500/µL, a hematocrit of 40%, a total bilirubin level of 0.8 mg/dL, a digoxin level of 0.5 ng/mL, a troponin level of less than 0.5 µg/L, and normal electrolyte levels. Urinalysis showed 4 red blood cells (RBCs) per high-power (hpf) and 18 WBCs per hpf.
The next steps. Can the patient be discharged with the diagnosis of a urinary tract infection (UTI)? Can physical examination rule out a ruptured AAA or mesenteric ischemia? The treating physicians were worried about the 3 vascular abdominal emergencies in the elderly and took steps to exclude those diagnoses. Indeed, elderly patients with abdominal pain are more likely to have a serious illness than younger patients. Approximately 60% of elderly patients who present to the ED with abdominal pain will be admitted, 20% will require surgical or invasive procedures, and 5% will die.3 Furthermore, among those older than 80 years, if an incorrect diagnosis is made at the time of admission, mortality almost doubles.4
Given this patient’s unchanged ECG and stable vital signs, an emergent abdominal CT scan was ordered along with immediate surgical consultation for possible mesenteric ischemia. An initial CT scan performed with intravenous (IV) contrast only showed a normal aorta and possible sigmoid thickening. A second CT scan with oral contrast showed “thickening of a long segment of the distal ileum without fat stranding or fluid.” These findings are consistent with mesenteric ischemia.
Acute mesenteric ischemia. This is caused by insufficient intestinal blood flow from occlusive or non-occlusive pathology of the arteries or venous occlusion. Arterial occlusion is commonly caused by an embolus or thrombosis, while non-occlusive ischemia occurs as a result of processes such as vasospasm or low cardiac output. Venous occlusion is commonly caused by thrombosis. Acute mesenteric ischemia frequently involves the superior mesenteric artery circulation or venous outflow.
Acute arterial occlusive mesenteric ischemia occurs almost exclusively in patients with atherosclerotic disease. Emboli can originate from dislodged atheromatous plaques, secondary to aortic instrumentation, or from cardiac emboli, including from post–MI mural thrombus, valvular disease, and atrial fibrillation. Thrombosis is often caused by atherosclerotic vascular disease, aortic aneurysm, or aortic dissection. Non-occlusive mesenteric ischemia also regularly occurs in patients with significant atherosclerotic disease and is often caused by low-output states (congestive heart failure [CHF], MI, sepsis) or vasospastic drugs. Venous occlusion is caused by a hypercoaguable state, malignancy causing compression of the vessels, portal hypertension, or venous injury from recent surgery or trauma. Embolism accounts for approximately 50% of cases, thrombosis for 25%, non-occlusive causes for 20%, and venous thrombus for 5%.5
Acute arterial mesenteric ischemia classically presents as the rapid onset of severe periumbilical pain, possibly with nausea, vomiting, and diarrhea. The hallmark of acute mesenteric ischemia is pain out of proportion to examination findings. Only 25% of patients have a positive stool guaiac test for occult blood. If ischemia progresses untreated, the patient will develop tenderness, peritoneal signs, and shock. Caution must be used, however, as clinical presentation varies slightly by type, such as a more insidious course with venous thrombosis.
No laboratory test is sensitive enough to rule out the diagnosis reliably, because the results may be entirely normal early in the course of the disease; most are only abnormal once bowel necrosis has begun.6 Abnormalities may include an elevated WBC count, metabolic acidosis, and an elevated lactate level. Elevated serum lactate has been shown to be between 77% and 100% sensitive, but only 42% specific.7,8 It would be prudent to consider mesenteric ischemia in any patient who has acute abdominal pain with metabolic and lactic acidosis.
Patients with suspected mesenteric ischemia are often evaluated with radiographic studies. Plain radiographs are usually normal or nonspecific. Positive findings are frequently seen late and include intramural air (pneumatosis intestinalis), thickened bowel wall with “thumbprinting,” and portal venous gas.
Ultrasound can be used to detect occlusion in the celiac or superior mesenteric artery, but it cannot detect more distal clots. It also cannot be used to diagnose non-occlusive disease. Ultrasound is limited by the presence of distended loops of bowel.9
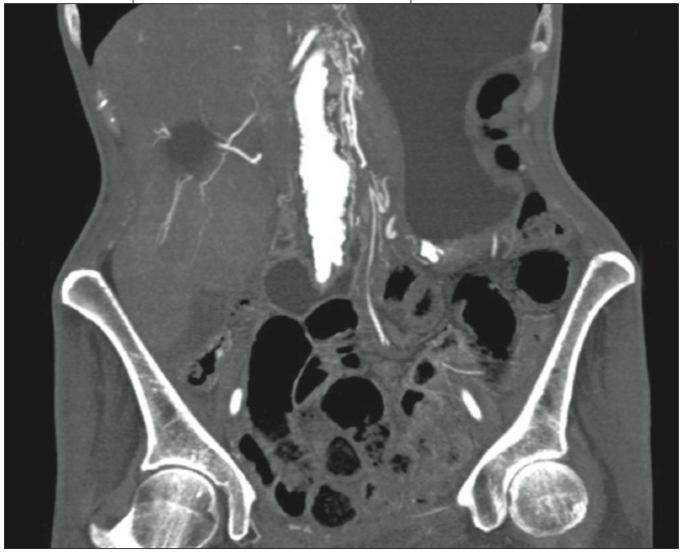
Figure 1 – This CT scan demonstrates two of the findings of mesenteric isch- emia: intramural air (pneumatosis intestinalis) and thrombus in the superior mesenteric artery.
CT findings are often normal or nonspecific. However, CT can help evaluate other causes of abdominal pain. Specific findings include pneumatosis intestinalis, portal venous gas, abnormal bowel enhancement, and mesenteric vessel occlusion (Figure 1). The most common finding is bowel wall thickening or edema. The sensitivity is between 64% and 87% for identifying mesenteric ischemia on CT.10
Magnetic resonance angiography (MRA) and multi-row detector computer tomographic angiography (CTA) are both highly sensitive in detecting mesenteric ischemia. However, given its speed, cost, and availability, CTA is the desired modality.9 A study by Ofer and associates11 in 2009 demonstrated an overall sensitivity of 89%, a specificity of 97%, and an accuracy of 96% for 16-slice CTA in diagnosing mesenteric ischemia. A more recent study by Barmase and colleagues12 in 2011 showed a 100% sensitivity and specificity in detecting acute mesenteric ischemia in 16 patients by multi-row detector CTA.
Angiography traditionally has been the gold standard for diagnosis of mesenteric ischemia. However, its use has gone out of favor with the advancement of CT scanners. It is likely only useful for stable patients without peritoneal signs, when mesenteric ischemia is strongly suspected and the patient has a normal or equivocal CTA scan. It is important to remember that patients with an acute surgical abdomen and a high clinical suspicion for mesenteric ischemia should go directly to surgery.
Once the suspected diagnosis of acute mesenteric ischemia is made, an aggressive approach is warranted because small delays in treatment significantly increase mortality. The mortality ranges from 59% to 93%, with higher mortality associated with bowel wall infarction. However, mortality can be reduced with rapid treatment.5 Unfortunately, despite advancements in diagnostic and treatment modalities, the mortality rate is still as high as it was decades ago. This is likely due in part to the advanced presentation, advanced age, and diagnostic difficulties present in the assessment of elderly patents.13 Treatment includes aggressive fluid resuscitation and hemodynamic monitoring. Patients should receive broad-spectrum antibiotics.
For acute embolic mesenteric ischemia, surgical resection of ischemic bowel and/or embolectomy of involved vessel have been the standard of care.9 Other therapies involve intra-arterial infusions of papaverine or thrombolytics coupled with laparoscopy in patients without peritonitis.14 Thrombotic disease is treated using surgical revascularization and removal of gangrenous bowel. Venous thrombosis is treated with anticoagulation and removal of gangrenous bowel. Finally, non-occlusive disease is treated with reversal of the low-flow state and/or papaverine infusion.9
Hospital course. Although the CT scan was consistent with mesenteric ischemia, the patient’s pain diminished and the surgical service declined to admit her. She was admitted to the geriatric service with the diagnosis of possible diverticulitis versus alendronate-induced esophagitis versus mesenteric ischemia.
On hospital day 3, the patient’s condition acutely worsened, and peritoneal signs developed. She was taken to the operating room, where 57 cm of ischemic ileum and 6.5 cm of ischemic cecum were removed with primary anastomosis of the remainder. Despite the traditionally high mortality for such a clinical scenario, the patient did well and was discharged 8 days later.
LESSONS FROM THIS CASE
•Suspect mesenteric ischemia in all elderly persons who have severe abdominal pain without significant tenderness.
•Do not be dissuaded from a proper diagnostic evaluation by the seeming presence of a UTI in an elderly patient.
•The only methods to “rule out” mesenteric ischemia are specific vessel contrast-enhanced studies (MRA, CTA, or angiography) and surgery, but traditional CT often will provide important alternative diagnoses.
CASE 2:
OLDER MAN WITH GROSS HEMATURIA
Initial evaluation. An obese 69-year-old man presented to the hospital with left lower quadrant pain of sudden onset and gross hematuria. The patient’s pain was moderate, but he displayed significant diaphoresis.
Blood pressure was 161/95 mm Hg; heart rate, 61 beats per minute; respiration rate, 17 breaths per minute; and temperature, 36.4°C (97.5°F). His abdomen was soft, with normoactive bowel sounds and moderate left lower quadrant tenderness. He displayed no costovertebral angle tenderness.
A chest film revealed cardiomegaly and mild CHF. Urinalysis showed 3 WBCs per hpf and and 10 RBCs per hpf.
Differential diagnosis of severe pain with slight tenderness. The dangerous triad of vascular emergencies (AAA, mesenteric ischemia, and MI) can cause abdominal pain of a severity that is out of proportion to the tenderness observed on physical examination. So, too, can the other conditions included in this differential diagnosis:
•Aortic dissection.
•Biliary tract disease (in elderly patients).
•Nephrolithiasis.
•Peptic ulcer with perforation (in elderly patients).
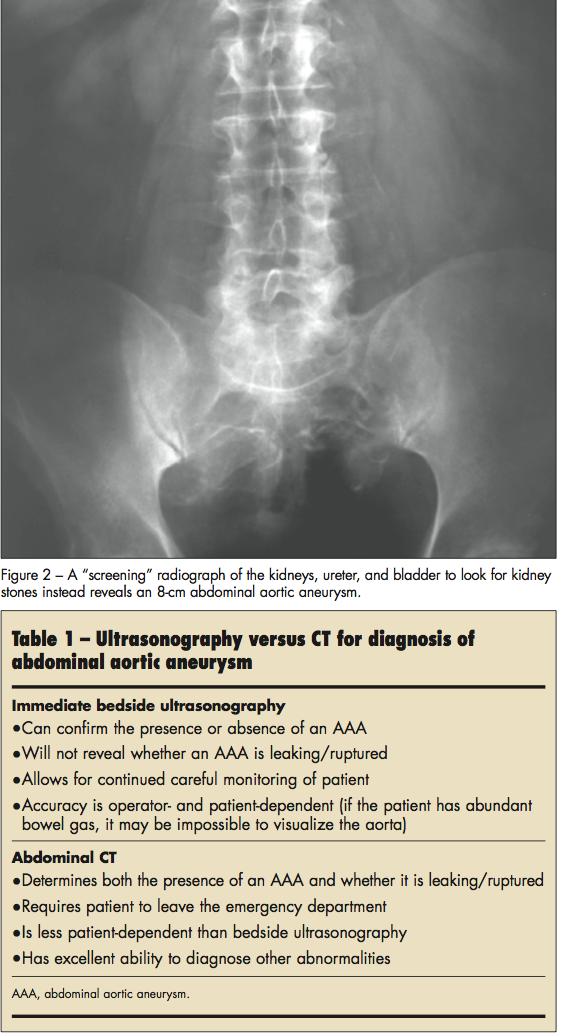
The next steps. The ECG showed sinus rhythm and no signs of myocardial ischemia. Because the differential diagnosis includes nephrolithiasis, physicians at this point may obtain a screening radiograph of the kidneys, ureter, and bladder (KUB) to look for kidney stones. This patient’s KUB is shown in Figure 2.
An abdominal series should consist of 3 views, including flat, upright, and upright chest films. Although often used as a screening tool when the differential diagnosis includes nephrolithiasis, a KUB to look for kidney stones is no longer recommended.15 More recent literature suggests the usefulness of a KUB in the ED is limited to the identification of small bowel obstruction in the setting of acute abdominal pain, suspicion of esophageal foreign body, or suspected sharp foreign body.16 The identification of perforation and volvulus may also be possible.17 Plain radiography is not a good screening tool for nephrolithiasis because the sensitivity is only 45% to 64%.15,16,18 In patients with acute, diffuse, nonspecific abdominal pain, the KUB lacks utility as 98% of these studies will be normal or have a positive finding unrelated to the acute condition.19 Furthermore, clinicians must carefully interpret films that will have a delayed reading by a radiologist.
This patient had an AAA, which can have a subtle appearance on an abdominal x-ray film. In patients with an AAA, abdominal radiographs may show a calcified outline of the aorta and lateral displacement of the calcified wall, which suggests the presence of the aneurysm. A sign of leakage or rupture of an AAA is the obliteration of the ipsilateral iliopsoas margin. In a patient with appropriate symptoms, the sensitivity of abdominal radiography for AAA is only 60% to 70%. Therefore, plain films should not be the initial diagnostic study when an AAA is suspected. Instead, ultrasonography or CT should be used (Table 1).
Abdominal aortic aneurysm. This is a localized dilatation of all layers of the aortic wall. Although the cause of AAA is unknown, the condition is associated with long-standing hypertension and atherosclerosis. AAAs are present in about 6% of men aged 55 to 64 years and 14% of those aged 65 to 74 years. They are 4 to 6 times more common in men than in women.20
Most AAAs are asymptomatic unless they rupture or leak. With rupture, patients may present with abdominal or back pain and hypotension. The physical examination may be misleading because patients often lack significant tenderness and a pulsatile mass.
Radiologic studies establish the diagnosis in most cases. Plain lateral lumbar spine radiographs reveal evidence suggestive of AAA in 60% of cases. However, they should never be used to rule out AAA and are, therefore, of little use in the evaluation of a patient in whom an AAA is suspected.
Under ideal conditions, the sensitivity and specificity of ultrasonography for detecting an AAA approaches 100%.21 Ultrasonography also has the advantage of being able to be done at the bedside of an otherwise unstable patient, and it is the imaging modality of choice in these circumstances. A literature review showed that in patients suspected of having an AAA, ED bedside ultrasound scanning is both sensitive and specific for detecting an AAA and may improve patient care.22 Furthermore, the bedside ultrasound scan done by trained emergency medicine residents has been shown to be 94% sensitive at detecting an AAA.23
However, when faced with an unstable patient who has compelling clinical evidence of an AAA, seek immediate laparotomy. Limitations of ultrasound include difficulty in identifying rupture or leakage. Also, in non-fasting patients, large portions of the abdominal aorta (at least one third of its length) may not be visualized on bedside emergency ultrasonography.24

Figure 3 – A sagit- tal image of a contrast-enhanced CT scan shows a large leaking abdominal aortic aneurysm.
CT is the diagnostic test of choice for patients in stable condition in whom a ruptured AAA is suspected (Figure 3). The sensitivity of CT for detecting AAA is nearly 100%, and it has the advantage of being able to detect other potential causes of abdominal pain and hypotension, and to determine whether an endovascular repair is feasible.
IV contrast is not needed for the diagnosis of a ruptured AAA. However, a contrast-enhanced CTA is the best diagnostic and pre-intervention planning study because it accurately delineates the location, size, and extent of the aneurysm and the involvement of branch vessels, allowing for accurate quantitative 3D measurements.25
Angiography is less sensitive and more invasive than other imaging tests. Historically, its main use has been the evaluation of patients before elective AAA repair; it has no role in the emergent evaluation of a patient with a suspected leaking AAA. Likewise, MRI is an accurate method of identifying AAA, but it is time consuming and often not available, and therefore also plays little role in the ED.26
Treatment of a leaking AAA involves immediate surgical consultation and fluid and blood transfusions to maintain adequate organ perfusion. In previous decades, the mortality associated with emergent repair of a ruptured AAA was 50%, but a more recent study suggests that it may be as low as 41%.27 The mortality is higher when hemorrhage occurs in the abdominal cavity as opposed to the retroperitoneal space.28 One study found that emergency surgery in patients older than 80 years prolonged life, on average, by only 1 week.29
Newer treatments involve endovascular grafts placed via the femoral artery under fluoroscopic guidance. Currently, most centers use these grafts for elective AAA repair in patients who are poor candidates for surgery, but a few institutions have the capability to place them emergently.30 A randomized trial that compared endovascular aneurysm repair and open repair for rupture did not find a significant difference in mortality.31 However, there is accumulating evidence that endovascular repair may lead to improved survival following a ruptured AAA. A review of the American College of Surgeons National Surgical Quality Improvement Program database revealed a lower mortality for patients undergoing endovascular repair versus open repair for a ruptured AAA.32
Hospital course. The treating physician received the radiologist’s report identifying the AAA 5 hours after the patient arrived, and immediate surgical consultation was obtained. As the patient was prepared for surgery, he complained of increased abdominal and back pain. He was given analgesics but continued to have pain and became hemodynamically unstable. All resuscitative efforts failed, including blood transfusion and emergency thoracotomy, and the patient died less than 2 hours after the diagnosis was made.
LESSONS FROM THIS CASE
•Always consider AAA first in those patients with vasculopathy who have signs and symptoms of nephrolithiasis.
•Screening KUBs lack sensitivity for serious abdominal pathology; an abdominal series also lacks sensitivity and should be reserved for suspected perforation, obstruction, or foreign body.
•Bedside ultrasonography and CT are the tests of choice when AAA is included in the differential of a patient with abdominal pain.
CASE 3:
YOUNG WOMAN WITH LOWER ABDOMINAL PAIN
Initial evaluation. A 32-year-old woman presented to her primary care physician (who is also a good friend) with a 3-week history of intermittent lower abdominal pain. The pain began in the right lower quadrant but had become diffuse and was increasing in frequency and severity. She denied nausea, vomiting, diarrhea, and any genitourinary symptoms; she felt that the pain was gastrointestinal and she experienced increasing “bowel pressure.” She reported that the pain made it increasingly difficult to get through her workday.
At the time of examination she had no pain. Her past medical history was significant only for being gravida 2, para 1 (1 normal spontaneous vaginal delivery at term and 1 spontaneous abortion). She was trying to conceive. Her last normal menstrual period had occurred 2 weeks earlier.
Blood pressure was 106/84 mm Hg; heart rate, 85 beats per minute; respiration rate, 18 breaths per minute; oxygen saturation, 100% on room air; and temperature, 37.2°C (99°F). Results of the heart and lung examination were normal. Her abdomen was soft and diffusely tender with moderate guarding in the right lower quadrant without any rebound. She had no costovertebral tenderness.
Differential diagnosis of lower abdominal pain in a young woman. Diseases specific to the female patient must be assessed, including ectopic pregnancy and ovarian torsion, because they can lead to significant morbidity and mortality if undiagnosed. The following other conditions must also be included in this differential diagnosis:
•Appendicitis.
•Hemorrhagic ovarian cyst.
•Nephrolithiasis.
•Pregnancy.
•Threatened abortion.
•Tubo-ovarian abscess.
Given the differential diagnosis, are there any critical elements of the physical examination missing? A review of the medical records revealed that no pregnancy test was done and no pelvic or rectal examination was performed. The patient did have a urinalysis done that showed no abnormalities, and her hematocrit was 40.6%.
The patient was told that the problem was probably not urgent, but she was advised not to take any analgesics until the cause of her pain was identified. She was also told to schedule a pelvic ultrasound scan in at least a week to allow time for insurance authorization.
An elective pelvic ultrasound scan performed 8 days later showed an 8.3-cm heterogeneous, hypoechoic mass within the right adnexa and a small amount of fluid within the cul-de-sac. In conjunction with a positive urine pregnancy test and a serum beta–human chorionic gonadotropin (beta-hCG) level of 676 mIU/mL, these findings were indicative of an ectopic pregnancy.
Ectopic pregnancy. Implantation of a fertilized ovum outside the endometrial cavity defines this condition. This potential life-threatening implantation occurs in approximately 1.5% to 2.0% of pregnancies and remains the most common cause of non-traumatic maternal death in the first trimester.33 It accounts for 6% of pregnancy-related deaths in the United States overall.34
Risk factors include pelvic inflammatory disease, previous tubal surgery, prior ectopic pregnancy, infertility, diethylstilbestrol (DES) exposure, smoking, age over 35 years, intrauterine device use, and many lifetime sex partners.33,35,36 Nevertheless, almost half of all cases of ectopic pregnancy occur in women without risk factors.37
The presence of both an ectopic pregnancy and an intrauterine pregnancy is known as a heterotopic pregnancy. In women undergoing in vitro fertilization, the risk of heterotopic pregnancy increases from 1 per 4000 to 1 per 100.33
Most ectopic pregnancies occur in the fallopian tube. Eighty percent occur in the ampulla of the fallopian tube, 12% in the isthmic segment, 5% in the fimbria, and 2% in the corneal/interstitial region. Ectopic pregnancies occurring in nontubal sites are rare, with 1.4% in the abdomen and 0.2% in the ovary and cervix.36
Classically, ectopic pregnancy presents with the triad of vaginal bleeding, abdominal bleeding, and amenorrhea. Other signs and symptoms include tachycardia and hypotension secondary to rupture and hemorrhage, and shoulder pain secondary to diaphragmatic irritation caused by hemoperitoneum. It is imperative to remember that the patient may not report having missed her period.
Pelvic examination may reveal cervical motion tenderness and an adnexal mass; however, the physical examination has never been proven to be useful in ruling out ectopic pregnancy. In fact, almost 50% of patients who were found to have an ectopic pregnancy in one review had benign physical findings on first presentation.37
The most important laboratory test in a woman of childbearing age with pelvic pain is urine qualitative beta-hCG measurement. A positive test correlates with a serum beta-hCG level of approximately 10 to 50 mIU/mL, and 90% of pregnancies can be diagnosed on the first day of the missed menstrual period.38 False-negative results occur when the beta-hCG level is less than 50 mIU/mL, usually as a result of dilute urine or testing too soon after ovulation. Under these conditions, the urine pregnancy test would miss only 1 in 2000 ectopic pregnancies, most of which would be too small to be dangerous.
Serum beta-hCG can be measured qualitatively or quantitatively, and the test can detect a beta-hCG level as low as 3 mIU/mL. There is minimal difference in sensitivity compared to urine testing; however, serum beta-hCG measurement is helpful in highly suspicious cases with a negative urine test. The most useful aspect of the quantitative test is that it is helpful in interpreting ultrasound results and in following patient progress.
Classically, it has been taught that the serum beta-hCG level doubles every 48 hours in early viable pregnancies. Studies have shown that the hCG concentration rises by at least 66% every 48 hours during the first 40 days of pregnancy in 85% of viable intrauterine pregnancies.39 More recently, it has been shown that a rise of 53% every 2 days can be seen in potentially viable pregnancies.40 While the beta-hCG level can vary among viable pregnancies, 71% of ectopic pregnancies have serial serum hCG values that increase more slowly than expected with a viable intrauterine pregnancy or decrease more slowly than expected with a miscarriage.33

The discriminatory beta-hCG zone is defined as the serum hCG level above which a gestational sac should be visualized by ultrasound examination if an intrauterine pregnancy is present.39 The gestational sac is the first structure of a pregnancy that can be visualized via ultrasound (at about 4.5 to 5 weeks). It is visible on transvaginal ultrasonography when the quantitative beta-hCG level is above 1500 mIU/mL, while on transabdominal ultrasonography it is visible with levels above 6500 mIU/mL. Ultrasound findings and their corresponding beta-hCG levels in a viable intrauterine pregnancy are listed in Table 2.
During the evaluation for a possible ectopic pregnancy, a quantitative beta-hCG measurement and a transvaginal ultrasound scan should be obtained. There is no need to wait for the quantitative beta-hCG results before obtaining the ultrasound scan. In symptomatic patients, it is possible to diagnose up to one-third of ectopic pregnancies even with a beta-hCG level of less than 1000 mIU/mL.41
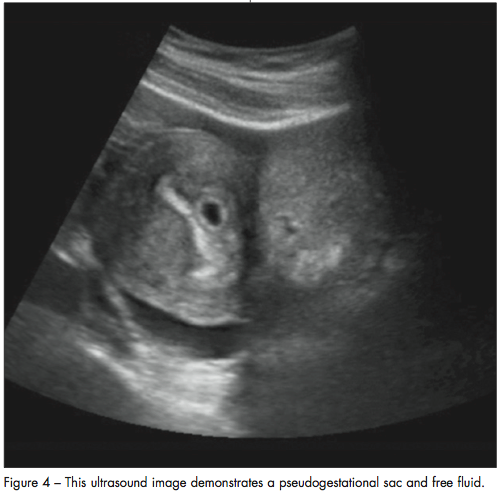
Beta-hCG above the discriminatory zone (higher than 1500 mIU/mL). The finding of a gestational sac on an ultrasound scan is suggestive but not completely diagnostic of an intrauterine pregnancy. This is because the gestational sac can be confused with a pseudogestational sac, which is an endometrial fluid collection often associated with an ectopic pregnancy.36 The pseudogestational sac is seen in 10% to 20% of ectopic pregnancies (Figure 4).42
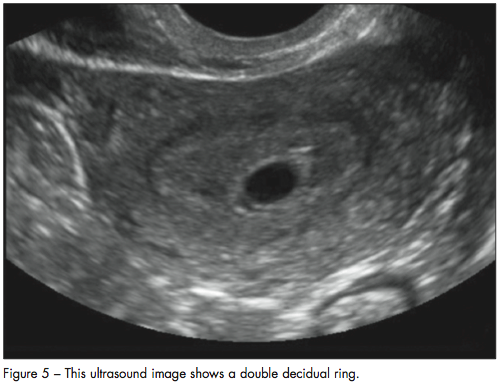
The double decidual ring, two echogenic rings around the gestational sac, is seen slightly later in pregnancy (Figure 5). In the radiology literature, it is considered highly reliable for the diagnosis of an intrauterine gestational sac and is pathognomonic for an early intrauterine pregnancy.43,44 Visualization of the double decidual ring helps differentiate the gestational sac from a pseudogestational sac. However, the double decidual ring has only a short window in which to be visualized and is not consistently seen.43,44 Furthermore, the double decidual ring can be difficult for clinicians who are not expert radiologists to identify correctly, leading to the incorrect diagnosis of an intrauterine pregnancy.42 Therefore, definitive evidence of an intrauterine pregnancy includes visualization of a yolk sac within the gestational sac, visualization of a fetal pole, or cardiac activity. This will exclude an ectopic pregnancy unless a heterotopic pregnancy is suspected.
Definite evidence of an ectopic pregnancy includes visualization of an extrauterine sac containing a yolk sac, fetal pole, or cardiac activity. This, however, is seen in only 16% to 32% of ectopic pregnancies. Other findings that raise concern for an ectopic pregnancy include an empty uterus with tubal ring, complex adnexal mass, or moderate to large free fluid. All these scenarios mandate consultation with an obstetrician-gynecologist.42
Approximately 10% to 20% of patients who are evaluated for ectopic pregnancy will have a non-diagnostic scan. These patients include those with an empty uterus without any evidence of an extrauterine pregnancy. This scenario is indicative of an ectopic pregnancy or a nonviable pregnancy. However, it is possible that multiple gestations are present, causing an inability to visualize the gestation sac despite a beta-hCG level higher than 1500 mIU/mL.45 It is also possible that the gestation sac or ectopic pregnancy was not visualized because of suboptimal pelvic ultrasound imaging. These patients must have close follow-up with a repeated ultrasound scan, beta-hCG measurement, and clinical examination within 48 hours. Because of the concern for possible rupture of an unidentified ectopic pregnancy, this plan should be made in conjunction with an obstetrician-gynecologist.
Beta-hCG below the discriminatory zone (less than 1500 mIU/mL). While it is possible to detect a gestational sac or findings that raise concern for an ectopic pregnancy in a patient with a beta-hCG level lower than 1500 mIU/mL, such patients often have normal pelvic ultrasound scans. The differential in this situation includes ectopic pregnancy, early intrauterine pregnancy, and nonviable pregnancy. These patients should be followed every 48 to 72 hours with repeated beta-hCG testing. When the level is lower than 1500 mIU/mL, an ultrasound scan should be performed to evaluate for a gestation sac. An abnormally rising or falling beta-hCG level suggests an abnormal pregnancy or failed pregnancy, respectively.39
Some obstetrician-gynecologists employ progesterone tests to help differentiate normal from abnormal pregnancies. Very low values (less than 5 ng/mL) are predictive of abnormal pregnancy in 97% to 100% of patients. High values (greater than 25 ng/mL) are predictive of normal pregnancy in 97% of patients. Unfortunately, intermediate values are not helpful in evaluation.
Treatment. Surgery (most often laparoscopic) is indicated for hemodynamically unstable patients, patients who fail medical therapy, or for those patients who are not candidates for medical therapy.
Methotrexate, a folate antagonist, can be used for medical treatment of ectopic pregnancies. It may be used in stable and reliable patients with an empty uterus, an ectopic mass smaller than 3.5 to 4 cm, no fetal cardiac activity on ultrasound, and a beta-hCG level of less than 5000 mIU/mL. A beta-hCG level higher than 5000 mIU/mL portends a significant increase in treatment failure, and such patients may benefit from a multi-dose regimen.33,46 If the patient is stable and the ectopic pregnancy appears to be resolving, serial examinations and observation may be elected.
LESSONS FROM THIS CASE
•Do not rely on a recent normal menstrual period to rule out pregnancy.
•All women of childbearing age with abdominal pain should have a pregnancy test.
•Do not treat colleagues differently from other patients and try to spare them important elements of the physical examination; your favor could be a serious medical mistake.
1. Colucciello SA, Lukens TW, Morgan DL. Assessing abdominal pain in adults: a rational, cost-effective, and evidence-based strategy. Emerg Med Pract. 1999;1:1-20.
2. Adams ID, Chan M, Clifford PC, et al. Computer-aided diagnosis of acute abdominal pain: a multicentre study. Br Med J (Clin Res Ed). 1986;293:
800-804.
3. Lewis LM, Banet GA, Blanda M, et al. (). Etiology and clinical course of abdominal pain in senior patients: a prospective, multicenter study. J Gerontology. Series A, Biological Sciences and Medical Sciences. 2005;60(8):1071-1076.
4. van Geloven AA, Biesheuvel TH, Luitse JS, Hoitsma HF, Obertop H. (). Hospital admissions of patients aged over 80 with acute abdominal complaints. Eur J Surgery.2000;166(11):866-871.
5. Medscape. Acute mesenteric ischemia. http://emedicine.medscape.com/article/189146.
6. Glenister KM, Corke CF. Infarcted intestine: a diagnostic void. ANZ J Surgery. 2004;74(4):260-265.
7. Lange H, Jäckel R. Usefulness of plasma lactate concentration in the diagnosis of acute abdominal disease. Eur J Surg. 1994;160:381-387.
8. Klein HM, Lensing R, Klosterhalfen B, et al. Diagnostic imaging of mesenteric infarction. Radiology. 1995;197:79-83.
9. UpToDate. Acute mesenteric ischemia. http://www.uptodate.com/contents/acute-mesenteric-ischemia.
10. Taourel PG, Deneuville M, Pradel JA, et al. Acute mesenteric ischemia: diagnosis with contrast-enhanced CT. Radiology. 1996;199:632-637.
11. Ofer A, Abadi S, Nitecki S, et al. Multidetector CT angiography in the evaluation of acute mesenteric ischemia. Eur Radiol. 2009;19:24-29.
12. Barmase M, Kang M, Wig J, et al. Role of multidetector CT angiography in the evaluation of suspected mesenteric ischemia. Eur J Radiol. 2011;80(3):e582-e587.
13. Kassahun WT, Schulz T, Richter O, Hauss J. Unchanged high mortality rates from acute occlusive intestinal ischemia: six year review. Langenbeck’s
Archives Surgery. 2008;393(2):163-171. doi:10.1007/s00423-007-0263-5
14. Regan F, Karlstad RR, Magnuson TH. Minimally invasive management of acute superior mesenteric artery occlusion: combined urokinase and laparoscopic therapy.Amer J Gastroenterol. 1996;91:1019-1021.
15. American College of Radiology. ACR Appropriateness Criteria: Acute Onset Flank Pain — Suspicion of Stone Disease. http://acsearch.acr.org/
16. Smith JE, Hall EJ. The use of plain abdominal x rays in the emergency department. Emerg Med Journal. 2009;26(3):160-163.
17. Baker SR. The abdominal plain film. What will be its role in the future? Radiol Clin North Am. 1993;31:1335-1344.
18. Sandhu C, Anson KM, Patel U. Urinary tract stones—part I: role of radiological imaging in diagnosis and treatment planning. Clin Radiol. 2003;
58:415-421.
19. McCook TA, Ravin CE, Rice RP. Abdominal radiography in the emergency department: a prospective analysis. Ann Emerg Med. 1982;11(1):7-8.
20. Singh K, Bonaa KH, Jacobsen BK, et al. Prevalence and risk factors for abdominal aortic aneurysm in a population-based study: the Tromso Study. Am J Epidemiol.2001;154:236-244.
21. UpToDate Online. Clinical evaluation of abdominal aortic aneurysm. http://www.uptodate.com/contents/clinical-evaluation-of-abdominal-
aortic-aneurysm
22. Bentz S. Accuracy of emergency department ultrasound scanning in detecting abdominal aortic aneurysm. Emerg Med Journal. 2006;23(10):
803-804.
23. Costantino T, Bruno E, Handly N, Dean A. Accuracy of emergency medicine ultrasound in the evaluation of abdominal aortic aneurysm. J Emerg Med.2005;29(4):455-460.
24. Blaivas M, Theodoro D. Frequency of incomplete abdominal aorta visualization by emergency department bedside ultrasound. Acad Emerg Med. 2004;11(1):103-105.
25. American College of Radiology. ACR Appropriateness Criteria: Pulsatile Abdominal Mass, Suspected Abdominal Aortic Aneurysm. http://acsearch.acr.org/
26. Ernst CB. Abdominal aortic aneurysm. N Engl J Med. 2012;328(16):1167-1172.
27. Visser P, Akkersdijk GJ, Blankensteijn JD. In-hospital operative mortality of ruptured abdominal aortic aneurysm: a population-based analysis
of 5593 patients in the Netherlands over a 10-year period. Eur J Vasc Endovasc Surg. 2005;30:359-364.
28. Satta J, Laara E, Reinila A, et al. The rupture type determines the outcome for ruptured abdominal aortic aneurysm patients. Ann Chir Gynaecol. 1997;86:24-29.
29. Robinson D, Englund R, Hanel KC. Treatment of abdominal aortic aneurysm in the 9th and 10th decades of life. Aust N Z J Surg. 1997;67:640-642.
30. Hechelhammer L, Lachat ML, Wildermuth S, et al. Midterm outcome of endovascular repair of ruptured abdominal aortic aneurysms. J Vasc Surg. 2005;41:752-757.
31. Hinchliffe RJ, Bruijstens L, MacSweeney ST, et al. A randomized trial of endovascular and open surgery for ruptured abdominal aortic aneurysm - results of a pilot study and lessons learned for future studies. Eur J Vasc Endovasc Surg. 2006;32(5):506-513; discussion 514.
32. Giles KA, Pomposelli FB, Hamdan AD, Wyers MC, Schermerhorn ML. Comparison of open and endovascular repair of ruptured abdominal aortic aneurysms from the ACS-NSQIP 2005-07. J Endovascular Therapy. 2009;16(3):365-372.
33. Barnhart KT. Clinical practice. Ectopic pregnancy. N Engl J Med. 2009;361(4):379-387.
34. Chang J, Elam-Evans LD, Berg CJ, et al. Pregnancy related mortally surveillance—United States, 1991–1999. MMWR Surveillance Summaries. 2003;52:1-9.
35. Ankum WM, Mol BW, van der Veen F, Bossuyt PMM. Risk factors for ectopic pregnancy: a meta-analysis. Fertil Steril. 1996;65:1093-1099.
36. Medscape. Ectopic pregnancy. http://emedicine.medscape.com/article/258768-overview
37. Stovall TG, Kellerman AL, Ling FW, Buster JE. Emergency department diagnosis of ectopic pregnancy. Ann Emerg Med. 1990;19(10):1098-1103.
38. Wilcox AJ, Baird DD, Dunson D, et al. Natural limits of pregnancy testing in relation to the expected menstrual period. JAMA. 2001;286:1759-1766.
39. UpToDate. Clinical manifestations, diagnosis, and management of ectopic pregnancy. http://www.uptodate.com/contents/clinical-manifestations-diagnosis-and-management-of-ectopic-pregnancy.
40. Barnhart KT, Sammel MD, Rinaudo PF, et al. Symptomatic patients with an early viable intrauterine pregnancy: HCG curves redefined. Obstet Gynecol. 2004;104:50-54.
41. Dart RG, Dart L, Mitchell P, Berty C. The predictive value of endometrial stripe thickness in patients with suspected ectopic pregnancy who have an empty uterus at ultrasonaography. Academic Emerg Med. 1999;6:602-609.
42. Medscape. Emergent management of ectopic pregnancy. http://emedicine.medscape.com/article/796451
43. Medscape. Ultrasound imaging in the diagnosis of ectopic pregnancy. http://emedicine.medscape.com/article/104382
44. Levine D. Ectopic pregnancy. Radiology. 2007;245(2):385-397. doi:10.1148/radiol.2452061031
45. Kadar N, Bohrer M, Kemmann E, Shelden R. The discriminatory human chorionic gonadotropin zone for endovaginal sonography: a prospective, randomized study.Fertil Steril. 1994;61(6):1016-1020.
46. Menon S, Colins J, Barnhart KT. Establishing a human chorionic gonadotropin cutoff to guide methotrexate treatment of ectopic pregnancy: a systematic review. Fertil Steril. 2007;87(3):481-484.


